NARRATIVE/SYSTEMATIC REVIEWS/META-ANALYSIS
Continuous Patient Monitoring in Healthcare: A Comprehensive Review of Opportunities, Challenges, and Future Directions
K. Hima Bindu, MBBS, MD, FNB1  ; Sai Praveen Haranath, MBBS, MPH, FCCP Internal Medicine, Pulmonary and Critical Care Medicine2
; Sai Praveen Haranath, MBBS, MPH, FCCP Internal Medicine, Pulmonary and Critical Care Medicine2  Ravi Prakash Mahajan, MD, DM, FCAI (Hon), FRCA3
Ravi Prakash Mahajan, MD, DM, FCAI (Hon), FRCA3  ; K. Subba Reddy MBBS, MD, PDCC, IDCCM, EDIC, FICCM4
; K. Subba Reddy MBBS, MD, PDCC, IDCCM, EDIC, FICCM4  ; Rahul Khandelwal, MBBS5
; Rahul Khandelwal, MBBS5  ; Sneha Varahala, PharmD, MPH6
; Sneha Varahala, PharmD, MPH6 
1Critical Care, Consultant Critical Care, Apollo Hospitals Jubliee Hills, Hyderabad, India; 2Senior Consultant Pulmonologist & Critical Care Specialist, Medical Director, Apollo eACCESS TeleICU Service, Apollo Hospitals, Jubilee Hills, Hyderabad, India; 3Director, Critical Care Integration and Transformation, Apollo Hospitals Group, Director, Research and Innovation, Apollo Hospitals Group, Professor Emeritus, University of Nottingham, Nottingham, UK; 4Senior Consultant, Head of Critical Care Medicine, Apollo Hospitals, Jubliee Hills, Hyderabad, India; 5Chief Operations Officer, Tele ICU project, Apollo Hospitals, Jubliee Hills, Hyderabad, India; 6Mailman School of Public Health, Columbia University Irving Medical Center, New York, NY, USA
Keywords: Digital health, continuous monitoring, early warning systems, patient safety, remote patient monitoring, telemedicine, wearable sensors
Abstract
Traditional patient monitoring practices, particularly in general hospital wards, rely heavily on intermittent vital sign assessments, creating significant risk for undetected clinical deterioration. Continuous patient monitoring (CPM) using wearable sensor technologies represents a transformative shift toward real-time, proactive healthcare. This review explores the integration of wearable devices into clinical practice, highlighting their potential to improve patient outcomes by enabling early detection, enhancing patient mobility, and reducing preventable adverse events.
Wearable sensors offer continuous physiological data collection in both inpatient and remote care settings, enabling timely interventions and reducing hospital readmissions and ICU transfers. Evidence supports their effectiveness in managing chronic diseases such as diabetes and heart failure, as well as in acute care scenarios. Moreover, RPM platforms extend these benefits to home care environments, increasing healthcare access and continuity.
Despite these advantages, widespread implementation faces several challenges, including alarm fatigue, data overload, technical integration issues, patient comfort, and cybersecurity concerns. The review discusses strategies to overcome these barriers, including intelligent alarm systems, AI-powered analytics, streamlined workflows, and standardized interoperability.
Future research priorities include optimizing data-driven decision support tools, improving predictive algorithms, and rigorously evaluating the cost-effectiveness and clinical impact of continuous monitoring technologies. Addressing ethical and regulatory frameworks is also critical to ensuring patient trust and technology adoption.
In conclusion, CPM with wearable sensors holds significant promise for transforming healthcare delivery into a more responsive, preventative, and personalized model, contingent on resolving implementation challenges and leveraging evolving technologies.
Plain Language Summary
While continuous vital sign monitoring is standard in intensive care units, patients in general wards often receive intermittent monitoring, potentially delaying the detection of clinical deterioration. Wearable sensors offer a promising solution by enabling continuous, real-time data capture for a wide range of physiological parameters. This review examines the potential of wearable technology to enhance patient care in various healthcare settings, highlighting its capacity for personalized interventions, improved patient outcomes, and reduced alarm burdens. The authors discuss the advantages, challenges, and future directions of wearable technology in remote patient monitoring, emphasizing the need for further clinical research to validate its impact on clinical outcomes and optimize its integration into existing healthcare systems.
