Narrative/Systematic Reviews/Meta-Analysis
Medicare telehealth pre- and post-COVID-19: interstate framework, regulations, licensure, and HIPAA
Sophia Albanese, BA1  ; Amar Gupta, PhD2*
; Amar Gupta, PhD2*  ; Ilina Shah, BS, BA3
; Ilina Shah, BS, BA3  and Joanna Mitri, MD, MS4,5
and Joanna Mitri, MD, MS4,5 
1Rutgers University, New Brunswick, NJ, USA; 2MIT, Cambridge, MA, USA; 3University of Massachusetts, Amherst, MA, USA; 4Joslin Diabetes Center, Boston, MA, USA; 5Harvard Medical School, Cambridge, MA, USA
Abstract
The coronavirus disease-2019 (COVID-19) pandemic led to temporary relaxations for telehealth with respect to physician licensure, geographic location, and eligible sites for reimbursement. Earlier policies had impacted the rate of adoption of telehealth services and hindered the ability to derive full benefits related to cost, access to care, and quality of care. This aspect is analyzed using 2018 Medicare fee-for-service codes and rates for 10 telemedicine services. Based on the data analysis, additional research, and a literature review, this report describes how interstate practices can be better leveraged to achieve maximum potential for direct and indirect savings from pragmatic approaches for certain services. The interstate collaborations proposed in this report provide examples of broader telehealth policies that could foster increasing access to quality healthcare for Medicare beneficiaries and can potentially be used as insight to assist federal and state agencies as they review the continuation, cessation, or modifications of relaxations granted due to the COVID-19 pandemic.
Keywords: Medicare; telemedicine; medical licensure; interstate; cost-savings; patient privacy; COVID-19
Citation: Telehealth and Medicine Today 2021, 6: 299 - http://dx.doi.org/10.30953/tmt.v6.299
Copyright: © 2021 The Authors. This is an open access article distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, and enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See http://creativecommons.org/licenses/by-nc/4.0.
Published: 18 November 2021
Competing interests and funding: No conflicts of interest exist pertaining to this manuscript.
The authors have not received any funding or benefits from industry or elsewhere to conduct this study.
Corresponding Author: *Amar Gupta, Email: agupta@mit.edu
POLICY POINTS
- Multiple barriers related to physician licensure, geographic location, and eligible sites for Medicare coverage of interstate practice of telemedicine were temporarily lifted to address the COVID-19 pandemic. These reimbursement and other issues are analyzed in the context of potentially extending the relaxations, ending the temporary relaxations, or taking a hybrid or other approaches.
- This report argues that the Medicare coverage of interstate telehealth during the COVID-19 pandemic should be extended, in conjunction with incorporating adequate safeguards to ensure confidentiality of patient health information, patient safety, and physician accountability, with special provisions restricting involvement in Medicare-funded telemedicine practice by doctors and other medical personnel disbarred or disciplined in one or more states.
- The analyses within this report highlight an example of cost comparison of procedural codes between different states for telemedicine services.
The wider adoption of telemedicine could potentially help address the paradox of the United States spending the largest amount of money per capita on health care versus its healthcare system being ranked in the bottom half of all developed countries.1,2 The Center for Information Technology Leadership has estimated that the increased adoption and use of telemedicine could lead to an annual savings of $4.28 billion in the US healthcare system.3 Another study estimated that synchronous audio–video on-demand telemedicine could result in a net cost savings of $19–121 per visit.4 Telemedicine in US hospitals increased from 42% in 2012 to 76% in 2017, and significantly more as a result of the coronavirus disease-2019 (COVID-19) pandemic and the Coronavirus Aid, Relief, and Economic Security (CARES) Act.5,6 The barriers to a widespread adoption of telemedicine include reimbursement rates for providers, medical licensure laws, patient privacy, and geographic restrictions.
While virtual health care offers the potential for doctors to practice across state lines, traditional laws have deemed interstate medical practice to be illegal without obtaining a license from each state in which the physician’s patients are located.7 Previous research studies on interstate practice of telemedicine concluded that these barriers to the interstate practice of telemedicine were likely unconstitutional as they violated the interstate commerce clause of the United States Constitution.8 In 2018, 7 years after the aforementioned research was published, the US Department of Veterans Affairs (VA) launched a nationwide campaign to market and implement the notion of ‘anywhere to anywhere’ practice of telemedicine within the US, enabling streamlined interstate and in-home telemedicine services for US veterans.9
As part of the larger objective to study the implications of adopting a similar interstate telemedicine strategy for the civilian sector, this report begins with a cost comparison of procedural codes (Current Procedural Terminology [CPT] and Healthcare Common Procedure Coding System [HCPCS]) and uses publicly available data compiled from Medicare’s 2018 telemedicine fee-for-service codes to estimate the potential cost savings through potential interstate telemedicine practices, fewer geographic restrictions, and streamlined licensing regulations.
DATA AND METHODS
Rates were analyzed using the Centers for Medicare & Medicaid Services (CMS) Physician Fee Schedule Lookup Tool, available online at the Center for Medicare & Medicaid Services website (cms.gov).10 The analysis was conducted across all 50 states and the District of Columbia using the following parameters within the CMS Lookup Tool:
Year: 2018
Type of Information: Pricing Information
Select Health Care Common Procedure Coding System (HCPCS) Criteria: Single HCPCS Codes
Select Medicare Administrative Contractor (MAC) Option: All MACs
Modifier: All Modifiers
From this list, 10 codes were chosen for further analysis. These codes covered a range of telemedicine-only procedures, as well as procedures that can be done with or without telemedicine. In accordance with CMS’s rules on telemedicine, these services involved ‘interactive audio and video telecommunications systems that permit real-time communication’ between the healthcare professional and the beneficiary.11 The codes were processed through the Lookup Tool, which generated 113 groupings of reimbursement rates based on the 113 different MACs in 2018.
For each of the 10 codes studied, the average, maximum, and minimum rates were recorded from the CMS Lookup Tool for all MACs, both facility and non-facility. Traditionally, Medicare reimbursed for telemedicine services only if they are rendered at specific originating site locations, defined as ‘the location of an eligible Medicare beneficiary at the time the service furnished via a telecommunications system occurs’.12 The Medicare Final Rule from 2018 limited the geographic qualifications for an originating site to those within rural Health Professional Shortage Areas (HPSAs) or in a county that was not included in a Metropolitan Statistical Area (MSA).13 These restrictions mandated that telemedicine services were reimbursable only if the patient was located in a rural HPSA or non-MSA.
The Medicare Physician Fee Schedule includes both facility and non-facility fees. Facilities include hospitals, nursing homes, and other sites, while non-facility sites include places such as a physician’s office.14 Under CMS’s rules for telemedicine, a valid originating site can include a variety of both facility and non-facility locations.13 Regardless of whether the patient is at a facility or non-facility originating site, the added originating site fee remained the same at a flat rate of $25.76 in 2018.15 For the purpose of this study, the originating site charge of $25.76 was not included in the values examined, as it remains the same for all codes and does not impact the overall cost-difference analyses.
STUDY RESULTS
The rates for each procedural code varied by state and region within the state. The minimum fees across all states for facility and non-facility consistently corresponded to the state of Mississippi for the services specified in Table 1. The maximum facility and non-facility fees corresponded to the state of Alaska. Using these two extremes, the following table exhibits the opportunity for cost savings if an interstate telehealth system were to be implemented between Alaska and Mississippi. Table 1 summarizes the potential cost savings for facility and non-facility fees if Alaskan residents were to utilize telehealth services provided by practitioners in Mississippi rather than in Alaska. The percentage difference (% Diff) has been defined as the absolute value of the difference in the two fees divided by the average of these two fees.
The average cost savings in each scenario range from $28.07 to $41.02, with a percent difference of 26.9-46.2%. The highest average cost savings occurs when an Alaskan patient switches from a physician at an Alaskan non-facility to a physician at a Mississippi facility. This scenario also has the highest relative cost saving for a single procedure, with a 76.9% difference in cost for New Office or Outpatient Visits (99201) between Alaska and Mississippi. Out of all the scenarios, costs increase only for one procedure – Office or Outpatient Visit, New (99201) – when physicians in a Mississippi non-facility location are used instead of physicians in Alaskan facilities. Figure 1 presents the maximum cost saving scenario observed from Table 1, when a patient receives care from a Mississippi physician within a facility via telehealth, rather than from an Alaskan physician within a non-facility location.
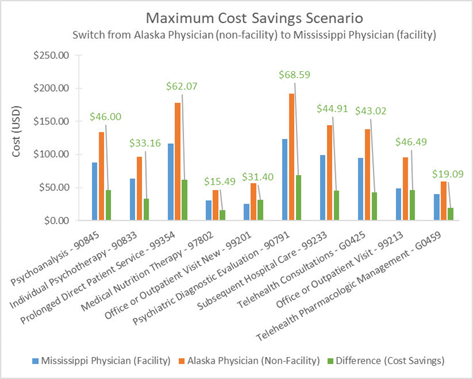
Figure 1—Maximum cost savings scenario: Alaska physician (non-facility) to Mississippi physician (facility). Source: Authors’ analysis of data from the CMS Physician Fee Schedule.
Another high-cost MAC, Queens, New York, shows a similar potential benefit for an interstate system. The average cost savings when a Queens patient utilizes Mississippi physicians range from $8.53 to $22.02, corresponding to a percentage difference of 7.6–29.3%. The scenario with highest average cost savings occurs when a Queens patient switches from using a physician based in a Queens non-facility to a physician in a Mississippi facility. As in the case of Alaska and Mississippi, this describes a switch from the costliest location type within the more expensive state to the least costly location type within the least expensive state. This scenario has the highest absolute cost saving for a single procedure, with $37.45 saved for office or outpatient visit (99213). In addition, it has the highest relative cost saving for a single procedure, with a 72.1% difference in cost for New Office or Outpatient Visit (99201). Of all the scenarios, costs increase only for two procedures – new and non-new office or outpatient visit (99201, 99213) – when physicians in Mississippi non-facility locations were used instead of physicians in Queens facilities.
Discussion
Summary
Mississippi has the lowest rates and Alaska has the highest rates under Medicare fee-for-service. In fact, the cost of healthcare in Alaska is twice the national average.16 Alaska’s high rates may be attributed to a lack of competition among providers, lack of specialists, the state’s small population, and the remote living conditions of many patients in Alaska.17 As of June 2019, 98,519 Alaskans were enrolled in Medicare.18 Table 1 leads to the conclusion that for the services specified in the study, Alaska-based Medicare could save an average of $34.55 per procedure by allowing patients to receive care from practitioners in Mississippi through an interstate telehealth collaboration.
Implications
An overly active interstate network would lead to diminished revenues for Alaskan healthcare professionals, possibly resulting some of them relocating to other states. The 2018 report, Information on Medicare Telehealth, by the Centers for Medicare and Medicaid Services found that rural areas, like much of Alaska, were characterized by an average of 30 specialists per 100,000 residents, compared with 263 specialists in urban areas.15 The report also stated that 93% of rural patients who utilized telehealth saved a trip to a clinic for after-hours treatment and 86% saved a trip to the emergency room.15 An interstate telehealth system could alleviate issues surrounding the lack of medical professionals within the patient’s home state.
Physician quality and access
Expanding telehealth practice across state lines can improve the health of doctors in hospitals and other specialties requiring night shifts. The article ‘Whatever you Do, Don’t Get Sick at Night’ explains that doctors avoid working night shifts because of the negative effects it places on their circadian rhythms and the difficulty in spending time with family and friends.19 Several studies confirm that night shifts may increase workers’ risks of cancer, cardiovascular disease, and other health complications.20,21 Issues, such as fatigue and sleep deprivation, impact the quality of work of healthcare professionals, thereby adversely impacting the quality of care provided to patients. To combat this issue, hospitals are gradually embracing the concept of physicians working during the day in one location to monitor patients throughout the night at another location via telemedicine.22,23 Emory University in Atlanta, Georgia, partnered with Royal Perth Hospital in Australia, to form two distributed teams to work in the eICU Center, one in Atlanta and the other in Perth. The 12-h time difference allows Emory’s eICU patients to be monitored around the clock, while allowing healthcare professionals in both continents to work during the day and receive adequate and regular rest at night.24 This concept can be considered for use within the United States too, where time zone differences are as large as 6 h between states.
Another benefit associated with interstate telemedicine collaborations is increased access to specialist services. Alaskan Medicare beneficiaries face barriers when accessing necessary services and providers due to low reimbursement rates to providers, which dissuades medical professionals from accepting new Medicare patients.25 Medicaid patients have faced a similar lack of care due to historically low reimbursement rates through Medicaid, which has prompted a similar research on the expansion of interstate policies for Medicaid beneficiaries.26 Data from private insurers in Alaska show that in-network specialist services can cost 10 times more in Anchorage than in other cities.26 Thus, in comparison with what they can earn in the private market, medical specialists residing in Alaska may be less inclined to treat Medicare patients at lower reimbursement rates. A Pew Research study revealed that that the expanded telehealth available during the COVID-19 pandemic played a crucial role in the treatment of patients with opioid use disorder, especially patients in rural areas who previously struggled to receive adequate care.27 Telemedicine across state lines offers a pragmatic mechanism for addressing this dilemma, as patients would have an increased access via telehealth to consult specialists in other states, especially when there is a lack of access to a certain specialty within their home state.
In addition to supporting physician well-being and increasing access to care, telemedicine offers a unique avenue to limit patient harm that may otherwise occur in the in-person setting. The COVID-19 pandemic provides a clear example of the role played by telehealth in reducing human contact, and therefore, reducing the risk of contracting additional infections.28,29 Outside of pandemics, healthcare-related infections represent approximately 1.7 million infections per year and nearly 99,000 deaths.30 Additional studies have shown that as much as 40% of infections that originate in hospitals are a result of cross-infections from contaminated surfaces transmitted via medical professionals to patients.31
Time and cost savings
Time and cost benefits related to travel can serve as a major source of savings when using telemedicine.32 The Texas Department of Criminal Justice saw transportation expenses related to medical services for their inmates decrease by $350 per visit when they began using telehealth, resulting in a savings of over $3 million in 1 year.33 The VAs healthcare system projected transportation costs for veterans to and from VA medical facilities at about $1 billion in 2015.34 As a result of using telemedicine, the VA reduced travel distance and time by an average of 145 miles and 142 min per visit from 2005 to 2013, leading to a yearly savings of $63,804 in 2013.34
Time-related savings via telemedicine are applicable in both rural and urban areas. The urban city of Los Angeles is ranked as the most traffic-congested city in the United States.35 A research study showed that ‘Angelenos spent an average of 102 h [in 2016] in traffic jams during peak congestion hours, costing drivers $2,828 each and the city $19.2 billion’. Recent research on postoperative pediatric care concluded that that travel and wait time constituted 98.4% of total time for in-person visits, which, in turn, led to in-person visits being characterized by an opportunity cost of $23.75 per minute versus $1.14 in the case of a virtual visit.36
Geographic limitations
There are wide disparities in healthcare utilization and outcomes between rural and urban residents. Because Medicare has limited the originating site solely to rural HPSAs, telehealth services provided in highly populated urban areas were ineligible for reimbursement.13 A 2017 Health Affairs blog highlighted how ‘Medicare payment policies target geography, and therefore do not focus on the real problem, which is access’.37 A 10-state study of 11,347 patient calls found that while rural patients were offered appointments 80% of the time, urban patients were offered appointments only 60% of the time. Furthermore, 69% of uninsured rural patients said they had a regular source of care compared with only 51% of uninsured urban patients. Also, 21% of rural patients said that they had delayed care compared with 32% of urban patients who felt they had delayed care.37 Access to care is usually presented as a problem only for rural areas; however, data suggest that urban areas should not be left out of the conversation.38 A study analyzing 203 orthopedic practices in North Carolina revealed that rural practices were 8% more likely than urban practices to offer appointments to Medicaid patients.38
Based on the above information, reimbursement policies could incorporate restrictions based on access to care, not on geography. Reimbursing telemedicine in urban areas would likely result in an increase in the use of telemedicine.39 This may increase quality of care through treatment at earlier stages of diseases. A 2019 study of synchronous telemedicine visits found that 16% of 650 patients would have ‘done nothing’ if they did not have access to telemedicine. Moreover, 74% of the patients saw their issues resolved via the telemedicine visit.4
Apart from the temporary relaxations granted during the COVID-19 pandemic, precedents exist within Medicare for waivers of geographic restrictions to foster better access to care for certain beneficiaries. CMS removed originating site geographic restrictions for practitioners furnishing monthly home dialysis end-stage renal disease (ESRD) related medical evaluations to hospital-based and critical access hospital (CAH) based renal dialysis centers, renal dialysis facilities, and beneficiary homes.12 In addition, with the passing of the Bipartisan Budget Act in 2019, several originating site limitations were lifted for patients seeking diagnosis, evaluation, or treatment of an acute stroke.13
State preference for local procurements
The debate on interstate service provision exists in many sectors other than health care. One of the examples is preference given to local bidders by state governments in awarding contracts for products and services. Such policies are praised by some observers for creating more local jobs and ensuring that tax revenues are reinvested within the state. Others criticize this structure for potentially stifling vendor competition, reducing the incentive for local businesses to provide the best quality, and placing a financial burden on taxpayers.40 Currently, 37 states have reciprocal laws, which require public contracting agencies to add a percent increase to every out-of-state business’s bid price equal to the percent of preference given to local businesses by the other state.41
Local procurement policies in Alaska dictate that a ‘5.0% preference is applied to the price in the bid of an Alaska bidder’ and a ‘15% preference is applied to the price in the bid of an Alaskan bidder offering services through an employment program’.42 This tilts the balance in favor of in-state companies.
If these local preference laws were extended to telehealth, services rendered by physicians in Mississippi would still cost less than the rates payable to Alaskan physicians for nine of the 10 codes analyzed. Furthermore, it should be noted that the federal government does not allow states to implement local preference laws on projects funded by federal dollars.43 Because Medicare is federally funded, one could argue that local preference laws are not applicable when considering interstate telehealth services funded by Medicare.44
COVID-19
On January 31, 2020, the United States Secretary of Health and Human Services declared the COVID-19 pandemic a public health emergency.45 The Trump administration passed The CARES Act that temporarily removed long-standing restrictions on the use of telehealth services for the Medicare population.46 The patient’s home became an eligible originating site, enabling patients to receive care without leaving their home and providers being reimbursed at the rate as if the visit occurred in person. In addition, physicians became temporarily free to practice telehealth in any US state regardless of their licensure. The CARES Act also made it possible for Medicare beneficiaries to receive care from a physician without having a prior relationship with that doctor, increasing access to care during stay-at-home orders.46
In a June 2020 letter to Congress, healthcare leaders highlighted that the changes to telehealth policy during the COVID-19 pandemic ‘allowed 46 percent of Americans to replace a cancelled healthcare visit with a telehealth service’.47 Among the four critical issues addressed in the letter, the authors urged policymakers to remove restrictions on the location of the patient to allow both rural and urban Medicare beneficiaries to be eligible to receive telehealth services.47
In the array of related bills introduced in Congress since the pandemic, the Advancing Telehealth Beyond COVID-19 bill aims to keep the barriers low for Medicare beneficiaries to receive telehealth beyond the COVID-19 pandemic.48 The bill proposes the removal of originating site and geographic limitations for telehealth under Medicare. The common goal of these bills is to ensure that Medicare beneficiaries have an increased access to quality care at an affordable cost via telemedicine.48
The private insurer ecosystem shows mixed reactions toward maintaining COVID-related relaxations after the pandemic. The Blue Cross Blue Shield of Tennessee has stated that telehealth claims submitted during COVID-19 have been 18 times greater than that in 2019, and that it will continue its in-network coverage of telehealth permanently.49 In contrast, several other private insurance companies plan to return to pre-COVID procedures.49
Any continuation of pandemic-related telehealth relaxations needs to be objectively analyzed in terms of the impact on the clinical outcome and quality of care. A recent study of outpatient cardiovascular telemedicine care during the pandemic shows that racial, gender, income, and age inequities were actually compounded compared with in-person treatment.50 By virtue of being based in technology, telehealth creates a digital divide between racial and socioeconomic groups, and the populations lacking digital literacy tend to correlate with older, less educated, people of color.51,52 Furthermore, children of color are 16% less likely to have computer access in their homes compared with white children.51
Licensing of physicians and privacy of patient records
One of the most commonly noted barriers to telehealth is physician licensure, leading to the consideration of diverse options, including multi-state licenses, mutual recognition of individual licenses across states, and federal licenses (53–55). While the Interstate Medical Licensure Compact has paved the way for increased interstate collaboration to increase the use of telemedicine, still fewer than 30 states are involved.56 Furthermore, the Interstate Medical Licensure Compact does not eliminate the need for a physician to apply in every state where his or her patients may be. It just facilitates those applications.
One of the solutions to licensure barriers is for the federal government to play the lead role in telemedicine licensure.57The VAs policy on interstate licensure serves as a precedent.9 Another is to emulate the example of the drivers’ license, which is issued at the state level, yet allows licensed drivers to drive in any state in the United States.58 Abroad, Canada is considering a national physician license.59 Australia has already implemented a national license and has received criticism for it being created too quickly without addressing flaws related to cost of licensure and inadequate treatment of physician misconduct.60,61
Physician misconduct requires attention when formulating an interstate licensure framework. When a physician has committed an act that requires disciplinary action, the medical board within the concerned state or territory can restrict the physician’s license to varying extents, most severely by revoking the license entirely, banning the physician’s practice of medicine in that state.62 Cases of doctors losing a license in one or more states and later obtaining a license in another state and continuing to practice medicine raise serious concerns.63,64 A study revisited the outcomes of cases where physicians had been disciplined for sexual misconduct toward patients, and it was concluded that 39.9% of these physicians continued to be licensed in ‘1 or more of the jurisdictions that originally sanctioned them’.65 This disparity in state laws on medical licensure should be addressed prior to implementing a permanent interstate system that relies on a robust nationwide list of doctors who have been disbarred or otherwise disciplined.
Interstate practice of telemedicine also raises issues related to Health Insurance Portability and Accountability Act of 1996 (HIPAA) and patient privacy. Concerns include confidentiality regulations that lack standards and clarity regarding patient consent, ownership of data, as well as the patients’ role in determining how their data can be utilized, and the potential creation of a nationwide standard for electronic record (66–68). When the US federal government announced the temporary lifting of restrictions related to telemedicine, the media highlighted that doctors could treat patients located anywhere in the country, and that medical records could be freely transferred, as violations of HIPAA would not be prosecuted.69 Under HIPAA, ‘state laws that are contrary to the federal law will be preempted by HIPAA’, meaning that if the state’s privacy laws are different than the federal law, then the federal law will be used, except in the case where the state law is more stringent than the federal law.70,71 The unilateral temporary suspension of federal HIPAA regulations meant that the diverse array of dissimilar state laws became fully applicable, thereby creating confusion and increasing the barrier for physicians to assist patients located in other parts of the country. Gradually, the state governments followed the example set by the federal government in suspending their respective regulations. However, this sets a dangerous precedent for potential misuse of patient information and violation of privacy of pictorial, numerical, and textual data. At the minimum, a baseline of standards should apply during and after the COVID-19 pandemic to provide confidence to patients about ensuring adequate patient privacy in interstate telehealth services provided with the assistance of electronic health information exchanges and other traditional and innovative mechanisms.72
CONCLUSION
Telehealth has been a major actor in mitigating the COVID-19 pandemic in the United States, partly because several barriers to the use of telehealth services were temporarily suspended to foster increased access to care in a manner that limited personal contact and conformed to social distancing measures during the pandemic.28 The temporary suspension of regulations enables patients from any area, not just rural areas, to receive care through telehealth modalities from physicians located in any state and for these physicians to receive Medicare payments.73 This report argues that the Medicare coverage of interstate telehealth should not be limited only to the COVID-19 pandemic. Such coverage can benefit more people, may save time and money, and could provide an increased access to care for the Medicare population. At the same time, the issues of confidentiality of patient health information, patient safety, physician accountability, and licensure regulations need to be strategically incorporated and addressed in the nationwide framework of organizations participating in Medicare. The current stopgap framework for interstate telehealth that has emerged as a result of COVID-19 and the CARES Act needs to be replaced by an approach that incorporates adequate measures to minimize the likelihood of patient harm across state lines through malpractice or through the disclosure of their medical information. This two-pronged approach of continuing Medicare coverage of interstate telehealth, and concurrently addressing the issues of quality of care and patient safety is relevant in the current context and for the post-pandemic phase.
Acknowledgments
The authors thank Sarah Timmons, Emily Yin, Amira McCants, and Emily Zhai for their contributions to this endeavor. The content of this report is solely the responsibility of the authors and does not represent necessarily the views of any affiliated groups or institutions.
REFERENCES
- CIA (2020). Field listing: current health expenditure – The World Factbook – Central Intelligence Agency. Available from: https://www.cia.gov/library/publications/resources/the-world-factbook/fields/409.html [cited 14 July 2020].
- WHO (2020). World Health Statistics 2020 visual summary. Available from: https://www.who.int/data/gho/whs-2020-visual-summary [cited 14 July 2020].
- Bell M, Larson D, Weems J, Kosiak D, Mickalowski K, Kilawee L. Geographic restrictions for Medicare telehealth reimbursement. National Rural Health Association; 2011. Available from: https://www.ruralhealthweb.org/getattachment/Advocate/Policy-Documents/GeographicRestrictionsfor MedicareReimbursementPolicyPaper.pdf.aspx?lang=en-US [cited 8 July 2020].
- Nord G, Rising KL, Band RA, Carr, BG, Hollander JE. On-demand synchronous audio video telemedicine visits are cost effective. Am J Emerg Med 2019; 37(5): 890–4. doi: 10.1016/j.ajem.2018.08.017
- Adler-Milstein J, Kvedar J, Bates DW. Telehealth among US hospitals: several factors, including state reimbursement and licensure policies, influence adoption. Health Aff (Millwood) 2014; 33(2): 207–15. doi: 10.1377/hlthaff.2013.1054
- American Hospital Association (2020). Fact sheet: telehealth. Available from: https://www.aha.org/factsheet/telehealth [cited 8 July 2020].
- Dayaratna K, Larkin PJ, O’Shea J. Reforming American medical licensure. Harv J Law Public Policy 2019; 42(1): 253–78.
- Gupta A, Sao D. The constitutionality of current legal barriers to telemedicine in the United States: analysis and future directions of its relationship to national and international health care reform. Health Matrix Clevel 2011; 21(2): 385–442.
- Lum HD, Kathryn N, Camilla BP, Cari RL, William WH. Anywhere to anywhere: use of telehealth to increase health care access for older, rural veterans. Public Policy Aging Rep 2020; 30(1): 12–18. doi: 10.1093/ppar/prz030
- Centers for Medicare and Medicaid Services (2020). Fact sheet. Physician Fee Schedule Search. Baltimore, MD; CMS.gov. Available from: https://www.cms.gov/apps/physician-fee-schedule/search/search-criteria.aspx [cited 8 July 2020].
- Centers for Medicare and Medicaid Services (2020). Medicare telemedicine health care provider fact sheet. CMS.gov. Available from: https://www.cms.gov/newsroom/fact-sheets/medicare-telemedicine-health-care-provider-fact-sheet [cited 8 July 2020].
- 42 CFR § 410.78 – Telehealth Services. Legal Information Institute; 2020. Available from: https://www.law.cornell.edu/cfr/text/42/410.78 [cited 8 July 2020].
- Centers for Medicare and Medicaid Services (2020). Telehealth services. Medicare learning network booklet. Available from: https://www.cms.gov/Outreach-and-Education/Medicare-Learning-Network-MLN/MLNProducts/Downloads/TelehealthSrvcsfctsht.pdf [cited 8 July 2020].
- Nicoletti B. Facility versus non-facility in the Physician Fee Schedule. CodingIntel; 2019, Dec. Available from: https://codingintel.com/facility-non-facility-physician-fee-schedule [cited 8 July 2020].
- Centers for Medicare and Medicaid Services (2018). Information on Medicare telehealth. Available from: https://www.cms.gov/About-CMS/Agency-Information/OMH/Downloads/Information-on-Medicare-Telehealth-Report.pdf [cited 8 July 2020].
- Alaska Public Media (2018). High healthcare costs in Alaska. Alaska Insight. Available from: https://www.youtube.com/watch?v=-V7qvzY3jVk [cited 8 July 2020].
- Clif G. Health care costs in Alaska: facts, causes, consequences, and remedies. Alaska Common Ground. Available from: http://akcommonground.org/high-health-care-costs-in-alaska-facts-causes-consequences-and-remedies/ [cited 8 July 2020].
- Centers for Medicare and Medicaid Services (2020). Medicare enrollment dashboard. CMS, Office of Enterprise Data & Analytics (OEDA). Available from: https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/Dashboard/Medicare-Enrollment/Enrollment%20Dashboard.html [cited 8 July 2020].
- Kimbol AS. Whatever you do, don’t get sick at night. Health Law Perspectives; 2008. Available from: https://www.law.uh.edu/healthlaw/perspectives/2008/(AK)%20night%20shift.pdf [cited 8 July 2020].
- Apellido RM. Night shift work and weight gain among female Filipino nurses. J Obesity Overweight 2018; 4(1): 1–23. doi: 10.15744/2455-7633.4.106
- Caruso CC, Baldwin CM, Berger A, Chasens ER, Edmonson JC, Gobel BH, et al. Policy brief: nurse fatigue, sleep, and health, and ensuring patient and public safety. Nurs Outlook 2019; 67(5): 615–9. doi: 10.1016/j.outlook.2019.08.004
- Gupta A, Seshasai S. Toward the 24-hour knowledge factory. Social Science Research Network; 2004. MIT Sloan Working Paper No. 4455-04.
- Gupta A, Sando S, Parthasarathy S, Quan SF. Information technology conduit as a portal to circumvent the graveyard shift. J Clin Sleep Med 2010; 6(2): 113–6. doi: 10.5664/jcsm.27757
- Woodruff Health Sciences Center. Emory cares for ICU patients remotely, turning ‘night into day’ from Australia. Emory News Center; 2018. Available from: http://news.emory.edu/stories/2018/05/buchman-hiddleson_eicu_perth_australia [cited 8 July 2020].
- Foland M. The perfect storm: the present and developing crisis in Alaska health care access. Anchorage Daily News; 2018. Available from: https://www.adn.com/opinions/2018/11/18/the-perfect-storm-the-present-and-developing-crisis-in-alaska-health-care-access [cited 8 July 2020].
- Wohlforth C. Some Alaska medical specialists charge as much as 10 times more than doctors in Seattle. Because they can. Anchorage Daily News; 2016. Available from: https://www.adn.com/opinions/2016/09/10/some-alaska-medical-specialists-charge-as-much-as-10-times-more-than-seattle-because-they-can/ [cited 8 July 2020].
- Connolly B, Paulson L. Expanded telehealth helps communities address opioid use disorder during pandemic. Pew Charitable Trusts; 2020 Jul 1. Available from: https://www.pewtrusts.org/en/research-and-analysis/articles/2020/07/01/expanded-telehealth-helps-communities-address-opioid-use-disorder-during-pandemic [cited 8 July 2020].
- Smith AC, Thomas E, Snoswell CL, Haydon H, Mehrotra A, Clemensen J, et al. Telehealth for global emergencies: implications for coronavirus disease 2019 (COVID-19). J Telemed Telecare 2020; 26(5): 309–13. doi: 10.1177F1357633X20916567
- Mathews AW, Evans M. Hospitals use telemedicine to minimize contact with virus patients. Wall Street Journal; 2020 Mar 4. Available from: https://www.wsj.com/articles/hospitals-use-telemedicine-to-minimize-contact-with-virus-patients-11583337283 [cited 8 July 2020].
- Klevens RM, Edwards JR, Richards CL, Horan TC, Gaynes RP, Pollock DA, et al. Estimating health care-associated infections and deaths in U.S. hospitals, 2002. Public Health Rep 2007; 122(2): 160–6. doi: 10.1177F003335490712200205
- Weber DJ, Rutala WH, Miller MB, Huslage K, Sickbert-Bennett E. Role of hospital surfaces in the transmission of emerging health care-associated pathogens: norovirus, clostridium difficile, and Acinetobacter species. Am J Infect Control 2010; 38(5): S25–33. doi: 10.1016/j.ajic.2010.04.196
- Krishnan S. Telemedicine: decreasing barriers and increasing access to healthcare. Altarum Health Care Value Hub; 2017. Available from: https://www.healthcarevaluehub.org/advocate-resources/publications/telemedicine-decreasing-barriers-and-increasing-access-healthcare [cited 8 July 2020].
- GlobalMed (2015). Telemedicine in corrections: cost-effective, safer way to provide timely healthcare to prison inmates. Available from: https://globalmed.com/wp-content/uploads/internal/corrections-whitepaper.pdf [cited 8 July 2020].
- Russo JE, McCool RR, Davies L. VA telemedicine: an analysis of cost and time savings. Telemed J E Health 2016; 22(3): 209–15. doi: 10.1089/tmj.2015.0055
- INRIX (2017). Los Angeles tops INRIX global congestion ranking. Available from: https://inrix.com/press-releases/scorecard-2017 [cited 8 July 2020].
- Finkelstein JB, Cahill D, Young K, Humphrey K, Campbell J, Schumann C, et al. Telemedicine for pediatric urological postoperative care is safe, convenient and economical. J Urol 2020; 204(1): 144–8. doi: 10.1097/JU.0000000000000750
- Huilgol YS, Joshi A, Carr BG, Hollander JE. Giving urban health care access issues the attention they deserve in telemedicine reimbursement policies. Health Affairs Blog; October 12, 2017. doi: 10.1377/hblog20171022.713615
- Patterson BM, Draeger RW, Olsson EC, Spang JT, Feng-Chang L, Kamath GV. A regional assessment of Medicaid access to outpatient orthopaedic care: the influence of population density and proximity to academic medical centers on patient access. J Bone Joint Surg 2014; 96(18): 156. doi: 10.2106/JBJS.M.01188
- Harvey JB, Valenta S, Simpson K, Lyles M, McElligott J. Utilization of outpatient telehealth services in parity and nonparity states 2010–2015. Telemed J E Health 2018; 25(2): 132–36. doi: 10.1089/tmj.2017.0265
- Cullen K. Maintaining local preference while increasing vendor competition. SourceSuite. Available from: http://www.sourcesuite.com/procurement-learning/purchasing-articles/Maintaining-Local-Preference-while-Increasing-Vendor-Competition.jsp [cited 15 May 2020].
- Mitchell S, LaVecchia O. Local purchasing preferences. Institute for Local Self-Reliance. Available from: https://ilsr.org/rule/local-purchasing-preferences [cited 8 July 2020].
- State of Alaska Department of Commerce, Community, and Economic Development (2013). Alaska’s Department of Administration. Alaska Bidder Preference AS 36.30.321. Available from: http://doa.alaska.gov [cited 8 July 2020].
- Institute for Public Procurement (2015). Position paper. Local preference in public procurement. Available from: https://www.nigp.org/resource/position-papers/Local%20Preference%20in%20Public%20Procurement%20Position%20Paper.pdf [cited 8 July 2020].
- Medicare.gov. How is Medicare funded? Available from: https://www.medicare.gov/about-us/how-is-medicare-funded [cited 8 July 2020].
- Public Health Emergency (2020). COVID-19: 2019 novel coronavirus disease. 15 Jun 2020. Available from: https://www.phe.gov/emergency/events/COVID19/Pages/default.aspx [cited 8 July 2020].
- Centers for Medicare & Medicaid Services (2020). Medicare telehealth frequently asked questions (FAQs). Mar 17. Available from: https://www.cms.gov/files/document/medicare-telehealth-frequently-asked-questions-faqs-31720.pdf [cited 8 July 2020].
- American Telemedicine Association (2020). Post-COVID telehealth priorities letter to Congress. Jun 29. Available from: https://www.americantelemed.org/policy/post-covid-telehealth-priorities-letter-to-congress/?inf_contact_key=06eeeacd185586d423f37779f2b3934a [cited 8 July 2020].
- Wicklund E. House to debate extending CARES Act telehealth coverage indefinitely. mHealthIntelligence. 2020 Jun 29. Available from: https://mhealthintelligence.com/news/house-to-debate-extending-cares-act-telehealth-coverage-indefinitely?inf_contact_key=0698ade2cc4b2b203b57fd3e7b9fed54 [cited 8 July 2020].
- O’Donnell J, Alltucker K. Telehealth can be lifesaving amid COVID-19, yet as virus rages, insurance companies look to scale back. USA Today. 8 Jul 2020. Available from: https://www.usatoday.com/story/news/2020/07/03/despite-covid-19-increase-insurance-companies-pull-back-telehealth/5352297002/ [cited 8 July 2020].
- Eberly LA, Khatana S, Nathan A, Snider C, Julien H, Deleener ME, et al. Telemedicine outpatient cardiovascular care during the COVID-19 pandemic: bridging or opening the digital divide? Circulation 2020; 142: 510–2. doi: 10.1161/circulationaha.120.048185
- Velasquez D, Mehrotra A. Ensuring the growth of telehealth during COVID-19 does not exacerbate disparities in care. Health Affairs 2020. doi: 10.1377/hblog20200505.591306
- Nouri S, Khoong EC, Lyles CR, Karliner L. Addressing equity in telemedicine for chronic disease management during the Covid-19 pandemic. NEJM Catalyst 2020. doi: 10.1056/CAT.20.0123
- Chandrashekar P, Jain SH. Eliminating barriers to virtual care: implementing portable medical licensure. Am J Manag Care 2020; 26(1): 20–2. doi: 10.37765/ajmc.2020.41223
- Mataxen PA. Licensure barriers to telehealth nursing practice. Nurs 2019; 49(11): 67–8. doi: 10.1097/01.NURSE.0000580716.17521.04
- Weigel G, Ramaswamy A, Sobel L, Salganicoff A, Cubanski J, Freed M. Opportunities and barriers for telemedicine in the U.S. during the COVID-19 emergency and beyond. Kaiser Family Foundation; 2020 May 11. Available from: https://www.kff.org/womens-health-policy/issue-brief/opportunities-and-barriers-for-telemedicine-in-the-u-s-during-the-covid-19-emergency-and-beyond [cited 8 July 2020].
- Interstate Medical Licensure Compact. The IMLC. Available from: https://imlcc.org [cited 10 October 2021].
- Marino B, Prasad R, Gupta A. A case for federal regulation of telemedicine in the wake of the Affordable Care Act. Sci Tech L Rev 2015; 16(2): 274–357. doi: 10.7916/stlr.v16i2.3995
- USA.gov (2020). Foreign nationals driving in the U.S. Feb 25. Available from: https://www.usa.gov/visitors-driving [cited 8 July 2020].
- Canadian Medical Association (2019). Virtual care in Canada: discussion paper. Available from: https://www.cma.ca/sites/default/files/pdf/News/Virtual_Care_discussionpaper_v2EN.pdf [cited 8 July 2020].
- Breen KJ. National registration scheme at 5 years: not what it promised. Aust Health Rev 2016; 40(6): 674–8. doi: 10.1071/AH15187
- Breen KJ. National registration legislative proposals need more work and more time. Med J Aust 2009; 191(8): 464–5. doi: 10.5694/j.1326-5377.2009.tb02888.x
- Saleh N. Top disciplinary actions taken by medical boards. MDLinx. 2019 Jan 15. Available from: https://www.mdlinx.com/article/top-disciplinary-actions-taken-by-medical-boards/lfc-3293 [cited 8 July 2020].
- Robins D. Georgia board licenses doctors other states won’t. Atlanta Journal-Constitution; 2014 Oct 04. Available from: https://www.ajc.com/news/georgia-board-licenses-doctors-other-states-won/3o2U6KJfOh05egv1siGG4K/ [cited 8 July 2020].
- Fauber J, Wynn M, Fiore K. Prescription for secrecy. Journal Sentinel Online; 2018 Feb 18. Available from: https://projects.jsonline.com/news/2018/2/28/is-your-doctor-banned-from-practicing-in-other-states.html [cited 8 July 2020].
- Dehlendorf CE, Wolfe SM. Physicians disciplined for sex-related offenses. JAMA 1998; 279(23): 1883–8. doi: 10.1001/jama.279.23.1883
- Sao D, Gupta A, Gantz DA. Interoperable electronic healthcare record: a case for adoption of a national standard to stem the ongoing healthcare crisis. J Leg Med 2013; 34(1): 55–90. doi: 10.1080/01947648.2013.768153
- Royal K. Who owns patient medical records? J Urg Care Med. Available from: https://www.jucm.com/owns-patient-medical-records [cited 8 July 2020].
- Terry K. Patient records: the struggle for ownership. Med Econ 2015; 92(23): 22–8.
- HHS.gov (2020). Notification of enforcement discretion for telehealth remote communications during the COVID-19 Nationwide public health emergency. Mar. Available from: https://www.hhs.gov/hipaa/for-professionals/special-topics/emergency-preparedness/notification-enforcement-discretion-telehealth/index.html [cited 8 July 2020].
- Potorac K. Possible solutions to the harmonization of federal and state privacy laws for health information exchanges. Institute for e-Health Policy. 2014. Available from: https://www.e-healthpolicy.org/sites/e-healthpolicy.org/files/PossibleSolutionsHarmonization FederalStatePrivacyLaws.pdf [cited 8 July 2020].
- HHS.gov (2020). Preemption of state law. Available from: https://www.hhs.gov/hipaa/for-professionals/faq/preemption-of-state-law/index.html [cited 8 July 2020].
- Mello MM, Adler-Milstein J, Ding KL, Savage L. Legal barriers to the growth of health information exchange-boulders or pebbles? Milbank Q 2018; 96(1): 110–43. doi: 10.1111/1468-0009.12313
- Remarks by President Trump, Vice President Pence, and Members of the Coronavirus Task Force in press briefing. The White House; 2020 Mar 17. Available from: https://www.whitehouse.gov/briefings-statements/remarks-president-trump-vice-president-pence-members-coronavirus-task-force-press-briefing-4/ [cited 8 July 2020].