USE CASE
Telehealth in a Pediatric Patient with Nevoid Basal Cell Carcinoma Syndrome
Allison M. Jay, MD1 ; Anthony Hamame, MD2; and M. Susan Jay, MD3
; Anthony Hamame, MD2; and M. Susan Jay, MD3
1Henry Ford St. John Hospital Cancer Center Genetic Testing and Counseling, Department: Cancer Genetics Wayne State University, Detroit, Michigan, USA; 2Henry Ford St. John Hospital, Imaging Department: East Pointe Radiology, Detroit, Michigan, USA; 3Department, Adolescent Medicine, Medical College of Wisconsin, Milwaukee, Wisconsin, USA
Keywords: COVID-19, NBCCS, nevoid basal cell carcinoma syndrome, pediatrics, telemedicine
Abstract
During COVID-19, telemedicine was adopted by many practices to serve patients with a variety of health conditions, including those afflicted with cancer. Here, we report an 11-year-old patient who went to her dentist, where a routine panoramic X-ray revealed multiple jaw keratocytes. She was referred to genetics because jaw keratocysts have a hereditary predisposition to basal cell cancer and other tumors.
She received genetic counseling in 2021, where telehealth was the primary modality for visits. The hospital’s secure video platform was used to gather medical history and counsel the mother on genetic testing for nevoid basal cell carcinoma syndrome (NBCCS). Prior to 2013, the cost for genetic testing was often thousands of dollars. In this case, the genetic testing company offered a patient pay option of $250.
Two days later, the patient presented to the cancer center, where a phlebotomist collected a blood sample. A 15-minute physical examination revealed macrocephaly and palmar pitting. Of note, the mother asked about numerous pinpoint lesions around the patient’s ocular region.
Genetic testing was positive for a pathogenic variant in PTCH1 c.454_455del. The patient was referred to pediatric dermatology, where more than 50 basal cells were diagnosed. Treatment was initiated with imiquimod and fluorouracil. In addition, she was referred to cardiology and gynecology, given reports of individuals with cardiac fibromas and gynecologic ovarian tumors. The patient is now 14 years old, doing well, and starting her freshman year in high school. This case highlights how telehealth contributes to a holistic approach to patient care.
Plain Language Summary
We describe a patient with a rare pediatric genetic condition of jaw keratocysts and skin cancer at a young age. Telehealth was used to help explain her condition to her and her family. It is important for providers to engage patients through video visits and telephone visits, so that they have a successful telehealth experience and get the best care. Genetic counseling lends itself to telehealth because much of the visit is counseling and there are DNA saliva kits that can be mailed to the patient.
Citation: Telehealth and Medicine Today © 2024, 9: 520.
DOI: https://doi.org/10.30953/thmt.v9.520
Copyright: © 2024 The Authors. This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, and the use is non-commercial. See http://creativecommons.org/licenses/by-nc/4.0.
Received: August 27, 2024; Accepted: October 16, 2024; Published: October 31, 2024
Conflicts of Interests: No relevant disclosures.
Funding Statement: None.
Corresponding Author: Allison M. Jay; Email: allyjcyprus@hotmail.com
Genetics is increasingly being utilized for precision medicine in cancer and areas such as neurology and cardiology. Healthcare providers may identify an abnormality on an electrocardiogram such as prolonged QT interval, which can be associated with sudden cardiac death. Often, as part of the diagnostic workup, geneticists recommend their patients be tested for a genetic predisposition.
After the onset of the COVID-19 pandemic in 2020, telehealth was increasingly offered for healthcare visits, which provided the entire family the opportunity to be present for the visit.1 Advantages of telehealth appointments include improved access for patients living in rural areas or far from a hospital center, with limited transportation options, and/or limited time availability due to work or school schedules. For patients unfamiliar with genetics and how it might impact their care, telehealth offers a comfortable medium for both patient and family to receive background information on genetics, how this testing is utilized in their care, and how it might impact other family members.
In addition to healthcare visits, teledentistry was popular after the COVID-19 epidemic in that it limited person-to-person contact. Teledentistry was first studied by the United States Army in 1994 as part of its Total Dental Access project, and in 1997 the term “teledentistry” was coined2 to describe the use of video telehealth to diagnose patients with dental conditions.3,4 Uhrin and colleagues4 conducted a meta-analysis of teledentistry looking at how oral cancers could be detected remotely. They found that teledentistry could contribute to earlier diagnosis and treatment of oral potentially malignant disorders (OPMD). While teledentistry was not utilized in the case reported here, it has the potential to improve care for many patients living far from a dental specialist. Teledentistry (as with telehealth) might have many few completed studies support the value of teledentistry in a diverse group of patients5, and future studies to address this in patients are needed.
Regarding the cost and Advances in Genetic Technology, prior to 2011 the cost of genetic testing for single gene disorders was often greater than $1,000 using sanger sequencing—the “gold standard” of genetic testing. For example, for two genes associated with hereditary breast and ovarian cancer, BRCA1 and BRCA2, Myriad Genetics, Inc. sequencing these genes in a patient cost approximately $3,000. On June 13, 2013, the Supreme Court ruled that patenting genes was unconstitutional and soon after genetic panels with genes including BRCA1, BRCA2 and other genes were increasingly offered using new next generation sequencing (NGS) technology. The NGS reduced cost and allowed many genetic testing companies to offer patient pay options of $250 with patient assistance plans, making it more feasible for many patients and their families.
With more reasonable genetic testing costs, and telehealth lending itself to genetic counseling, after the pandemic more patients were interested in this option for their care. The advantage with an initial telehealth consultation for genetics is that the patient and family can share information about their personal and family history in the comfort of their home and ask questions about the meaning of their results. Given that the physical examination might help to identify the condition the child has, and what genetic test should be used to confirm the condition, our genetics practice offers pediatric patients a brief 15- to 20-minute in-person visit after the initial telehealth visit where a physical examination is completed and blood is drawn.
In this case report, we describe a patient referred because of pathognomonic findings of jaw keratocysts on dental X-ray. This dental finding is known to be a sign of basal cell nevoid syndrome. Basal cell nevoid syndrome (OMIM #109400) is an autosomal dominant condition with a prevalence ranging from 1/31,000 to 1/164,000.6,7 This syndrome was originally known as “Gorlin Syndrome” after Robert Gorlin, a dentist in Minneapolis, Minnesota, United States.8 He subsequently collaborated with a dermatologist Dr. Bob Goltz and in 1960 they published “Multiple Nevoid Basal Cell Epitheliomata, Jaw Cysts, Bifid Rib-a Syndrome” in The New England Journal of Medicine.9 For a period the syndrome was often referred to as Gorlin/Goltz syndrome. However, more recently it is commonly referred to as basal cell nevoid syndrome.
Case Report
An 11-year-old female was referred by her dentist to our center’s oral maxillofacial surgeon to remove a jaw keratocyst, shown as a 2.5 × 2.5 cm radiolucent lesion of the right mandibular body (Figure 1: Dental Panorama X-ray). The patient was in sixth grade and enjoyed science and art.
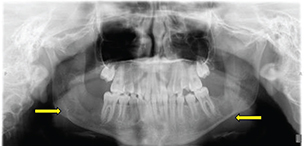
Fig. 1. Panoramic dental radiograph showing multiple bilateral odontogenic keratocysts.
As part of the workup for the dental findings, she had a computed tomography (CT) of the head, which identified a calcified falx cerebri (Figure 2). A CT of the jaw (Figure 3) revealed multiple mini cysts and a large cyst in her lower jaw. Surgery removed a cyst from the right mandibular body and ramus associated with impacted tooth #31 pathology was consistent with an odontogenic keratocyst. After being seen by the surgeon, she was referred for genetic testing. Her past medical history was notable for a broken arm, benign hydrocephalus at around 8 months of age for which she had magnetic resonance imaging performed.
