NARRATIVE/SYSTEMATIC REVIEWS/META-ANALYSIS
Surmounting Barriers to Healthcare Data and Information: International Case Studies
Bharath Perugu, MBA1 , Varun Wadhwa, BS2, Jin Kim, ME3, Jenny Cai, BS (Candidate)3
, Varun Wadhwa, BS2, Jin Kim, ME3, Jenny Cai, BS (Candidate)3 , Audrey Shin, BS (Candidate)4 and Amar Gupta, MBA/PhD3
, Audrey Shin, BS (Candidate)4 and Amar Gupta, MBA/PhD3
1Information Technology, ULV, Office Practicum, Fort Washington, PA, USA; 2Department of Economics, University of California, Berkeley, CA, USA; 3Department of Electrical Engineering and Computer Science, Massachusetts Institute of Technology, Cambridge, MA, USA; 4Computer Science and Economics, Wellesley College, Wellesley, MA, USA
Keywords: coordinated care, digital health, electronic health record, electronic medical record, health informatics, healthcare, interoperability, standards adoption
Abstract
Objective: This article reviews the interoperability landscape from the early 2000s to the present in Eurasia and Australia. Interoperability, in the context of this article, is “the ability to share information across time and space from multiple devices, sources, and organizations,” as defined by the IEEE (Institute of Electrical and Electronic Engineers). This review is followed by recommendations for future policy proposals that may improve the standardization of heterogeneous healthcare data in a global setting.
Methodology: A literature review was conducted on established national and supranational interoperability standards and systems in healthcare based on information obtained from journal publications, government, academy reports, published materials, and publicly available websites. Examples of specific interoperability efforts and an evaluation of their feasibility were conducted at three levels of healthcare interoperability, as defined by the National Academy of Medicine: Inter-facility (macro-tier) interoperability, Intra-facility (meso-tier) interoperability, and Point-of-care (micro-tier) interoperability.
Results: Due to the lack of available data, it is difficult to assess, in some nations, the efficacy of having one centralized system for electronic health information storage, as in the case of Taiwan. Nevertheless, this literature review still reveals that small countries in the EU, where there is a higher volume of intrastate population movement, have made considerable progress toward achieving national interoperability in healthcare records, using international and national interoperability frameworks. Uniformity in data records is more easily achieved in smaller populations when there exists a less diverse consortium of data to store and transfer, and standardization initiatives are often successful when arising from government bodies or nationally prominent health organizations.
Conclusions: As international travel becomes more commonplace and the diversity of data sources and healthcare environments grows, there is an increasing need to create more interoperable healthcare systems, not only at the national level but also at an international scale as well. A mediation strategy that can reconcile differences between different individual nationally interoperable healthcare systems will need to be developed to surmount the geopolitical boundaries that encase healthcare information.
Plain Language Summary
Enhancing healthcare globally is a challenge that requires improved standardization and communication to achieve better outcomes and value in healthcare investments. Interoperability in healthcare—the ability of two systems to exchange and use health information—is an area that, when not properly addressed, will greatly hinder data accessibility and undermine existing efforts to improve the quality of patient care.
Recognizing the importance of this issue, governments and health authorities have played a large role in promoting standards and interoperability in healthcare. There already exist many interoperable healthcare systems that have arisen on national and supranational levels in Eurasia and Australia, which store all medical records in a centralized repository and use platforms built on international standards, such as HL7 and DICOM, to standardize data formats and privacy protections. What is lacking is the ability to interoperate between individually built national systems. For example, there are no protocols set in place to safely transfer patient healthcare billing and clinical data for a patient who has moved from Europe to Asia.
To this end, the authors reviewed interoperability frameworks and systems set in motion at the international, supranational, and national levels. It explores the unique policies and systems built in each case and evaluates the efficacy and impact of each solution. This paper then spotlights the growing need for an overarching vision and mechanism that transcend geopolitical boundaries to help unify data assets scattered across heterogeneous health information systems.
Citation: Telehealth and Medicine Today © 2023, 8: 428 - https://doi.org/10.30953/tmt.v8.428
Copyright: © 2023 The Authors. This is an open access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0.
Received: May 31, 2023; Accepted: June 9, 2023; Published: July 24, 2023
Funding Statement: This research was not funded by any organization.
Financial and non-Financial Relationships and Activities: There are no financial and nonfinancial relationships or activities that might bias the interpretation of results.
Conflict Statements: No conflict of interest is involved in this paper.
Correspondening Author: Jenny Cai, Email: jxcai@mit.edu
The issue of fostering interoperability arises in many disciplines, industries, and fields, including computer hardware and software, telecommunications, finance, defense, e-governance, public safety, climate control, healthcare, and railways. In the context of computer-based systems that are used in different sectors of the economy, mechanisms for enhancing interoperability frequently evolve under the aegis of many professional organizations, such as those in Table 1.
| Professional Organization | Activity |
| The Association for Computing Machinery (ACM) | A US-based international nonprofit professional society for computing. ACM is the world’s largest scientific and educational computing society. It has established rigorous codes for upholding the ethical development and responsible use of computing tech. |
| Institute of Electrical and Electronics Engineers (IEEE) | A professional association for electronics engineering, electrical engineering, and related disciplines. |
| National Institute of Standards and Technology (NIST) | An agency of the US Department of Commerce whose mission is to promote American innovation and industrial competitiveness. NIST’s Systems Interoperability Group develops infrastructure to ensure the robustness of health IT systems.1 |
| International Organization for Standardization (ISO) | This independent organization develops standard numeric codes to ensure the quality, safety, and efficiency of products, services, and systems. In healthcare, ISO codes deal with everything from environmental and energy management to information security standards. |
| International Telecommunication Union (ITU) | ITU, part of the UN, develops codes to maintain the quality of information and communication technologies. For example, its standards ensure the high-quality reception of TV and radio programs that are free-to-air or satellite broadcasted. |
| World Health Organization (WHO) | The WHO sets standards for disease control, health care, and medicines to improve the quality of health services. |
| National Electrical Manufacturers Association (NEMA) | NEMA publishes more than a thousand medical imaging standards to ensure safety and interoperability in the use of medical imaging equipment. They are known for establishing DICOM (Digital Imaging and Communications in Medicine), which specifies a centralized way to transmit, store, and process digital medical images. |
| World Wide Web Consortium (W3C) | The W3C publishes recommendations to optimize the interoperability, security, and privacy of web standards, the tech used to build websites. |
While the need for electronic interoperability has been addressed in many cases, at the national level, mechanisms for achieving international interoperability have evolved at a slow pace, if not at all.2 This review examines specific examples of international, supranational, and national interoperability efforts concerning facilitating interoperability at three levels of healthcare interoperability, as illustrated in Figure 1.
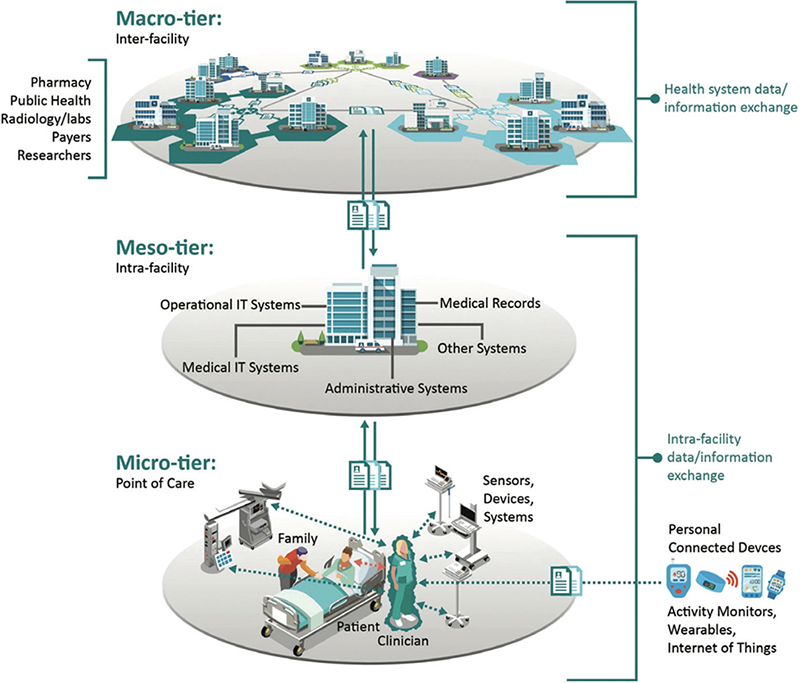
Fig. 1. Interoperability in the Health Ecosystem—Inter-facility (Macro-), Intra-facility (Meso-), and Point-of-Care (Micro-) Tiers.3
- Inter-facility (macro-tier) interoperability
- Intra-facility (meso-tier) interoperability
- Point-of-care (micro-tier) interoperability
When performing the analysis, the definition of interoperability published by the Institute of IEEE was considered: “The ability of two or more systems or components to exchange information to use the information that has been exchanged.”4 Interoperability was said to be achieved when “little or no reworking of the software to accommodate the new environment” is required and when the “behavior/benefits in the new setting…are identical to those seen in the original setting.”4
Leading Initiatives Abroad
The World Health Organization (WHO)
The WHO is a gateway to interoperability within US healthcare systems, as seen in the WHO’s utilization of ICD. Established in 1893, the International List of Causes of Death was a rudimentary directory developed by the International Statistics Institute.5 Later referred to as ICD-1, the standard was not widely adopted during its time. It would not be until 1948, with the genesis of the United Nations and, subsequently, the WHO, that the ICD would begin to see worldwide recognition for its applications. In response to the global development that occurred before and during World War 2, the WHO incorporated morbidity for the first time and released ICD version 6 in 1948.6 Much more inclined than previously, the United States joined the WHO and adopted ICD-6 for death certificate coding. Over time, however, the United States has been slow to adopt newer versions of the ICD revised by the WHO. The most recent ICD, ICD version 10, was released in 1990, with adoption not coming to the United States until 2015, 25 years after its release. Due to the excessive increase in size compared to its predecessor, ICD-10 implementation was pushed back by many US healthcare providers. Moreover, the United States emphasizes its involvement by amending the ICD to its own needs, the prime example being ICD-10-CM, a US modification of ICD-10.7 Yet, the United States continues to keep ties with ICD. Whether to avoid unnecessary changes in internal structure or for other reasons, the United States’ loyalty toward ICD implementation shows that the possibility for US ratification of interoperability standards developed by a supranational organization such as the WHO is there.
Another circumstance in which the United States adopted a globalized standard in healthcare is the implementation of the metric system. Currently, the United States is one of three countries to have not fully adopted the metric system for national use. Science and healthcare industry domains have fully adopted metric units; however, most other industries in the United States use metric units only sparingly.
After a 2015 study demonstrating that using customary measurements of teaspoons and tablespoons resulted in people using non-calibrated kitchen utensils as measuring devices, the FDA recommended that US healthcare providers use millimeter-only dosing instructions.8 This further exemplifies the United States is willingness to adopt global efforts given strong enough reasoning.
Many member states of the WHO advocate for the organization to play a role in promoting interoperability. This suggestion was implemented in December 2012 at the WHO Forum on Health Data Standardization and Interoperability, when it was recommended that the WHO host a “gateway” on eHealth standardization and interoperability to serve as a single source of information for Member States.9 Now, the organization has begun to advocate for interoperable standards to be a national effort.10 The adoption of national EHR systems among WHO member countries has witnessed a 46% global increase over 5 years. Recognizing the issue, governments and health authorities in 65 countries reported playing a role in promoting standards and interoperability. As such, countries outside of the United States have developed more efficient interoperability strategies on a national scale. Currently, four countries, Australia, the Netherlands, New Zealand, and the United Kingdom, boast nearly universal, over 90%, adoption of EHRs among care practitioners.11
The European Union (EU)
The EU’s emphasis on interoperability may be accredited to its member states’ interconnectivity. Recent statistics show that 62% of the member states’ citizens go on private trips, with 84% being to another EU member state.12 As such, the EU has recognized the necessity behind the interoperability of EHRs in its member states and has issued multiple initiatives to address the problem, such as developing the Patient Summary Guideline and creating the eHealth Action Plan. Adopted by the EU in November 2013, the Patient Summary Guideline is based on HL7 CDA and intended to support cross-border care in the EU and inform national eHealth programs. The guideline establishes the minimum essential information that needs to be exchanged to deliver safe care to a clinician’s patient, as well as recommended information that a clinician must aim to complete whenever possible. Despite the nonbinding recommendations of the PS Guideline, it symbolizes the introduction of a technical, semantic, and organizational framework for cross-border care noting the involvement that the EU Member States would accept. The PS Guideline is often compared to C-CDA, a US-based implementation guide.
The eHealth Action Plan aims to address and remove healthcare barriers for EU member states. The approaches employed by EU member states to implement national health records systems can be categorized into three models: the decentralized model, the centralized model, and the patient-centered model.13 The planned timeline extends from 2012 to 2020 and outlines the vision for eHealth in Europe. The plan even implements a special focus on mobile health to account for the widespread adoption of mobile electronics such as tablets and smartphones.14 The recent rise in importance of the subject results from recent statistics published, showing an increase in healthcare expenditure on gross domestic product (GDP) from 5.9% to 7.2% in the EU member states.15 Coincidentally, the working-age population is expected to fall dramatically from 61% to 51% of the total population.16
Within the past 5 years, the EU has initiated multiple telemedicine projects in anticipation of growing healthcare demands among its citizens. Projects such as ELECTOR, which is aimed at arthritis patients, and THALEA, which is aimed at assisting Intensive Care Units, have been funded to tackle the challenges brought upon by healthcare systems by connecting specialized care to areas that would otherwise be unable to receive such care. One branch of telemedicine is telemonitoring, the process of monitoring a patient’s health status remotely. Interoperability and guideline standardization within telemonitoring services are crucial for fully utilizing the service.17
In contrast to the national approach of WHO member states, the European Union (EU) understands the importance of supranational organizations on standardization in EHR systems. As a result, using existing standards and creating new standardized approaches have been a large focus of the EU to achieve healthcare interoperability across national borders.
The EU: Republic of Estonia
Estonia is at the forefront of healthcare IT utilization partly because Estonia is one of the most technologically savvy nations in the world, with over 88% of its population using the internet as of 2018.18 Although Estonian healthcare operates via an employer-sponsored insurance system, the country began “informal planning, and the first ideas of developing a nationwide e-health system were initiated” in the 1990s.19 Thus, Estonia planned for a national e-health system rather than a market-based option. By 2008, the e-health system of Estonia, known as the Estonian Health Information System (EHIS), was implemented.
In 2005, Estonia launched the Estonian e-Health Foundation (EeHF).19 The EeHF tries to develop standards and classifiers that will be used to create electronic records. Therefore, they can be easily shared later with other associations or countries.20 Through the EeHF, the Estonian Electronic Health Record (EHR) was developed to help physicians digitally record patient consultation information.21
Intra-facility (macro-tier) interoperability
Today, EHIS, along with each citizen’s EHR, is managed by TEHIK, a private company owned by the Estonian government.22 Furthermore, the EHIS is an integrated part of the broader Estonian e-state system, which includes e-voting, e-banking, and other government services. The Estonian parliament amended the Health Services Organization Act to mandate the submission of HL7 documents by all health providers in the country to the EHIS.23 “EHIS, by containing the health data of every Estonian resident virtually from birth to death, integrates different healthcare databases and services and makes it possible to access medical data, prescriptions, and medical images online in a secure and trusted way.”24 In 2018, Estonia became the first country to use blockchain technology to secure highly private citizen medical records.25
Inter-facility (meso-tier) interoperability
The EHIS system is composed of three layers. The first layer, the data layer, comprises repositories that store documents and images. While EHIS does not utilize a single database, it does integrate different software systems. The Estonian EHR is based on HL7 CDA, DICOM, and other internationally recognized standards for patient data exchange.19 The second layer, the data transfer layer, facilitates secure data transfer for document viewing by both patients and providers. X-Road is the data exchange layer for the Estonian e-state system. Based on the Service-Oriented Architecture (SOA) stack, X-Road is a secure passageway for data transfer that digitally signs and encrypts outgoing data and authenticates incoming data.26 The final layer, the application layer, allows for customizability by providers to offer targeted services to patients, providers, the government, and other stakeholders.19
Using the eHealth portal, providers can “send and receive laboratory test or medical imaging results electronically; can see and update an electronic medications list for their patients that includes any current medications prescribed by other physicians; can see hospital in-patient and emergency room records for their patients electronically; and can see and update an EHR for their patients including diagnosis and treatment information from multiple physicians and over time.”27
In 2010, Estonia launched its electronic prescription program, used today by the majority of physicians to prescribe medications [256]. As of January 2019, Estonia and Finland became the first EU member states to launch an ePrescriptions system that allows patients who have been prescribed medication in Finland to fill that prescription at a pharmacy in Estonia, which greatly improved pharmacy services, accuracy, flow of consultations, and accessibility of medicines.28
Point-of-care (micro-tier) interoperability
Each Estonian citizen and resident has a unique identification number, allowing an EHR to be linked to any patient in the country. Patients access EHIS through a patient portal which allows them to “view their medical data, express their health preferences and restrict access to documents.”23 Patients can also book or cancel medical consultations through the portal.23 These features are visually represented in the diagram in Figure 2.29
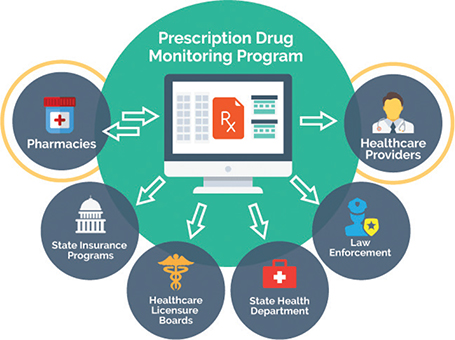
Fig. 2. PDMP Data Exchange Diagram.29
Patients access their healthcare data via the Estonian eHealth Patient Portal, which requires a patient’s signature and an Estonian National ID card for authentication. Although providers have access to patient data by default, patients using the eHealth portal can view any of their healthcare data as well as revoke or grant access to any provider.30
The Eu: The Republic Of Croatia
Since 2006, Croatia has operated the Primary Healthcare Information System (PHCIS), also known as the Croatian Health Insurance Fund’s central healthcare information networks (CEZIH), which utilizes the HL7v3 international standard and the EN 13606 European standard.31 This system hosts an EHR, patient portal, appointment scheduling, ePrescription, and eReferral services. Currently, “there is no comprehensive patient access to medical records.”
Ericsson Nikola Tesla, a Croatian-based company and an associated company of the Ericsson Group, has developed multiple platforms that facilitate interoperability, such as the Ericsson Healthcare Exchange (EHE), the Ericsson Mobile Health Exchange (EMH), the Ericsson Hospital Information System (EHIS), and eHealth Records. In Croatia, the EHE is an open communications platform that connects healthcare organizations and delivery systems. The scalability of the EHE system allows for applications to range across various healthcare service integration needs.32 Patient benefits include increased quality of life and safety as well as a reduction in unnecessary contact with the healthcare system.32
The Ericsson Mobile Health Exchange (EMH) platform helps patients and medical personnel access medical data remotely. The EMH enables healthcare providers to play a more active role in promoting patient well-being.32 The innovative structure of the EMH allows for modifications to be made for market adaptation. The EMH platform also incorporates aspects from the EHE and EHIS to integrate the systems to meet provider and patient needs.
Intra-facility (meso-tier) interoperability
For authorized users, PHCIS offers access to a patient’s lifelong medical history and personal data.33 Providers have access to data created by themselves and data explicitly sent to them.27
When a physician submits patient data to a patient’s EHR, the data are digitally signed by the physician’s smart card. The Croatian National Health Care Strategy 2012–2020 mandates that data from electronic-Personal Health Records (e-PHRs) are transmitted in real-time via Croatian Health Insurance Fund-certified software with HL7 standard messages and a virtual private network (VPN) from a provider to CEZIH.27 In Croatia, all “general, pediatric, gynecological, and dentistry practices, as well as pharmacies, primary health care laboratories, school medicine offices, out-of-hospital specialist-consulting health care, and the information system of the Croatian Health Insurance Fund, are connected to CEZIH.”32
The eHealth Records is a unified assembly where patient data are collected so that authorized doctors—those participating in the patient’s treatment and those authorized by the patient—can access it. The eHealth Records system allows doctors to survey the patient’s medical data, granting access to patient information when a patient cannot provide data or streamlining the search for clinically important information, such as allergies or medication records. Services such as ePrescription and eReferral help this platform work.
Inter-facility (macro-tier) interoperability
The EHIS helps centralize all patient data, including not only medical but also financial and administrative data. This allows medical institutions to avoid utilizing unnecessary paper records, as the data are processed automatically with EHIS. By combining large amounts of medical and nonmedical data, EHIS supports everyday clinical decision-making. Like the EHE system, the module-based, customizable nature of the EHIS allows healthcare providers to utilize this system, independent of size and specialty.32
The eHealth Records system, ePrescription, and eReferral tools are implemented in the CEZIH, which enables medical systems to store all medical information. Partially due to the implementation of these tools, the Republic of Croatia has kept a stagnant per capita spending on the health system, in comparison to the rest of the EU, which, on average, increased their per capita spending by approximately 30% from 2005 to 2015.34 The Republic of Croatia is also the lowest among the EU regarding health expenditures per capita.
One drawback to the current system is that limited terminology standards and templates exist for the Croatian system.32 Another issue is that Croatia has not implemented a national EHR system, resulting in only 3% of primary care physician offices using EHRs as of 2017.35
In 2014, Croatia released its Strategic Plan for eHealth Development. In the summer of 2019, Croatia implemented ePrescriptions for visiting Finnish citizens and access to patient summaries for Czech visitors. Croatia has also partnered with Estonia to allow Croatians abroad to fill their ePrescriptions from Croatia at Estonian pharmacies.36
Point-of-care (micro-tier) interoperability
The online patient portal component of the Croatian health information exchange system is a component of the national infrastructure and Croatian e-Citizen initiative.37 Patients access records associated with their National Health Insurance Number; however, no patient smart card is available in Croatia.37
Commonwealth of australia
Announced in July 2012, the Personally Controlled Electronic Health Record (PCEHR) is a shared health summary set up by the Australian government with the implementation overseen by the National Electronic Health Transition Authority. PCEHR is a patient-centered EHR, unlike the majority of EHRs that are provider-focused.38 The PCEHR consists of a central infrastructure for data transfer and periphery repositories for data and document storage. As a distributed system, PCEHR maps patient data across repositories by a patient’s Individual Health Identified (IHI). A PCEHR system diagram is shown in Figure 3.
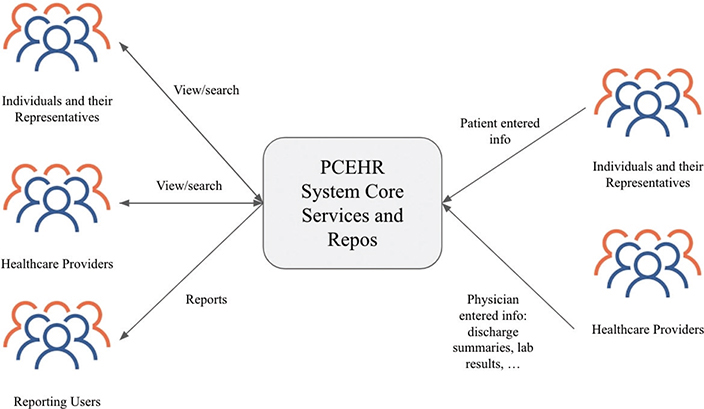
Fig. 3. Personally Controlled Electronic Health Record (PCEHR) System Diagram.
Intra-facility (meso-tier) interoperability
Most general practitioner physician offices in Australia utilize clinical information systems.39 An emergency access control exists, which enables providers to override a patient’s access settings in an emergency.40 Another unique feature of the system is that it does not allow for querying patient EHR records.38 Patient data can be viewed using the patient’s IHI in a provider portal.41 An index of available records for a queried IHI value is returned. Documents themselves are only called when selected at the index page for an IHI value in the portal.
The PCEHR is accessed using certified subsidiary software with an architecture built on two international frameworks: HL7 CDA and IHE Cross Enterprise Document Sharing (IHE XDS.b) profile.42
The Australian government offers the e-health practice incentives program (ePIP) to expand PCEHR use and training.43 While it has been budgeted to cost upwards of $800 million, the project is expected to save approximately $11.5 billion over 15 years on healthcare information exchange-related spending.39 While PCEHR offers customizability for patients, providers, like Australian Medical Association President Steve Hambleton, M.D., have expressed concerns about PCEHR complicating provider workflows, stating, “What is driving us mad is that the PCEHR has been built with so many controls that can be turned off and on by patients that they have forgotten that you want to make it easy for doctors and hospitals and other health professionals to use.”43
Inter-facility (macro-tier) interoperability
In Australia, hospital, specialist, and allied health professional adoption of such systems vary across the country.38
PCEHR uses HL7 CDA to transfer patient data from one repository to another. The Australian government uses the National Authentication Service for Health Personal Key Identifier (NASH PKI) certificate for security.44
Point-of-care (micro-tier) interoperability
Opting into the PCEHR system is optional for patients.45 Patients must register for an eHealth record with the government. Once registered, patients can control who has access to their health records. While the default eHealth record setting allows any provider with the patient’s IHI to access said patient’s record, patients can opt to delete records, restrict their access, or generate record access codes (RACs) to permit only providers with a given RAC to see a certain record.
One unique aspect of the PCEHR system is that it allows patients to generate health summaries and health notes.38 Patient data can be viewed by using the patient’s IHI in the patient portal.41
Taiwan
Each citizen and resident of Taiwan must enroll in the National Health Insurance system and receive a smart card known as the National Health Insurance Card (NHI Card).46 The NHI Card is connected to the NHIA via the NHI secure VPN. Upon visiting a provider, the NHI Card provides records of the six most recent treatments and prescriptions a patient has received. Then, the provider inserts their medical personnel ID card to load the next treatment and prescription decisions onto the NHI Card, replacing the least recent visit information of the original six most recent treatments.47 The effectiveness of the Taiwanese eHealth system is unknown, with the upload volume of medical records exceeding the download volume.48
Inter-facility (macro-tier) interoperability
The NHIA manages the information bank that holds more comprehensive patient records. Two portals to access the NHIA information bank exist: one for patients and another for providers. Launched in September 2014, My Health Bank is a patient-centered interface allowing patients to access their medical records. It aims to minimize “the information asymmetry between doctor and patient and ultimately makes medical care safer, better, and more effective.”49 My Health Bank offers both website and mobile application access.50 My Health Bank links three types of patient information via its portal: health records from the past 3 years, including dentistry and traditional medicine treatments; information about a patient’s insurance status, which can be downloaded to a patient’s physical device; and “synergistic information such as personal health records statistics, data visualization, and personalized health management information, including timely alerts for regular health examinations, health education information, and disease prognosis and risk assessment information, according to the patient’s health status.”48
Intra-facility (meso-tier) interoperability
NHI Medi-Cloud is the provider-focused portal that only grants individuals with medical personnel ID cards access to a patient’s records. The NHI Medi-Cloud includes the same types of information available to patients via My Health Bank.51 Taiwan’s Electronic Medical Record Exchange Center (EEC) is responsible for health record interoperability. Hospitals convert entered patient data to standardized formats, and the EEC indexes the XML files from all hospitals to provide querying services for providers. Hospitals commonly generate HL7 CDA documents and DICOM images for data storage, along with the IHE XDS profile for data transfer. Patients can download data from My Health Bank and use it with health applications to track and monitor their health.48
In 2013, Taiwan’s National Health Insurance Administration (NHIA) developed the “Pharmacloud System,” enabling providers to sort through patient medical records to identify adverse pharmaceutical interactions. Pharmacloud has greatly improved the efficiency and accuracy of hospital medical reconciliation processes.52
Point-of-care (micro-tier) interoperability
Patients opt-in to the NHI account system by selecting a password for their NHI account. By setting up a password, patients control physician access to their records, as the default setting for a patient’s records is without a password.53
Current Trends, Options, and Conclusion
Small countries such as Estonia have made greater progress regarding the percentage of the population whose personal health records are interoperable. One can argue that it is easier to attain greater uniformity regarding file structures and protocols in such countries. At the same time, it should be pointed out that it would be very inefficient if each country had one or more healthcare information systems that catered to a significant number of patients in that country alone, based on the growing global trend to travel across international borders. This problem is already being felt in Europe, where millions of residents travel across national borders within Europe each year, and access to medical information is impeded by differences in medical information systems and the stringent provisions for accessing personal data across national borders.
The information on symptoms, diseases, drugs, remedies, and other aspects of healthcare should be available to relevant organizations and not be constrained by organizational or national boundaries. To address an increasing need for accessing and researching data from diverse sources and environments, one needs to develop and implement effective mechanisms to surmount organizational, national, and other political boundaries concerning diverse types of healthcare information.
A potential strategy that deserves consideration is to have a better mechanism for “mediating” between the solutions being developed in different sub-niches of the healthcare areas, such as in various medical specialties, pharmacies, medical devices, health IoT space, and patient-reported outcomes (PROs). Ideally, such oversight should be provided by an entity that commands professional respect, such as an international standards organization, the World Health Organization, W3C, or a consortium involving appropriate healthcare industry representatives, governmental agencies, and academia. The consortium model was applied successfully to catalyze and globally deploy the concepts of automated nationwide processing of bank checks and Internet Telephony, respectively. In both cases, the consortium helped to surmount the reluctance to depart from conventional practices, as has been highlighted 500 years ago by renowned political philosopher Niccolo Machiavelli54:
“It ought to be remembered that there is nothing more difficult to take in hand, more perilous to conduct, or more uncertain in its success than to take the lead in introducing a new order of things. Because the innovator has for enemies all those who have done well under the old conditions and lukewarm defenders in those who may do well under the new…”
Acknowledgments
This article incorporates input from over 100 persons in industry, academia, government, and other relevant constituencies. The authors would like to acknowledge Stephanie Zawada (Ph.D. @ Mayo Clinic Graduate School of Biomedical Sciences), Kelly Zhang (MD @ Stanford University School of Medicine), and Bruce Allen Hecht (Master of Science @MIT, VG2PLAY, IEEE Standards Association) for their contributions to this paper. The authors are very grateful to their professional colleagues with whom discussions have been held on this topic. These colleagues come from many countries. The list for the United States includes Micky Tripathi, John Halamka, and (Late) Gio Wiederhold. We thank them for their interest in this important field and their inputs, comments, and suggestions over several years.
References
- NIST [Internet]. 2008 [cited 2023 Jun 24]. Systems Interoperability Group. Available from: https://www.nist.gov/itl/ssd/systems-interoperability-group
- Lesh K, Weininger S, Goldman JM, Wilson B, Himes G. Medical device interoperability-assessing the environment. In: Proceedings of the 2007 joint workshop on high confidence medical devices, software, and systems and medical device plug-and-play interoperability [Internet]. USA: IEEE Computer Society; 2007 [cited 2023 Apr 26]. p. 3–12. (HCMDSS-MDPNP ’07). Available from: https://doi.org/10.1109/HCMDSS-MDPnP.2007.22
- Pronovost PJ, National Academy of Medicine (U.S.), editors. Procuring Interoperability: achieving high-quality, connected, and person-centered care. Washington, DC: NAM.EDU; 2018. 1 p. (Learning health system series).
- Interoperability, composability, and their implications for distributed simulation: towards mathematical foundations of simulation interoperability | IEEE Conference Publication | IEEE Xplore [Internet]. [cited 2023 Jun 24]. Available from: https://ieeexplore.ieee.org/document/6690487
- 5.2 Mapping other code systems to SNOMED CT—data analytics with SNOMED CT—SNOMED confluence [Internet]. [cited 2023 May 2]. Available from: https://confluence.ihtsdotools.org/display/DOCANLYT/5.2+Mapping+Other+Code+Systems+to+SNOMED+CT
- International Classification of Diseases (ICD) [Internet]. [cited 2023 May 8]. Available from: https://www.who.int/standards/classifications/classification-of-diseases
- Chute CG, Huff SM, Ferguson JA, Walker JM, Halamka JD. there are important reasons for delaying implementation of the new ICD-10 coding system. Health Aff (Millwood). 2012 Apr;31(4):836–42. doi: 10.1377/hlthaff.2011.1258
- Jenco M. Ditch the spoon AAP: metric dosing of medications a safer choice. AAP News. 2015 Apr 1;36(4):11–11.
- First Global Forum on Human Resources for Health 2–7 March 2008 Kampala, Organization WH, Alliance GHW. Report on the first global forum on human resources for health. 2010 [cited 2023 May 8]; Available from: https://apps.who.int/iris/handle/10665/70834
- National eHealth Strategy Toolkit [Internet]. [cited 2023 May 8]. Available from: https://www.who.int/publications-detail-redirect/national-ehealth-strategy-toolkit
- The use of health information technology in seven nations| Commonwealth Fund [Internet]. [cited 2023 May 15]. Available from: https://www.commonwealthfund.org/publications/journal-article/2011/apr/use-health-information-technology-seven-nations
- People on the move [Internet]. [cited 2023 May 8]. People on the move—Chapter 4: out and about. Available from: https://ec.europa.eu/eurostat/cache/digpub/eumove/bloc-4.html?lang=en
- Dumortier J, Verhenneman G. Legal regulation of electronic health records: a Comparative analysis of Europe and the US. In: George C, Whitehouse D, Duquenoy P, editors. eHealth: legal, ethical and governance challenges [Internet]. Berlin, Heidelberg: Springer; 2013 [cited 2023 May 8]. p. 25–56. Available from: https://doi.org/10.1007/978-3-642-22474-4_2
- Capture Calendar | European Union, archived by Publications Office of the European Union | Archive-It Wayback Machine [Internet]. [cited 2023 May 8]. Available from: https://wayback.archive-it.org/12090/*/https://ec.europa.eu/digital-single-market/en/news/ehealth-action-plan-2012-2020-innovative-healthcare-21st-century
- The 2012 ageing report: economic and budgetary projections for the 27 EU Member States (2010–2060)—European Commission [Internet]. [cited 2023 May 8]. Available from: https://ec.europa.eu/economy_finance/publications/european_economy/2012/2012-ageing-report_en.htm
- Internet of things, smart sensors, and pervasive systems: enabling connected and pervasive healthcare—ScienceDirect [Internet]. [cited 2023 May 8]. Available from: https://www.sciencedirect.com/science/article/abs/pii/B9780128153680000014
- Simalatsar A, De Micheli G. Medical guidelines reconciling medical software and electronic devices: Imatinib case-study. In: 2012 IEEE 12th International Conference on Bioinformatics & Bioengineering (BIBE); 2012. p. 19–24.
- World Bank Open Data [Internet]. [cited 2023 May 8]. Individuals using the internet. Available from: https://data.worldbank.org
- Metsallik J, Ross P, Draheim D, Piho G. Ten years of the e-Health System in Estonia. Semantic Scholar. 2018;2336. Available from: https://ceur-ws.org/Vol-2336/MMHS2018_invited.pdf [Cited 31 May 2023].
- Estonian eHealth Foundation (EeHF) | Antilope ProjectAntilope Project [Internet]. [cited 2023 May 8]. Available from: https://www.antilope-project.eu/antilope-project-partners/estonian-ehealth-foundation/
- The emergence of National Electronic Health record architectures in the United States and Australia: models, costs, and questions—PMC [Internet]. [cited 2023 May 8]. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1550638/
- TEHIK [Internet]. [cited 2023 May 8]. Avaleht. Available from: https://www.tehik.ee/avaleht
- de Lusignan S, Ross P, Shifrin M, Hercigonja-Szekeres M, Séroussi B. Comparison of approaches to providing patients access to summary care records across old and new Europe: an exploration of facilitators and barriers to implementation. Stud Health Technol Inform. 2013 Aug 7;192:397–401.
- Health Services Organisation Act. Estonian Parliament. 2007 Dec. Available from: https://www.ilo.org/dyn/natlex/docs/ELECTRONIC/60517/61928/F-2104585905/EST-60517.pdf
- Heston T. A case study in blockchain healthcare innovation [Internet]. Rochester, NY; 2017 [cited 2023 May 8]. Available from: https://papers.ssrn.com/abstract=3077455
- Atkinson C, Bostan P, Draheim D. Foundational MDA patterns for service-oriented computing. J Object Technol. 2015;14(1):1:1.
- Oderkirk J. Readiness of electronic health record systems to contribute to national health information and research [Internet]. Paris: OECD; 2017 Dec [cited 2023 May 8]. Available from: https://www.oecd-ilibrary.org/social-issues-migration-health/readiness-of-electronic-health-record-systems-to-contribute-to-national-health-information-and-research_9e296bf3-en
- Zeegers Paget D, Azzopardi Muscat N, Zeegers Paget D, Jakab Z, Andriukaitis V, Charpak Y. European Public Health News. Eur J Public Health. 2019 Apr 1;29(2):381–4. doi: 10.1093/eurpub/ckz032
- Prescription Drug Monitoring Program (PDMP) | Clay County PHC, MO [Internet]. [cited 2023 May 1]. Available from: https://www.clayhealth.com/251/Prescription-Drug-Monitoring-Program-PDM
- Priisalu J, Ottis R. Personal control of privacy and data: Estonian experience. Health Technol. 2017;7(4):441–51. doi: 10.1007/s12553-017-0195-1
- The Health Systems and Policy Monitor [Internet]. [cited 2023 May 8]. Health systems in Transition (HiT) Profile of Croatia. Available from: https://www.pf.uni-lj.si/media/raziskava.delovanja.zdravstvenih.sistemov.pdf
- Ericsson Nikola Tesla d.d.—Electronic Healthcare Exchange—EHE [Internet]. [cited 2023 May 8]. Available from: https://www.ericsson.hr/en/electronic-healthcare-exchange
- Gvozdanović D, Koncar M, Kojundzic V, Jezidzić H. National healthcare information system in Croatian primary care: the foundation for improvement of quality and efficiency in patient care. Inform Prim Care. 2007 Feb 1;15:181–5. doi: 10.14236/jhi.v15i3.657
- State of Health in the EU: Croatia Country Health Profile 2021. OECD/European Observatory on Health Systems and Policies (2021), Croatia: Country Health Profile 2021, State of Health in the EU, OECD Publishing, Paris/European Observatory on Health Systems and Policies, Brussels.
- Budin A, Tesla EN. e-health: Challenges and lessons learned—AEMH 2017. Availble from: https://www.aemh.org/images/AEMH_documents/2017/AndreaBudin.pdf
- Croatia to start the exchange of ePrescriptions and patient summaries [Internet]. [cited 2023 May 8]. Available from: https://www.digitalhealthnews.eu/development/5814-croatia-to-start-the-exchange-of-eprescriptions-and-patient-summaries
- Mountford N, Kessie T, Quinlan M, Maher R, Smolders R, Van Royen P, et al. Connected health in Europe: where are we today? [Internet]. University College Dublin; 2016 the Authors [cited 2023 May 8]. Available from: http://hdl.handle.net/10197/8523
- Pearce C, Bainbridge M. A personally controlled electronic health record for Australia. J Am Med Inform Assoc. 2014 Jul 1;21(4):707–13. doi: 10.1136/amiajnl-2013-002068
- E-health in Australia and elsewhere: a comparison and lessons for the near future—PubMed [Internet]. [cited 2023 May 8]. Available from: https://pubmed.ncbi.nlm.nih.gov/23823284/
- Hanna L, Gill SD, Newstead L, Hawkins M, Osborne RH. Patient perspectives on a personally controlled electronic health record used in regional Australia. Health Inf Manag J Health Inf Manag Assoc Aust. 2017 Jan;46(1):42–8. doi: 10.1177/1833358316661063
- [PDF] Sound Foundations: leveraging International Standards for Australia’s National Ehealth System | Semantic Scholar [Internet]. [cited 2023 May 8]. Available from: https://www.semanticscholar.org/paper/Sound-Foundations%3A-Leveraging-International-for-Williams-McCauley/735350b86741d037827f3e98bd09f082ac8a125e?p2df
- NASH PKI certificates for software vendors and developers—National Authentication Service for Health—Services Australia [Internet]. [cited 2023 May 8]. Available from: https://www.servicesaustralia.gov.au/nash-pki-certificates-for-software-vendors-and-developers?context=23091
- PulseIT [Internet]. [cited 2023 May 8]. Mechanics of PCEHR are driving us mad. Available from: https://privacy.org.au/Papers/PCEHR-131122.pdf
- Practice Incentives Program—Services Australia [Internet]. [cited 2023 May 8]. Available from: https://www.servicesaustralia.gov.au/practice-incentives-program
- Andrews L, Gajanayake R, Sahama T. The Australian general public’s perceptions of having a personally controlled electronic health record (PCEHR). Int J Med Inf. 2014 Dec;83(12):889–900. doi: 10.1016/j.ijmedinf.2014.08.002
- Wu TY, Majeed A, Kuo KN. An overview of the healthcare system in Taiwan. Lond J Prim Care. 2010 Dec;3(2):115–9. doi: 10.1080/17571472.2010.11493315
- Design and prototype of a mechanism for active on-line emerging/notifiable infectious diseases control, tracking and surveillance, based on a national healthcare card system—PubMed [Internet]. [cited 2023 May 8]. Available from: https://pubmed.ncbi.nlm.nih.gov/17379353/
- An Assessment of the Interoperability of Electronic Health Record Exchanges Among Hospitals and Clinics in Taiwan—PMC [Internet]. [cited 2023 May 8]. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6458540/
- National Health Insurance Administration Ministry of Health and Welfare [Internet]. [cited 2023 May 8]. Available from: https://eng.nhi.gov.tw/en/mp-2.html
- New NHI Mobile App Brings NHI Services at Your Fingertips-National Health Insurance Administration Ministry of Health and Welfare-NEWS [Internet]. [cited 2023 May 8]. Available from: https://eng.nhi.gov.tw/en/cp-244-94ba4-8-2.html
- Creating online personal medical accounts: recent experience in two developed countries—ScienceDirect [Internet]. [cited 2023 May 8]. Available from: https://www.sciencedirect.com/science/article/abs/pii/S2211883718301783?via%3Dihub
- Tseng YT, Chang EH, Kuo LN, Shen WC, Bai KJ, Wang CC, et al. Preliminary physician and pharmacist survey of the National Health Insurance PharmaCloud system in Taiwan. Comput Methods Programs Biomed. 2017 Oct 1;149:69–77. doi: 10.1016/j.cmpb.2017.07.004
- Rau HH, Wu YS, Chu CM, Wang FC, Hsu MH, Chang CW, et al. Importance-performance analysis of personal health records in Taiwan: a web-based survey. J Med Internet Res. 2017 Apr 27;19(4):e131. doi: 10.2196/jmir.7065
- Machiavelli N. The Prince [Internet]. 1998 [cited 2023 May 8]. Available from: https://www.gutenberg.org/files/1232/1232-h/1232-h.htm