Citation: Telehealth and Medicine Today © 2025, 10: 562
DOI: https://doi.org/10.30953/thmt.v10.562
Copyright: © 2025 The Authors. This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0.
Submitted: March 12, 2025; Accepted: March 12, 2025; Published: July 9, 2025
Corresponding Author: K. Hima Bindu, himabindukotamarthy@gmail.com
Competing interests and funding: No funding was sourced for writing the article.
There are no conflicts of interests.
Continuous Patient Monitoring with Wearable Sensors: A Paradigm Shift in Patient Safety
Although traditional intermittent patient monitoring is a fundamental aspect of healthcare delivery, it suffers from inherent limitations. Relying on infrequent manual assessments creates vulnerabilities, particularly during periods of reduced staffing, where subtle yet clinically significant deteriorations in a patient’s condition can be missed.1,2 This delay in detection can have cascading consequences, leading to an increased risk of unplanned ICU admissions, prolonged hospital stays, and potentially preventable fatalities.3,4
Several studies underscore the critical need to address the shortcomings of intermittent monitoring. For example, McGloin et al.,5 demonstrated a concerning correlation between missed physiological deteriorations and adverse patient outcomes, including preventable deaths and ICU admissions. Furthermore, research suggests that physiological warning signs often precede life-threatening events by 8 to 24 h, highlighting a critical window of opportunity for intervention that traditional monitoring often fails to capture.6,7 Respiratory rate, a sensitive indicator of impending deterioration, exemplifies this challenge, as it is frequently not accurately recorded or acted upon in a timely manner.4
Continuous patient monitoring (CPM), particularly with the advent of sophisticated yet user-friendly wearable sensors, offers a compelling solution to bridge these gaps and usher in a new era of proactive, data-driven patient care.8 Unlike intermittent checks, wearable sensors provide a constant stream of physiological data, acting as vigilant sentinels against unseen deterioration. This real-time insight empowers healthcare providers with the information needed to intervene proactively, potentially mitigating risks before they escalate into crises.1,6
The advantages of wearable sensor technology extend beyond early detection, offering a compelling blend of patient-centric and system-level benefits.
Enhanced Patient Comfort and Mobility
Wearable sensors promote patient comfort and mobility by eliminating the need for bulky, restrictive bedside monitors. This enhanced mobility reduces the risk of complications associated with prolonged immobility, such as pressure ulcers and pneumonia, while simultaneously improving the patient experience.9–12
Shifting From Reactive to Proactive Care
Continuous patient monitoring facilitates a fundamental shift in healthcare delivery, moving away from a reactive approach where interventions occur after an event to a proactive model where potential problems are identified and addressed before they escalate. This proactive approach improves patient outcomes and has the potential to reduce healthcare costs by preventing costly hospital admissions and intensive care stays.13,14 While there is an initial investment required to set up a remote monitoring system, the overall cost of care can still be lower. If a patient can be effectively monitored from the ward with ICU-level oversight, it is often more cost-efficient than transferring them to the ICU.
Optimized Workflow and Enhanced Data Accuracy
Automated data capture and transmission streamline documentation processes, freeing up valuable nursing time for direct patient care and reducing the risk of human error. Furthermore, the continuous, objective data derived from wearable sensors provide a more comprehensive and accurate representation of a patient’s physiological status compared to intermittent manual assessments, empowering clinicians to make more informed clinical decisions (Figure 1).1,15–17
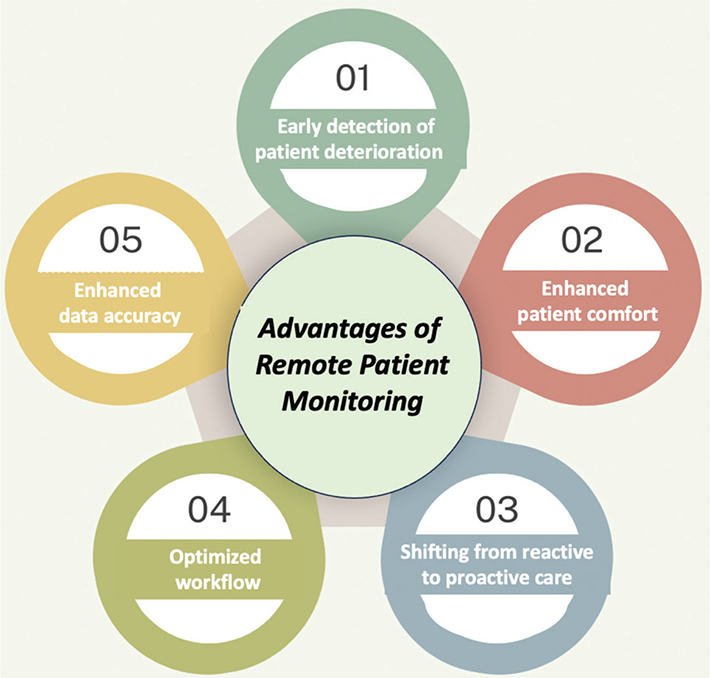
Fig. 1. Advantages with the remote patient monitoring system.
The convergence of miniaturization, extended battery life, and seamless wireless communication has fostered rapid innovation in the field of wearable sensor technology.8,18 These advancements have led to the development of increasingly sophisticated yet affordable devices capable of capturing a wide array of physiological parameters.19–23 As technology continues to evolve, wearable sensors are poised to become indispensable tools in healthcare, facilitating a paradigm shift from reactive interventions to proactive, data-driven care that prioritizes patient well-being and paves the way for a future of improved patient outcomes.1,24
Continuous Monitoring with Wearables: Transforming Patient Outcomes
The integration of CPM, particularly leveraging wearable sensor technology, is revolutionizing healthcare delivery by enabling a proactive, data-driven approach that significantly improves patient outcomes. With robust data collection in place, we can integrate predictive analytics powered by AI to proactively stratify patients based on their risk of ICU transfer—even before clinical deterioration occurs. This paradigm shift from reactive interventions to continuous, real-time insights into a patient’s physiological status empowers healthcare providers to identify and address potential health issues early, mitigating complications, reducing hospital stays, and ultimately improving patient well-being across diverse clinical settings.1–4,25
Early Detection and Intervention: The Cornerstone of Improved Outcomes
One of the most compelling benefits of CPM lies in its ability to detect subtle changes in a patient’s condition that might otherwise go unnoticed with traditional intermittent assessments 8,13,18,26,27 This early detection is particularly crucial for:
Managing Chronic Conditions
Early intervention is essential for managing conditions such as diabetes, cardiovascular disease, and respiratory disorders. Studies reveal that continuous glucose monitoring in patients with diabetes leads to better glycemic control, reducing the risk of long-term complications such as neuropathy and retinopathy.5,6,28,29
Enhancing Acute Care
The application of CPM has demonstrated a significant impact in acute care settings as well. Research, such as the study by Harvey et al.,2 revealed that implementing a contactless monitoring system in a medical-surgical ward was associated with a decrease in both ICU transfers and overall hospital length of stay. This improvement can be attributed to the early detection of clinical deterioration, enabling timely interventions that prevent patients from deteriorating to the point of requiring intensive care.7,9–11
Expanding Reach Through Remote Patient Monitoring
The benefits of CPM extend beyond hospital walls through remote patient monitoring technologies. Wearable sensors, coupled with telehealth platforms, allow for continuous monitoring of patients in home-based settings, such as those receiving home care or undergoing rehabilitation.12,14,15 This accessibility is particularly valuable for patients who have limited access to healthcare providers, ensuring timely interventions and reducing the need for unnecessary hospital visits.16,17,19,20 It also enhances access to care for patients in remote settings, where critical care physicians can monitor and manage cases effectively from a distance.
Patient-Centric Design for Enhanced Comfort and Compliance
Beyond its clinical impact, the use of wearable sensors for CPM offers a patient-centric approach to monitoring. These devices are typically discreet, comfortable, and minimize the disruption associated with frequent manual vital sign checks, particularly during periods of rest.21–24 This patient-centric design can lead to improved comfort, compliance, and satisfaction with their care.30–33
The integration of CPM and wearable sensor technology represents a transformative shift in healthcare, moving from reactive interventions to proactive, data-driven care. While further research is warranted to optimize implementation strategies and explore the full potential of these technologies across diverse patient populations, the existing evidence strongly supports their role in improving patient outcomes and transforming healthcare delivery.34–36
Challenges and Limitations of Continuous Monitoring Technologies
Despite the immense potential of continuous monitoring to revolutionize patient care, several challenges and limitations require careful consideration and proactive solutions (Figure 2).
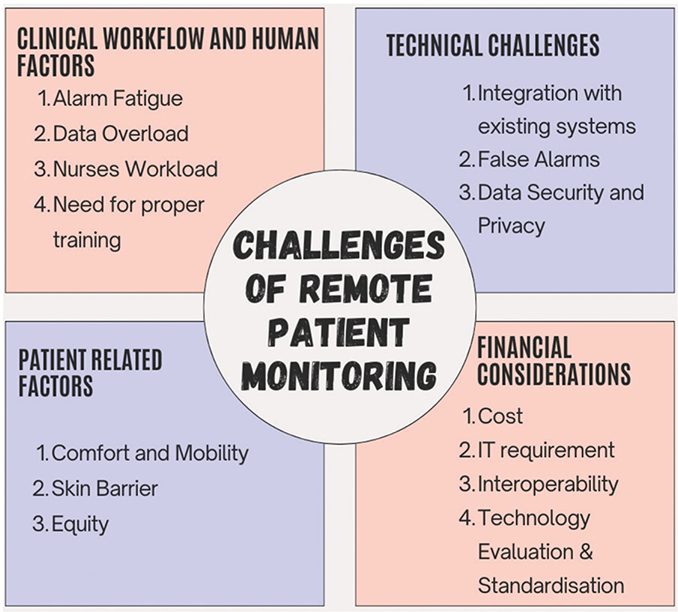
Fig. 2. Challenges with remote patient monitoring systems. IT: information technology.
Clinical Workflow and Human Factors
Alarm Fatigue
The high volume of alarms generated by continuous monitoring systems can lead to alarm fatigue among healthcare providers, increasing the risk of missing critical events. Implementing smart alarm systems that filter non-actionable alerts and leveraging predictive analytics to anticipate deterioration can mitigate this risk.12,14,24,36
Data Overload
The sheer volume of data generated can overwhelm clinicians. Advanced data visualization tools and AI-powered decision support systems are crucial for prioritizing critical information and facilitating timely interventions.25,26,34
Nurses’ Workload
Integrating continuous monitoring into existing workflows requires careful planning to avoid overburdening nurses. Efficient training programs and user-friendly interfaces are essential to streamline processes and maximize the technology’s benefits.30,31
Training
Comprehensive training programs for healthcare providers are non-negotiable. These programs must cover proper device use, data interpretation, and effective response to alerts, ensuring patient safety and optimal utilization of the technology.30,31,34
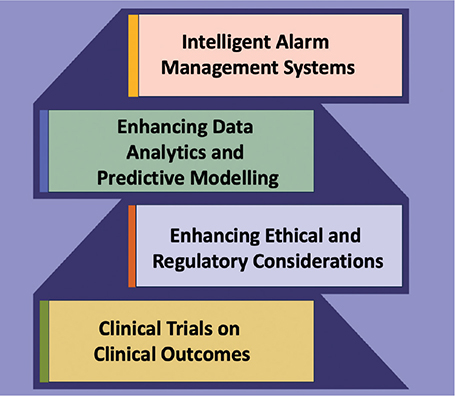
Fig. 3. The future research and directions of remote patient monitoring.
Technical Challenges
Integration with Existing Systems
Seamless integration with electronic health records (EHR) and clinical workflows is crucial for data accessibility and informed decision-making. Standardized interoperability protocols and dedicated information technology (IT) support are essential for successful implementation.12,16,24,29,30
False Alarms
Technical glitches and patient movement can trigger false alarms, reducing system reliability and increasing workload. Investing in advanced sensors with higher accuracy and developing algorithms that minimize false positives are key areas for improvement.14,15,24,30
Data Security and Privacy
Robust cybersecurity measures are paramount to protecting sensitive patient data. Compliance with privacy regulations, secure data encryption, and strict access controls are essential for maintaining patient trust and confidentiality.17,19,20
Patient-Related Factors
Comfort and Mobility
Balancing the need for continuous monitoring with patient comfort and mobility is essential. Utilizing comfortable and minimally invasive sensors, along with clear communication about the monitoring process, can improve patient experience and compliance.23,24
Skin Barrier
Some individuals may experience skin irritation or allergic reactions to adhesive sensors. Exploring alternative attachment methods and hypoallergenic materials can minimize these risks.21,22
Financial and Infrastructure Considerations
Cost
While the initial investment in continuous monitoring technology may be substantial, its long-term cost-effectiveness—evidenced by reduced hospital readmissions and shorter lengths of stay—makes a strong case for its adoption. Moreover, this upfront cost remains significantly lower than the expenses associated with ICU treatment.1,13
Information technology Infrastructure and Interoperability
Robust IT infrastructure, including reliable network connectivity and seamless EHR interoperability, is fundamental for real-time data transmission, analysis, and utilization.24,29,30
Technology Evaluation and Standardization
The rapid evolution of sensor technology necessitates rigorous evaluation and standardization to ensure accuracy, reliability, and interoperability across different systems.33,34
By proactively addressing these challenges and limitations, we can unlock the full potential of continuous monitoring technologies to transform healthcare delivery, improve patient outcomes, and create a more efficient and patient-centered healthcare system.
Equity and adoption considerations
While continuous monitoring and wearable sensor technologies hold significant promise for transforming healthcare delivery, their adoption is not uniformly accessible across all populations. Digital literacy and health literacy play a crucial role in how effectively patients can engage with these tools. In addition, social determinants of health—including socioeconomic status, access to technology, and educational background—may create disparities in who benefits from these innovations. To ensure equitable implementation, it is essential to incorporate user-friendly designs, provide patient and caregiver education, and address structural barriers to access. Strategies that include community engagement and culturally sensitive communication can further support inclusive adoption.
Future Directions and Research Priorities
To fully realize the transformative potential of CPM, several key areas require further research and development:
Developing an Intelligent Alarm Management System
Future research should prioritize the development of intelligent alarm management systems that incorporate artificial intelligence and machine learning to minimize false alarms, prioritize clinically significant alerts, and deliver context-aware notifications to healthcare providers. In parallel, a cost-effective and immediately implementable strategy involves conducting a comprehensive inventory of existing alarms to identify and deactivate those that are redundant or offer limited clinical value. The integration of both approaches is essential to reducing alarm fatigue, enhancing patient safety, and improving the overall efficiency of clinical workflows.32–34
Enhancing Data Analytics and Predictive Modeling
Advanced data analytics techniques, including machine learning and deep learning, hold immense potential for extracting meaningful insights from CPM data. Future research should focus on developing and validating robust algorithms for predicting adverse events, personalizing treatment plans, and identifying high-risk patients who will benefit most from CPM.11,12,15,16
Addressing Ethical and Regulatory Considerations
As CPM becomes more sophisticated and integrated into healthcare systems, it is crucial to address the ethical and regulatory considerations surrounding data privacy, security, and informed consent. Establishing clear guidelines and best practices for data governance, transparency, and patient empowerment will be essential for fostering trust and ensuring the responsible use of CPM technologies.17,19,20,22
Evaluating the Impact of Continuous Patient Monitoring on Clinical Outcomes and Cost-Effectiveness
Rigorous clinical trials and real-world studies are needed to evaluate the impact of CPM on patient outcomes, healthcare utilization, and overall cost-effectiveness. This evidence base will be crucial for informing clinical guidelines, reimbursement policies, and investment decisions.13,14,33,36
Conclusion
This review highlights the growing relevance of CPM in modern healthcare, emphasizing the potential benefits and the challenges of widespread adoption. Healthcare practitioners increasingly recognize the value of telemonitoring and remote patient monitoring for personalized care and improved patient outcomes. However, addressing concerns regarding data security, alarm fatigue, digital equity, and integration with existing workflows is crucial for wider acceptance.
Technological advancements, particularly in wearable technology and artificial intelligence, offer promising solutions. Wearable sensors enable continuous data collection, while AI-powered predictive analytics can minimize false alarms and enhance the accuracy of early warning systems.
Successful integration of continuous monitoring into healthcare relies heavily on robust IT infrastructure, standardized technologies, and seamless EHR interoperability. The overall return on investment (ROI) is likely to be positive, provided that the monitoring system is well-integrated and the clinical workflow is appropriately designed to support its use. Future research should focus on optimizing these areas, as well as evaluating the impact of continuous monitoring on clinical outcomes across diverse patient populations. By addressing the existing challenges and harnessing the power of emerging technologies, CPM can transform healthcare delivery, leading to improved patient outcomes, optimized resource allocation, and a more proactive and preventative approach to healthcare.
Contributors
Dr. K Hima Bindu, Dr. Sai Praveen Haranarth, Prof. Ravi Prakash Mahajan, Dr. Rahul Khandelwal, Dr. Subbareddy, Dr. Sneha Varahala
Data availability Statement (DAS): Data Sharing, Reproducibility, and Data Repositories
This article is a review of previously published literature and does not involve the generation of new data. All sources of information have been appropriately cited and are available in the public domain. No additional datasets were generated or analyzed for this study.
Data Sharing
This review article is based entirely on previously published data, which are publicly accessible through the original sources cited within the manuscript. As no new datasets were generated, data sharing is not applicable.
Application of AI-Generated Text or Related Technology
None
References
- Joshi M, Ashrafian H, Aufegger L, Khan S, Arora S, Cooke G, et al. Wearable sensors to improve detection of patient deterioration. Expert Rev Med Devices. 2019;16(2):145–54. https://doi.org/10.1080/17434440.2019.1563480
- Brown H, Terrence J, Vasquez P, Bates DW, Zimlichman E. Continuous monitoring in an inpatient medical-surgical unit: a controlled clinical trial. Am J Med. 2014;127(3):226–32. https://doi.org/10.1016/j.amjmed.2013.12.004
- Downey CL, Chapman S, Randell R, Brown JM, Jayne DG. The impact of continuous versus intermittent vital signs monitoring in hospitals: a systematic review and narrative synthesis. Int J Nurs Stud. 2018;84:19–27. https://doi.org/10.1016/j.ijnurstu.2018.04.013
- Centre for Clinical Practice at NICE (UK): acutely ill patients in hospital: recognition of and response to acute illness in adults in hospital. National Institute for Health and Clinical Excellence; 2007.
- McGloin H, Adam SK, Singer M. Unexpected deaths and referrals to intensive care of patients on general wards. Are some cases potentially avoidable? J R Coll Physicians Lond. 1999;33(3):255–9. https://doi.org/10.1016/S0035-8819(25)01722-2
- Goldhill DR, White SA, Sumner A. Physiological values and procedures in the 24 hours before ICU admission from the wards. Anaesthesia. 1999;54:529–34. https://doi.org/10.1046/j.1365-2044.1999.00837.x
- Mapp ID, Davis LL, Krowchuk H. Prevention of unplanned intensive care unit admissions and hospital mortality by early warning systems. Dimens Crit Care Nurs. 2013;32(6):300–9. https://doi.org/10.1097/DCC.0000000000000004
- Hernandez-Silveira M, Ahmed K, Ang S-S, Zandari F, Mehta T, Weir R, et al. Assessment of the feasibility of an ultra-low power, wireless digital patch for the continuous ambulatory monitoring of vital signs. BMJ Open. 2015;5(5):e006606. https://doi.org/10.1136/bmjopen-2014-006606
- Ludikhuize J, Borgert M, Binnekade J, Subbe C, Dongelmans D, Goossens A. Standardized measurement of the modified early warning score results in enhanced implementation of a rapid response system: a quasi-experimental study. Resuscitation. 2014;85(5):676–82. https://doi.org/10.1016/j.resuscitation.2014.02.009
- Weenk M, Koeneman M, van de Belt TH, Engelen LJLPG, van Goor H, Bredie SJH. Wireless and continuous monitoring of vital signs in patients at the general ward. Resuscitation. 2019;136:47–53. https://doi.org/10.1016/j.resuscitation.2019.01.017
- Boatin AA, Wylie BJ, Goldfarb I, Azevedo R, Pittel E, Ng C, et al. Wireless vital sign monitoring in pregnant women: a functionality and acceptability study. Telemed J E Health. 2016;22(7):564–71. https://doi.org/10.1089/tmj.2015.0173
- Zubiete ED, Luque LF, Rodríguez AVM, González IG. Review of wireless sensors networks in health applications. Ann Int Conf IEEE Eng Med Biol Soc. 2011;2011:1789–93. https://doi.org/10.1109/IEMBS.2011.6090510
- Kaboli PJ, Rosenthal GE. Delays in transfer to the ICU: a preventable adverse event? J Gen Intern Med. 2003;18:155–6. https://doi.org/10.1046/j.1525-1497.2003.21217.x
- Darwish A, Hassanien AE. Wearable and implantable wireless sensor network solutions for healthcare monitoring. Sensors (Basel). 2011;11(6):5561–95. https://doi.org/10.3390/s110605561
- Ohashi K, Kurihara Y, Watanabe K, Ohno-Machado L, Tanaka H. Feasibility evaluation of Smart Stretcher to improve patient safety during transfers. Methods Inf Med. 2011;50(3):253–64. https://doi.org/10.3414/ME0616
- Noah B, Keller MS, Mosadeghi S, Stein L, Johl S, Delshad S, et al. Impact of remote patient monitoring on clinical outcomes: an updated meta-analysis of randomized controlled trials. NPJ Digit Med. 2018;1(1):20172. https://doi.org/10.1038/s41746-017-0002-4
- Sahandi R, Noroozi S, Roushan G, Heaslip V, Liu Y. Wireless technology in the evolution of patient monitoring on general hospital wards. J Med Eng Technol. 2010;34(1):51–63. https://doi.org/10.3109/03091900903336902
- Michard F, Gan TJ, Kehlet H. Digital innovations and emerging technologies for enhanced recovery programmes. Br J Anaesth. 2017;119(1):31–9. https://doi.org/10.1093/bja/aex140
- Buist MD, Jarmolowski E, Burton PR, Bernard SA, Waxman BP, Anderson J. Recognising clinical instability in hospital patients before cardiac arrest or unplanned admission to intensive care. A pilot study in a tertiary-care hospital. Med J Aust. 1999;171(1):22–5. https://doi.org/10.5694/j.1326-5377.1999.tb123492.x
- Schein RM, Hazday N, Pena M, Ruben BH, Sprung CL. Clinical antecedents to in-hospital cardiopulmonary arrest. Chest. 1990;98(6):1388–92. https://doi.org/10.1378/chest.98.6.1388
- Tarar A. Wearable skin sensors and their challenges: a review of transdermal, optical, and mechanical sensors. Biosensors. 2020;10(6):56. https://doi.org/10.3390/bios10060056
- Khatsenko K, Khin Y, Maibach H. Allergic contact dermatitis to components of wearable adhesive health devices. Dermatitis. 2020;31(5):283–6. https://doi.org/10.1097/DER.0000000000000575
- Weenk M, Bredie SJ, Koeneman M, Hesselink G, van Goor H, van de Belt TH. Continuous monitoring of vital signs in the general ward using wearable devices: randomized controlled trial. J Med Internet Res. 2020;22(6):e15471. https://doi.org/10.2196/15471
- Prgomet M, Cardona-Morrell M, Nicholson M, