ORIGINAL RESEARCH
Impact of Patients’ Health Literacy on the Adoption of Medical Teleconsultation: Evidence From France
Corinne Rochette, PhD1,2  ; Norbert Lebrument, PhD1,2
; Norbert Lebrument, PhD1,2 
1Full Professor, Management Sciences, IAE Clermont Auvergne, France; 2Full Professor, Management Sciences, leRMa Research Centre, Clermont-Ferrand, France
Keywords: E-health, France, health literacy, patient empowerment, structural equation modeling, technology acceptance model, teleconsultation adoption
Abstract
Objectives: Medical teleconsultation is a key solution to improve access to healthcare, particularly during crises. This study examines the influence of patients’ health literacy on the adoption of medical teleconsultation in France. We hypothesize that higher levels of health literacy are associated with more positive perceptions and greater intention to use teleconsultation services.
Methods: We conducted a nationwide online survey of 1,163 French adults between December 2020 and January 2021. The proposed conceptual model integrates three key dimensions of health literacy—understanding, access, and evaluation—with core constructs from the technology acceptance model (TAM), including perceived usefulness, ease of use, trust, and intention. The model was tested using partial least squares structural equation modeling (PLS-SEM).
Results: The structural equation model explains 54.2% of the variance in teleconsultation adoption. While health literacy dimensions positively influence perceived ease of use, two of them—understanding and access—showed a surprising negative impact on perceived usefulness. Trust in teleconsultation emerges as a key mediating factor between literacy and adoption. All paths in the model are statistically significant.
Conclusion: This study provides novel empirical evidence that patients’ health literacy significantly shapes their attitudes toward and intention to use teleconsultation although not always in the expected direction. These findings highlight the importance of tailoring digital health services to diverse literacy profiles and call for further research to better understand the nuanced effects of literacy in digital healthcare environments.
Plain Language Summary
Teleconsultation helps people access medical care remotely. This became especially important during the COVID-19 pandemic. To use these services effectively, patients need certain skills, like understanding health information and using digital tools. This study looked at how people’s health literacy—their ability to find, understand, and use health information—affects their use of teleconsultation in France. Based on a national survey, we found that health literacy influences people’s trust in and intention to use teleconsultation. Interestingly, having more knowledge does not always lead to more positive views. These results suggest that teleconsultation tools should be adapted to different levels of health literacy.
Citation: Telehealth and Medicine Today © 2025, 10: 548
DOI: https://doi.org/10.30953/thmt.v10.548
Copyright: © 2025 The Authors. This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0.
Submitted: December 19, 2024; Accepted: April 16, 2025; Published: May 31, 2025
Funding Statement: This work was supported by the research chair health and territories of the foundation of Clermont Auvergne University.
Financial and non-Financial Relationships and Activities: The authors declare no conflicts of interest. This study was conducted in accordance with ethical guidelines. This submission adheres to the author guidelines provided by Telehealth and Medicine Today.
Corresponding Author: Corinne Rochette, corinne.rochette@uca.fr
The concept of health literacy, introduced in the 1970s, has received increasing attention since the 1990s. Health literacy is an important part of the ability of patients to meet the complex demands of health in a modern society.1 Its growing complexity has multiple origins, including determinants of diseases and increasing medical knowledge. In addition, the chronicity of many diseases is due to an aging population, which leads to complex care and, moreover, leads people to self-manage their disease.
Added to this is the difficulty of accessing medical resources, which are becoming increasingly scarce in some regions (also known as “medical deserts”). There is therefore a challenge to develop the health literacy of the population, as well as to offer services (in particular e-health) that enable people who are sometimes geographically distant from medical resources to benefit from health services.
It is in this context that telemedicine has emerged as a set of practices enabling remote healthcare delivery using information and communication technologies. The latter includes several modalities, such as tele-expertise (professional-to-professional exchanges), telemonitoring (remote patient follow-up), and teleconsultation.
Teleconsultation is a synchronous remote consultation between a patient and a healthcare professional using video or audio transmission tools. It differs from broader concepts such as e-health—which encompasses digital tools for health information management, mobile health applications, or health portals—by focusing specifically on the act of medical consultation. In France, the COVID-19 pandemic acted as a catalyst for the deployment of teleconsultation services, which were supported by regulatory and financial incentives from public health authorities. However, despite strong governmental support, disparities persist in the use of teleconsultation across the population, particularly linked to sociodemographic and cognitive factors.
Teleconsultation is one of the solutions to meet the need of patients to access health services rapidly. Medical teleconsultation changes the relationship between patients and physicians. It requires new skills among patients. These include, firstly, technical (the ability to use a teleconsultation device) and, secondly, cognition (the ability to describe their symptoms and their state of health with precision). We therefore hypothesize that a good level of health literacy can be predictive for the adoption of teleconsultation.2
Health literacy is conceptualized as a set of capacities, which are partly knowledge based. It is context specific and subject to the influence of healthcare interactions and structures, such as the way services are organized and delivered.3 Nutbeam3 considers it an asset. In the conceptual model of health literacy risks, he distinguished three different types of literacy: functional, interactive, and critical. Based on this perspective, people with better developed health literacy will have skills and capabilities that enable them to engage in a range of health-enhancing actions, including personal behaviors (e.g., changed health behaviors and practices), as well as social actions for health and the capability of influencing others toward healthy decisions. People with better health literacy have access to a wider range of health options, such as improved outcomes, greater autonomy in decision-making, and alternative care pathways. Telemedicine, for example, can be one such option—allowing individuals to receive medical advice remotely rather than forgoing care altogether.
Different definitions of health literacy can be synthesized around four dimensions relevant to health: (1) access/obtain information, (2) understand information, (3) process/appraise information, and (4) apply/use information.4–7 Considering these dimensions, using teleconsultation means having technical ability and the ability to describe symptoms, thus demonstrating navigation skills within the health system and a level of digital health literacy. This requires developing services that allow people to interact with health professionals and experts to, among other things, easily access health and care services.
Many literacy measurement tools have been developed.8 An important limitation to their use is the mobilization of significant human resources, as most measures rely on face-to-face assessment and heavily on understanding medical terms. Classical measurement tools such as Rapid Estimate of Adult Literacy in Medicine (REALM) and Test of Functional Health Literacy in Adults (TOPHLA) have long been confined to assessing the ability to read, understand, and use written information or numeracy skills applied to health management (e.g., blood glucose interpretation). More recent scales, such as the Health Literacy Questionnaire (HLQ) or the Health Literacy Survey-Europe (HLS-EU), consider a broader understanding of the concept in order to consider a more global action.9, 10 From this perspective, it seems interesting to use part of the HLQ questionnaire to collect the perceptions that people (potential patients) have of medical information and their use of it.
Therefore, we propose to assess health literacy by putting forward a general measurement tool based on the four dimensions of health literacy: (1) accessing, (2) understanding, and (3) evaluating medical information to act (in our case), as well as (4) adopting teleconsultation.
An analysis of the literature reveals a significant lack of empirical studies investigating the impact of health literacy on the adoption of teleconsultation in the French context. To address this gap, our research empirically tests a conceptual model based on the technology acceptance model (TAM),11–14 extended to include trust in technology,15 resistance to using medical teleconsultation, and technological anxiety. The model we propose, illustrated in Figure 1, seeks to answer the following question: “Is the intention to use teleconsultation influenced by specific dimensions of patients’ health literacy?”
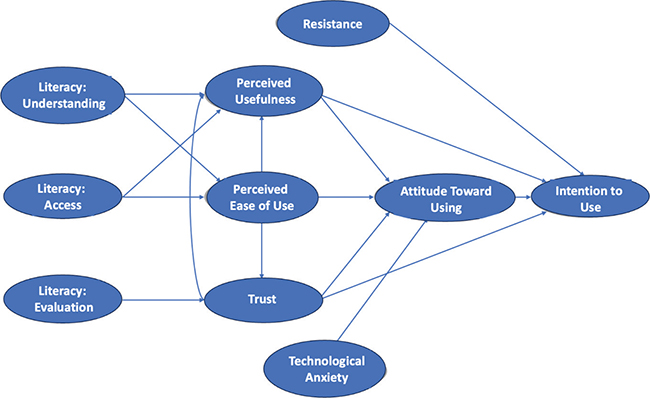
Fig. 1. Conceptual model of the impact of literacy on the adoption of medical teleconsultation.
Our model integrates three core dimensions of health literacy—understanding of medical information, access to medical information, and evaluation of healthcare services4–7—with the main constructs of TAM to explain patients’ intention to adopt medical teleconsultation. These dimensions are hypothesized to influence several intermediate variables, including perceived ease of use, perceived usefulness, trust in teleconsultation technology, attitude toward use, technological anxiety, and resistance to technology. The model includes 16 hypotheses (H1–H16), each corresponding to a direct path tested among the variables. H1–H3 link health literacy to perceived ease of use and trust; H4–H8 relate to core and extended TAM constructs, such as trust and anxiety; H9–H12 explain behavioral intention to use teleconsultation based on perceptions and attitudes; and H13–H16 reflect additional tested relationships, including unexpected negative effects of health literacy on perceived usefulness, as well as classic TAM pathways (e.g., ease of use → usefulness; ease of use → attitude).
All proposed relationships are based on prior research2 and are empirically tested using structural equation modeling, with results detailed in Appendices 1 and 2.
Methods
Study Design and Sample
Data were collected between December 2020 and January 2021 using an online platform and survey tool dedicated to research data collection. We used the quota method adjusted by removal only to have a representative sample of the French population. The questionnaire, based on voluntary participation, was self-administered to adults aged 18 years or older throughout France. There were 1,163 respondents who completed the questionnaire, which included proposals on which the respondents had to give their opinion. Table 1 summarizes the demographics of the cohort of respondents.
Measurements
To operationalize the constructs of the conceptual model, we selected the measurement instruments presented in Appendix 1. All were drawn from prior research. These instruments were adapted and contextualized to fit the specific focus of our study. Health literacy was assessed using three self-reported blocks of questions: (1) three items measuring the understanding of medical information, (2) four items assessing access to medical information, and (3) four items related to the evaluation of healthcare services. Responses were recorded using a five-point Likert scale. To measure these dimensions, we selected the HLQ developed by Osborne et al. (2013) as it provides a validated, multidimensional approach to health literacy. Unlike earlier tools such as REALM or TOFHLA, which focus primarily on reading skills or numeracy, the HLQ captures functional, interactive, and critical aspects of literacy. These dimensions are essential to understanding how individuals access, interpret, and apply health-related information in decision-making contexts—particularly in digital environments such as teleconsultation. For this study, we used a subset of HLQ items corresponding to the three key dimensions mentioned above. These items were translated and culturally adapted to the French context through a standardized, multistep process:
- Initial translation and back-translation by bilingual health and social science experts.
- Pre-testing with a pilot sample of 25 adult respondents to assess clarity and cultural appropriateness.
- Minor wording revisions to enhance comprehension while preserving the conceptual integrity of each dimension.
This approach ensured that the adapted instrument was linguistically accurate, contextually relevant, and accessible to a diverse French adult population. We followed the main recommendations in the literature16–18 to define the measurement instruments and validate the content of each construct. In addition, we assessed the reflective nature of the model’s constructs using the decision criteria proposed by Jarvis et al.19
Statistical Analysis
The test of the structural equations model according to the PLS-PM approach was conducted using XLSTAT 2021.2.1.1124 for Windows. For all analyses, a p value (two-tailed) of <0.05 was considered to indicate statistical significance. Table 2 shows the estimation parameters used.20 Partial least squares path modeling (PLS-PM) was applied as a statistical technique used to estimate complex cause‑effect relationships between observed and unobserved variables. Latent variables, such as trust or perceived usefulness, are unobservable theoretical constructs inferred from multiple measured indicators. PLS-PM is particularly suited for models with multiple latent constructs and when the data do not meet multivariate normality assumptions.
After verifying the factorability of the data, we validated the external and internal models based on three levels of assessment:
- The quality of the measurement model and the scales used, including internal reliability (Cronbach’s alpha and Dijkstra–Henseler’s rho), convergent validity (unidimensionality), and discriminant validity.
- The quality of the structural model was assessed through the coefficient of determination (R²) for each dependent latent variable and the significance levels of the path coefficients, evaluated using a bootstrapping procedure (5,000 resamples).
- The global fit of the model using the goodness of fit (GoF) index. The GoF reflects the overall fit by combining the quality of both the measurement model and the structural model paths.
Cronbach’s alpha and Dijkstra–Henseler’s rho (ρA) are indicators of internal consistency, measuring how reliably the items represent each construct. Average variance extracted (AVE) indicates how much of the variance in the observed variables is explained by the latent construct. Values above 0.70 for alpha and rho and above 0.50 for AVE are considered acceptable. Path coefficients indicate the strength and direction of the relationships between variables. The R² values show the proportion of variance explained in each dependent variable. Cohen’s f² reflects the effect size of individual predictors. All significance levels were estimated using bootstrapping (5,000 resamples), providing robust t-values and confidence intervals.
Results
Descriptive statistics for all samples are presented in Appendix 1. These results enable the reliability of the measuring scales used in our research to be validated (Table 2).
| Latent variable | Cronbach’s alpha | DG rho (ρ)* | Average variance extracted |
| Literacy: Understanding | 0.838 | 0.903 | 0.754 |
| Literacy: Access to medical information | 0.836 | 0.891 | 0.672 |
| Literacy: Health care evaluation | 0.778 | 0.857 | 0.598 |
| Technological anxiety | 0.904 | 0.954 | 0.909 |
| Resistance | 0.906 | 0.941 | 0.841 |
| Perceived ease of use | 0.921 | 0.944 | 0.808 |
| Trust in technology | 0.947 | 0.966 | 0.904 |
| Perceived usefulness | 0.945 | 0.958 | 0.821 |
| Attitude toward using | 0.955 | 0.967 | 0.880 |
| Intention to use | 0.940 | 0.962 | 0.893 |
| *DG rho (ρ): Dillon-Goldstein’s rho. | |||
Regarding the test results of the structural model analyzed in Table 4, the percentage of variance explained for each of the dependent variables of the model is satisfactory (13.8% for perceived ease of use of medical teleconsultation, 38.6% for trust in medical teleconsultation, 78.6% for attitude toward using medical teleconsultation, and 75.5% for intention to use medical teleconsultation). The average of the variance explained by our model is 54.2%. All the relationships tested with a bootstrap method are significant. These results underscore the predictive validity of the proposed model to explain the impact of literacy on the adoption of medical teleconsultation.
| Variable | R2 | Path coefficient | Significance (t) | Pr >|t| | f2 of Cohen | Conclusion about the influence |
| Influence on perceived usefulness of medical teleconsultation: | 0.645 | |||||
| Literacy: understanding | –0.072 | –3.27** | 0.001 | 0.009 | Negative | |
| Literacy: access | –0.048 | –2.24* | 0.026 | 0.004 | Negative | |
| Perceived ease using medical teleconsultation | 0.188 | 8.07*** | 0.000 | 0.056 | Positive | |
| Trust in medical teleconsultation | 0.699 | 31.28*** | 0.000 | 0.845 | Positive | |
| Influence on perceived ease of use of medical teleconsultation: | 0.138 | |||||
| On literacy: understanding | 0.244 | 7.33*** | 0.000 | 0.046 | Positive | |
| On literacy: access | 0.174 | 5.24*** | 0.000 | 0.024 | Positive | |
| Influence on trust in medical teleconsultation: | 0.386 | |||||
| On perceived ease of use of medical teleconsultation | 0.597 | 25.07*** | 0.000 | 0.542 | Positive | |
| On literacy: evaluation | 0.079 | 3.32*** | 0.000 | 0.009 | Positive | |
| Influence on attitude toward using medical teleconsultation: | 0.786 | |||||
| On perceived usefulness of medical teleconsultation | 0.322 | 14.26*** | 0.000 | 0.176 | Positive | |
| On perceived ease of use of medical teleconsultation | 0.174 | 9.22*** | 0.000 | 0.073 | Positive | |
| On trust in medical teleconsultation | 0.464 | 19.83*** | 0.000 | 0.340 | Positive | |
| Technological anxiety | –0.059 | –3.87*** | 0.000 | 0.013 | Negative | |
| Influence on intention to use medical teleconsultation: | 0.755 | |||||
| On resistance | –0.077 | –5.28*** | 0.000 | 0.024 | Negative | |
| On perceived usefulness of medical teleconsultation | 0.284 | 10.90*** | 0.000 | 0.103 | Positive | |
| On trust in medical teleconsultation | 0.293 | 10.14*** | 0.000 | 0.089 | Positive | |
| On attitude toward using medical teleconsultation | 0.341 | 11.49*** | 0.000 | 0.114 | Positive | |
| f²: A measure of effect size used to assess the strength of a relationship between variables in a regression model; Pr(>|t|): The p-value for each test; R²: coefficient of determination. *p < 0.05; **p < 0.01; ***p < 0.001. |
||||||
In addition, Appendix 3 summarizes the results of the path analysis, including R² values for dependent variable, path coefficients, significance levels (based on t-values from bootstrapping), and Cohen’s f² effect sizes. The data presented in Appendix 2 support the testing of 16 hypotheses (H1–H16), showing both expected and unexpected influences of health literacy dimensions on perceived ease of use, usefulness, trust, attitude, and behavioral intention. Statistically significant relationships (p < 0.05) highlight the explanatory power of the model and the central role of health literacy in teleconsultation adoption.
The table supports the testing of 16 hypotheses (H1–H16), showing both expected and unexpected influences of health literacy dimensions on perceived ease of use, usefulness, trust, attitude, and behavioral intention. Statistically significant relationships (p < 0.05) highlight the explanatory power of the model and the central role of health literacy in teleconsultation adoption. The PLS-PM approach does not offer an index estimating the overall quality of the model. To address this limit, Tenenhaus et al.20 developed an indicator for the overall fit quality of a model: the GoF indicator. The results for GoF indices in our model are satisfactory. The absolute GoF close to 0.66 is well above the 0.36 value recommended by Wetzels et al.21 Similarly, the stability of the overall fit quality of the model is satisfactory, given there is no difference in the scores of the absolute GoF indices before and after bootstrap (Table 5).
The results confirm the robustness of the proposed model and highlight the significant role of health literacy in shaping perceptions and behavioral intentions regarding medical teleconsultation. All hypothesized paths were statistically significant, supporting both expected and unexpected relationships. Notably, two dimensions of health literacy—understanding and access—were found to negatively influence perceived usefulness, contrary to initial assumptions.
These surprising results call for a deeper exploration of the contextual and psychological factors that might explain such counterintuitive effects. The following discussion section elaborates on these findings, providing interpretations and implications in light of existing literature and the specificities of the French healthcare context.
Discussion
Statement of Principal Findings
Our initial hypothesis that people must have a good level of understanding of medical information to perceive the usefulness of teleconsultation is not confirmed. Furthermore, perceived understanding of medical information and perceived access to information have a negative impact on the perceived usefulness of teleconsultation.
This counterintuitive result (that higher levels of understanding and access to health information negatively influence the perceived usefulness of teleconsultation) warrants further reflection. One possible explanation is that individuals with higher health literacy feel more autonomous in managing minor health issues. Therefore, they are less likely to perceive teleconsultation as necessary. In contrast, when facing more serious symptoms, these patients may perceive teleconsultation as insufficient and favor conventional face-to-face consultations, which they associate with more complete clinical assessments and direct physical examination. Another interpretation may involve psychological mechanisms such as a preference for traditional interactions or overconfidence in self-diagnosis among highly literate individuals. These patients may view digital consultations as a step removed from the relational depth and diagnostic reliability they associate with in-person visits.
Moreover, this result may reflect cultural and contextual specificities of the French healthcare system. In France, strong value is placed on the relational dimension of care and the in-person presence of the physician. For health-literate individuals who are already confident navigating the healthcare system, the digital interface may be perceived as reducing the quality of care rather than enhancing it.
This interpretation is supported by contrasting evidence from other healthcare systems. For example, in Scandinavian countries, where digital health integration is more mature and patient trust in online systems is high, studies reveal that higher health literacy correlates positively with perceived usefulness and acceptance of teleconsultation. In contrast, research from Southern Europe and parts of Asia suggests that the acceptability of teleconsultation varies significantly depending on healthcare infrastructure, cultural expectations around medical care, and prior exposure to digital health tools. These comparative insights reinforce the idea that health literacy does not operate independently. Rather, it interacts with contextual variables such as healthcare norms, institutional trust, and perceived quality of digital services.
On the other hand, understanding and access to medical information have a positive influence on the perceived ease of use. A patient with good reading and writing skills will be more comfortable using teleconsultation. Our results indicate that the person’s ability to evaluate care has a positive but weak influence on trust in teleconsultation. It is probably less easy to evaluate the quality of the service obtained through teleconsultation because the medical relationship is built on interactions, such as the quality of auscultation and evaluation of the patient’s physical state, which are more difficult to do remotely because some physiological indicators of the state of health are no longer as accessible as they would be in a face-to-face observation. Confidence in teleconsultation is largely determined by the perceived ease of use and also has a strong influence on the perceived usefulness.
Intention to use teleconsultation is positively influenced by trust. These perceived usefulness and attitude toward use confirm the results of technology adoption models.12,13
Taken together, these findings provide strong empirical support for the central role of health literacy in shaping the adoption of medical teleconsultation. While not all effects were in the expected direction, the statistical significance and explanatory power of the literacy dimensions in the model confirm their critical influence on perception, trust, and ultimately behavioral intention. This reinforces the conclusion that health literacy is not a peripheral factor but a key determinant in the successful uptake of teleconsultation services in the French context.
Strengths and Limitations
Using a nationally representative sample of French adults, the present study provides evidence that teleconsultation adoption is associated with health literacy. A first strength of this study concerns the adaptation of measurement scales to assess health literacy and its application to a large representative sample of the French population. A second concerns the combination of a model of measurement with a model of technology adoption that can be considered as a model of technological literacy.
As for the limitations, the main concern is results that may seem counterintuitive at first, the significant but negative influence of literacy on the perceived usefulness of teleconsultation. The second concern is the contextual nature of the research, which limits the generalization of the results. A third limitation is the absence of data on whether respondents had previously used teleconsultation. Prior experience may influence not only perceived ease of use and usefulness but also trust and intention to adopt. Future research should incorporate this variable to better isolate the effects of health literacy from those of familiarity with digital health tools. The questionnaire did not include a specific item regarding prior use of teleconsultation. Although this information was not collected, previous experience with such services could influence user perceptions and behavioral intention. However, during the study, teleconsultations represented only 3.7% of general practitioners’ activity in France.
Interpretation in the Context of the Wider Literature
Patients who usually lack the understanding of medical information and access to health information have traditionally been expected to be dependent on medical providers and the healthcare system. According to certain studies, teleconsultation requires that people have good health literacy to express their symptoms because of the lack of face-to-face contact and auscultation. Usually, people with low literacy are considered less comfortable and confident with teleconsultation.2 At the same time for particular pathologies and for chronic diseases that need a straight patient follow-up, teleconsultation is a good way to build, step by step, a good base of health literacy, with the limitation that they require important dedicated human resources at the beginning before empowering the patient.
Implications for Policy, Practice, and Research
A first extension of this work is to identify the explanatory elements of the negative influence of two of the HL dimensions on the perceived usefulness of the TC. This would require, in an initial phase, conducting a qualitative study on the adoption of telemedicine by distinguishing between two groups of people: one with a high level of health literacy and one with a low level.
Finally, on a more practical level, this raises the question of the development of specific health teleservices depending on the level of literacy of the people to better respond to the needs of each category. This research highlights the need to consider the positioning of teleconsultation in relation to conventional consultation and self-management of disease through therapeutic education by identifying the health situations and patient profiles for which its use is judicious.
From this perspective, several practical strategies can be envisioned to reduce health literacy gaps and improve access to teleconsultation. These include the design of user-friendly platforms with simplified interfaces, which include implementation of communication training for healthcare professionals to better engage with patients remotely and deployment of support services such as helplines or digital navigators. Local health authorities and providers could also co-create tailored educational materials (e.g., pictorial guides, multilingual instructions) in collaboration with community stakeholders.
These approaches would contribute to a more inclusive deployment of teleconsultation services, particularly for vulnerable or digitally excluded populations. In addition to these practical implications, future research could further explore the relationship between health literacy and teleconsultation adoption through various methodological lenses. A first avenue would be to conduct longitudinal studies to observe how individuals’ health literacy evolves and how this affects their acceptance and sustained use of teleconsultation. Second, experimental or quasi-experimental research could evaluate the effectiveness of specific interventions (e.g., interface simplification, digital coaching, patient navigator programs) in improving adoption rates among populations with low health literacy. Third, comparative cross-national studies would help examine how different healthcare systems, digital infrastructures, and cultural factors influence this relationship. Finally, mixed-methods approaches combining quantitative surveys with qualitative interviews or user experience testing could provide a more nuanced understanding of patients’ decision-making processes and perceived barriers. These perspectives would enrich the field and contribute to more inclusive and effective e-health strategies.
Conclusions
This study confirms the significant role of health literacy in shaping the adoption of medical teleconsultation. By integrating key literacy dimensions into a TAM, we provide empirical evidence that health literacy influences patients’ perceptions, particularly ease of use, trust, and behavioral intention. Although some effects, such as the negative influence on perceived usefulness, were unexpected, they reflect the complexity of digital health engagement and the importance of contextual and cultural factors.
Our findings have both theoretical and practical relevance. They call for teleconsultation services that are better tailored to varying literacy levels through simplified platforms, professional training, and patient support systems. Health literacy should be considered a core factor in the design of inclusive digital health policies.
Future studies should build on these results using longitudinal, comparative, or mixed-methods approaches to further explore how literacy affects the adoption and sustainability of teleconsultation across different patient populations and healthcare systems.
Contributors
Dr. Rochette conceptualized the conceptual framework and conceived the draft. Both authors conducted the literature review and designed the quantitative data collection. Both authors wrote the original paper. Dr. Lebrument analyzed the data and wrote the results, and Dr. Rochette discussed the contributions.
Data Availability Statement (DAS), Data Sharing, Reproducibility, and Data Repositories
Requests for data can be made to the corresponding author.
Application of AI-Generated Text or Related Technology
Not applicable.
References
- Kickbusch I, Maag D. Health Literacy. In: Kris Heggenhougen and Stella Quah, editors. International Encyclopedia of Public Health. Vol 3. San Diego: Academic Press; 2008. pp. 204–211.
- Kjeldsted E, Lindblad KV, Bødtcher H, Sørensen DM, Rosted E, Christensen HG, et al. A population-based survey of patients’ experiences with teleconsultations in cancer care in Denmark during the COVID-19 pandemic. Acta Oncol. 2021;60(10):1352–60. https://doi.org/10.1080/0284186X.2021.1956688
- Nutbeam D. The evolving concept of health literacy. Soc Sci Med. 2008;67(12):2072–8. https://doi.org/10.1016/j.socscimed.2008.09.050
- Nutbeam D. Evaluating health promotion—progress. problems and solutions. Health Promot Int. 1998;13(1):27–44. https://doi.org/10.1093/heapro/13.1.27
- Sørensen K, Van den Broucke S, Fullam J, Doyle G, Pelikan J, Slonska Z, et al. Health literacy and public health: A systematic review and integration of definitions and models. BMC Public Health. 2012;12:80. https://doi.org/10.1186/1471-2458-12-80
- Osborne RH, Batterham RW, Elsworth GR, Hawkins M, Buchbinder R. The grounded psychometric development and initial validation of the Health Literacy Questionnaire (HLQ). BMC Public Health. 2013;13:1–7. https://doi.org/10.1186/1471-2458-13-658
- Sørensen K, Pelikan JM, Röthlin F, Ganahl K, Slonska Z, Doyle G, et al. Health literacy in Europe: comparative results of the European health literacy survey (HLS-EU). Eur J Public Health. 2015;25(6):1053–8. https://doi.org/10.1093/eurpub/ckv043
- Haun JN, Patel NR, French DD, Campbell RR, Bradham DD, Lapcevic WA. Association between health literacy and medical care costs in an integrated healthcare system: a regional population based study. BMC Health Serv Res. 2015;15:1–11. https://doi.org/10.1186/s12913-015-0887-z
- Pelikan JM, Ganahl K, Van den Broucke S, Sørensen K. Measuring health literacy in Europe: introducing the European health literacy survey questionnaire (HLS-EU-Q). In: Okan O, Bauer U, Levin-Zamir D, et al., editors. International handbook of health literacy. Bristol: Policy Press; 2019, p. 115–38.
- Jordan JE, Buchbinder R, Briggs AM, Elsworth GR, Busija L, Batterham R, et al. The health literacy management scale (HeLMS): a measure of an individual’s capacity to seek. understand and use health information within the healthcare setting. Patient Educ Couns. 2013;91(2):228–35. https://doi.org/10.1016/j.pec.2013.01.013
- Davis FD. Perceived usefulness. Perceived ease of use and user acceptance of information technology. MIS Q. 1989;13:319–40. https://doi.org/10.2307/249008
- Davis FD, Bagozzi RP, Warshaw PR. User acceptance of computer technology: a comparison of two theoretical models. Manag Sci. 1989;35:982–1003. https://doi.org/10.1287/mnsc.35.8.982
- Venkatesh V, Morris MG, Davis GB, Davis FD. User acceptance of information technology: toward a unified view. MIS Q. 2003;27(3):425–78. https://doi.org/10.2307/30036540
- Venkatesh V, Davis FD. A theoretical extension of the technology acceptance model: four longitudinal field studies. Manag Sci. 2000;46:186–204. https://doi.org/10.1287/mnsc.46.2.186.11926
- Gefen D, Karahanna E, Straub DW. Trust and TAM in online shopping: an integrated model. MIS Q. 2003;27(1):51–90. https://doi.org/10.2307/30036519
- Becker J-M, Klein K, Wetzels M. Hierarchical latent variable models in PLS-SEM: guidelines for using reflective-formative type models. Long Range Plann. 2012;45:359–94. https://doi.org/10.1016/j.lrp.2012.10.001
- Diamantopoulos A, Sarstedt M, Fuchs C, Wilczynski P, Kaiser S. Guidelines for choosing between multi-item and single-item scales for construct measurement: a predictive validity perspective. J Acad Mark Sci. 2012;40:434–49. https://doi.org/10.1007/s11747-011-0300-3
- MacKenzie SB, Podsakoff PM, Podsakoff NP. Construct measurement and validation procedures in MIS and behavioral research: integrating new and existing techniques. MIS Q. 2011;35:293–334. https://doi.org/10.2307/23044045
- Jarvis CB, MacKenzie SB, Podsakoff PM. A critical review of construct indicators and measurement model misspecification in marketing and consumer research. J Consum Res. 2003;30: 199–218. https://doi.org/10.1086/376806
- Tenenhaus M, Amato S, Esposito Vinzi V. A global goodness-of-fit index for PLS structural equation modelling. In: Proceedings of the XLII SIS Scientific Meeting 2004, p. 739–42.
- Wetzels M, Odekerken-Schröder G, Van Oppen C. Using PLS path modeling for assessing hierarchical construct models: guidelines and empirical illustration. MIS Q. 2009;33(1):177–95. https://doi.org/10.2307/20650284
- Barbeite FG, Weiss EM. Computer self-efficacy and anxiety scales for an Internet sample: testing measurement equivalence of existing measures and development of new scales. Computers in Human Behavior. 2004;20(1):1–5.
- Bhattacherjee A, Hikmet N. Physicians’ resistance toward healthcare information technologies: A dual-factor model. In 2007 40th Annual Hawaii International Conference on System Sciences (HICSS’07). 2007. (pp. 141–141). IEEE.
- Urstad KH, Andenaes R, Wahl AK, Kvarme LG, Helseth S, Moum T. The health literacy questionnaire: Initial validity testing in a Norwegian sample. HLRP: Health Literacy Research and Practice. 2020;4(4):e190–e199.
- Belanche D, Casaló LV, Flavián C. Integrating trust and personal values into the Technology Acceptance Model: The case of e-government services adoption. Cuad Econ Dir Empresa. 2012;15:192–204.
Copyright Ownership: This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0.
Appendix
| Construct | Definition | Items (n) | Type and source of measuring instrument |
| Literacy: understanding | The degree to which a person understands any written health information or instruction about treatment or medication. | 3 | HLQ: items measured on a Likert 5-point scale* |
| Literacy: access to medical information | The degree to which a person identifies the right information when needed and reliable sources of information. | 4 | HLQ: items measured on a Likert 5-point scale* |
| Literacy: health care evaluation | The degree to which a person feels able to assess whether the information is appropriate and the offer meets their health situation. | 4 | HLQ: items measured on a Likert 5-point scale* |
| Technological anxiety | The degree to which a person is uncomfortable using a particular piece of technology. | 2 | Adapted from Barbeite and Weiss, 2004 (22) |
| Resistance | The degree to which a person resists using new technology. | 3 | Adapted from Bhattacherjee and Hikmet, 2007 (23) |
| Perceived usefulness of medical teleconsultation | The degree to which a person believes that the use of medical teleconsultation improves his or her health management. | 5 | Items measured on a Likert 5-point scale |
| Perceived ease of use of medical teleconsultation | The degree to which a person believes that using medical teleconsultation would be free from effort. | 4 | Items measured on a Likert 5-point scale** |
| Trust in medical teleconsultation technology | The degree to which a person expects medical teleconsultation to have the functions required to monitor his or her health without malfunction. | 3 | Items measured on a Likert 5-point scale*** |
| Attitude toward using medical teleconsultation technology | Favorable or unfavorable feelings regarding the use behavior of medical teleconsultation. | 4 | Items measured on a Likert 5-point scale** |
| Intention to use medical teleconsultation technology | The degree to which a person expresses willingness to use medical teleconsultation. | 3 | Items measured on a Likert 5-point scale** |
| Source: Urstad et al.24; **Davis11; Venkatesh et al.13; ***Gefen et al.15; Belanche et al.25. Tool: HLQ: Health Literacy Questionnaire. |
|||
Addendum
Defining Acronyms
AVE: Average variance extracted
GoF: Goodness of fit
HL: Health literacy
HLQ: Health Literacy Questionnaire
HLS-EU: Health Literacy Survey-Europe
PLS-PM: Partial least squares path modeling
PLS-SEM: Partial least squares structural equation modeling
REALM: Rapid Estimate of Adult Literacy in Medicine
TAM: Technology acceptance model
TOPHLA: Test of Functional Health Literacy in Adults