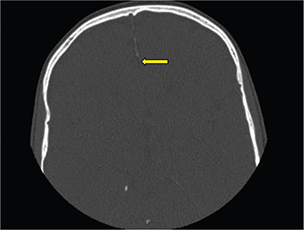
Fig. 2. Axial head CT of 11-year-old female showing calcifications of the falx cerebri not typically present at this age. CT: computed tomography.
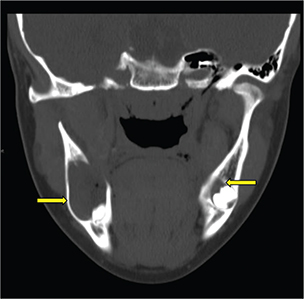
Fig. 3. Coronal maxillofacial CT demonstrating expansile cystic lesions in the bilateral mandible compatible with multiple odontogenic keratocysts. CT: computed tomography.
During the telehealth visit a three-generation family history was obtained (Figure 4). No individuals with jaw keratocysts or basal cell cancers were reported. The mother reported possible lupus/mixed connective tissue disorder. Her brother had attention-deficit/hyperactivity disorder. Another brother had a connective tissue disorder. At the time of initial consultation, the father of the patient had a cyst on his arm but no known basal cells.
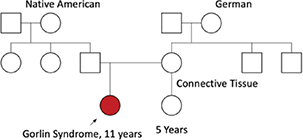
Fig. 4. A 3-generation pedigree for patient.  Gorlin Syndrome.
Gorlin Syndrome.
The patient was counseled about nevoid basal cell carcinoma syndrome (NBCCS), which can present with systems outside the skin including in the genitourinary system: ovarian fibromas, ovarian cysts, and cardiac fibromas. Given clinical suspicion for NBCCS, she was referred to gynecology, which did not identify any ovarian abnormalities, and cardiology. Cardiology coordinated an echocardiogram, which demonstrated multiple small hyperechoic lesions suggestive of fibromas in the left ventricular free wall, papillary muscles, apex, and interventricular septum.
The patient continues to be monitored closely by cardiology. Genetic testing was positive for a pathogenic variant in PTCH1. Recently, the father of the patient contacted us to have genetic testing for the PTCH1 variant, given he was newly diagnosed with three basal cell cancers at 33 years old. Because he works in a 6 am to 6 pm shift 1 week on and 1 week off and lives approximately 1 hour and 45 minutes away, a telehealth visit allowed access to care after his work hours and allowed physical examination of the skin lesions biopsied. His genetic work up is still in progress.
Discussion
Nevoid Basal Cell Carcinoma Syndrome
Major criteria for NBCCS include: basal cell cancers before age 20 years, odontogenic keratocysts of the jaw before age 20 years, palmar/plantar pitting, lamellar calcification of the falx cerebri, medulloblastoma, and having a first degree family member who has been diagnosed (such as a mother or father).10 The genes for Nevoid Basal Cell Carcinoma Syndrome encode proteins which have tumor suppressor activity in the Hedgehog (Hh) signaling pathway. Consequently mutations in these genes disrupt their ability to suppress tumors, and contribute to basal cell proliferation.2 The PTCH gene makes up 67% to 79% of pathogenic variants. SUFU, Suppressor of Fused Homologue, accounts for approximately 6% of patients diagnosed, and unknown etiology occurs in 15% to 27% of patients.10 The PTCH2 gene has been more recently included on gorlin syndrome panels, the percentage of cases attributed to this gene is unknown. Of note, patients with SUFU are at greater risk for medulloblastoma often before age five, and screening recommendations exist for these young pediatric patients.
In terms of implications for family members, 70% to 80% of patients have an affected parent. Telehealth is a feasible option to offer cascade testing to family members, in that they could have a virtual appointment and be sent a genetics saliva kit to coordinate targeted testing for the pathogenic variant found in their family members. Many companies offer free cascade testing for family members for three months from a positive report date.
Telehealth Implications
While Danylchuk and colleagues5 found limited studies of telehealth in diverse populations, Dr. Samantha Tam at Henry Ford Health System in Detroit, Michigan, USA studied both telephone visits and video visits in a diverse group of patients affected with head and neck cancers. The results revealed that while patients with “lower median household incomes had less odds of completing a virtual visit. This disparity was not demonstrated in telephone visits.”11 As a result of this success with telephone visits in adult cancer patients, it is plausible that such success would be replicable in parents of pediatric patients being evaluated for genetic syndromes.
Green and colleagues12 published “An Evidence Based Guideline of the National Society of Genetic Counselors for Telehealth” in 2022. They conducted a systematic evidence review, which found telehealth genetic counseling had noninferior outcomes compared to in-person visits. The key takeaway from their guideline is that many of the studies were in cancer. With cancer genetics the session, often, a discussion of cancer and genes and physical examination is not performed because it does not actionably impact the decision of which genes to test. In pediatrics conditions, the physical examination can be helpful in refining the differential diagnosis of the patient’s condition and is important in choosing the genes to sequence. Another important finding from their guideline, is that telehealth could “increase health disparities for certain populations and could worsen the divide in digital equity.”
Per the National Digital Inclusion Alliance, digital equity is defined as a “condition in which all individuals and communities have the information technology capacity needed for full participation in our society, democracy, and economy.13 Digital equity is necessary for civic and cultural participation, employment, lifelong learning, and access to essential services.” Patients with unreliable internet access, telephone access, no healthcare insurance for telephone/telehealth visits may experience challenges with this medium. In addition, for genetics patients, some studies have shown less success in at home collection using saliva kits (due to patients eating before collection) and buccal kits as compared to blood draws.12 In addition, potential errors include patients mislabeling their saliva specimen.14 This may contribute to longer turnaround times for results. While many cancer genetic testing companies offer mobile phlebotomy for adult patients, in general, this is not offered for pediatric patients.
Green and colleagues12 also discussed barriers for providers to offer genetics care through telehealth. These include difficulty in offering psychosocial support to patients over the phone, and inability to use genetic counseling visual aids to explain background information on genetics. Our clinic has found success asking our community hospital social worker to follow up with a phone call to inquire about ways to offer support for cancer patients for concerns such as a lack of housing or transportation. For in person visits, genetic counselors and the geneticist have visual aids as part of a slide show that covers background information on genetics, cancer, and inheritance for families. For phone counseling, we use the same visual aids to structure the phone interview. We describe what is on our screen and aim to “slow down the visit” to explain genetic concepts to the patient in a way they can understand. Our genetics team often tries to use an analogy to describe genetics and mutations in line with their job occupation, essentially meeting them where they are. Other pragmatic barriers include the inability to perform a physical examination and financial considerations such as lack of insurance payor coverage for visits.
Conclusion
This case report highlights that telehealth can be successful in genetic counseling and genetic visits in the future may combine telehealth and brief in-person visits to coordinate blood draws and targeted physical examinations for pediatric patients. Guidelines published by Drs. Tam’s11 and Green’s12 emphasize the need for providers to continue to be committed to engaging patients in multiple modalities, promoting digital equity, and adapting care delivery to the needs of the patient.
Contributors
Dr. Allison Jay drafted the case report, Dr. Hamame drafted writeup on the radiology section, Dr. Susan Jay contributed to revision and editing of the case report.
Informed Consent Statement
The patient’s mother signed consent for this case report available upon request.
Data Availability Statement (DAS), Data Sharing, Reproducibility, and Data Repositories
None were used.
Application of AI-Generated Text or Related Technology
Contact the corresponding author for more information.
Acknowledgments
The authors would like to thank Justin Beatty for his diligent review of the references, and Dr.Susan Szpunar for her conscientious review of the manuscript and thoughtful insights. The authors are also grateful to Louise Milobowski for her encouragement and kind support of this paper, and Maryann Rubio and Lorrie Lipa for offering resources that improved the quality of this paper.
References
- Breen KE, Tuman M, Bertelsen CE, Sheehan M, Wylie D, Fleischut MH, et al. Factors influencing patient preferences for telehealth cancer genetic counseling during the COVID-19 pandemic. JCO Oncol Pract. 2022;18(4):e462–71. https://doi.org/10.1200/OP.21.00301
- Gambini D, Passoni E, Nazzaro G, Beltramini G, Tomasello G, Ghidini M, et al. Basal Cell Carcinoma and Hedgehog Pathway Inhibitors: Focus on Immune Response. Front Med (Lausanne). 2022;9:893063.
- Islam MRR, Islam R, Ferdous S, Watanabe C, Yamauti M, Alam MK, et al. Teledentistry as an effective tool for the communication improvement between dentists and patients: an overview. Healthcare (Basel). 2022;10(8):1586. https://doi.org/10.3390/healthcare10081586
- Uhrin E, Domokos Z, Czumbel LM, Koi T, Hegyi P, Hermann P, et al. Teledentistry: a future solution in the diagnosis of oral lesions: diagnostic meta-analysis and systematic review. Telemed J E Health. 2023;29(11):1591–600. https://doi.org/10.1089/tmj.2022.0426
- Danylchuk NR, Cook L, Shane-Carson KP, Cacioppo CN, Hardy MW, Nusbaum R, et al. Telehealth for genetic counseling: a systematic evidence review. J Genet Couns. 2021;30(5):1361–78. https://doi.org/10.1002/jgc4.1481
- Verkouteren BJA, Cosgun B, Reinders M, Kessler P, Vermeulen RJ, Klaassens M, et al. A guideline for the clinical management of basal cell naevus syndrome (Gorlin-Goltz syndrome). Br J Dermatol. 2022;186(2):215–26. https://doi.org/10.1111/bjd.20700
- Barankin B. Nevoid basal cell carcinoma syndrome (Gorlin syndrome). UptoDate; 2024. [cited 2024 Aug 25]. Available from: https://medilib.ir/uptodate/show/5340
- Gorlin RJ. Nevoid basal cell carcinoma (Gorlin) syndrome. Genet Med. 2004;6(6):530–9. https://doi.org/10.1097/01.GIM.0000144188.15902.C4
- Gorlin RJ, Goltz RW. Multiple nevoid basal-cell epithelioma, Jaw Cysts and Bifid Rib—a syndrome. N Engl J Med. 1960;262:908–12. https://doi.org/10.1056/NEJM196005052621803
- Evans DG. Nevoid basal cell carcinoma syndrome. In: Adam MP, Feldman J, Mirzaa GM, Pagon RA, Wallace SE, Bean LJH, et al., editors. GeneReviews((R)). Seattle, WA; 1993, updated 2024.
- Tam S, Wu VF, Williams AM, Girgis M, Sheqara JZ, Siddiqui F, et al. Disparities in the uptake of telemedicine during the COVDI-19 surge in a multidisciplinary head and neck cancer population by patient demographic characteristics and socioeconomic status. JAMA Otolayrngol Head Neck Surg. 2021;47(2):209–11. https://doi.org/10.1001/jamaoto.2020.3052
- Green S, Hartzfeld D, Terry AB, Fissell K, Friedman S, Paolino N, et al. An evidence-based practice guideline of the National Society of Genetic Counselors for telehealth genetic counseling. J Genet Couns. 2023;32(1):4–17. https://doi.org/10.1002/jgc4.1627
- National Digital Inclusion Alliance [Internet]. [cited 2024 Aug 25]. Available from: https://www.digitalinclusion.org/definitions/
- Williams S, Ebrahimzadeh JE, Clay D, Constantino G, Heiman J, Wangensteen KJ, et al. Comparing telemedicine and in-person gastrointestinal cancer genetic appointment outcomes during the COVID-19 pandemic. Hered Cancer Clin Pract. 2023;21(1):6. https://doi.org/10.1186/s13053-023-00250-8
Copyright Ownership: This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, and the use is non-commercial. See http://creativecommons.org/licenses/by-nc/4.0.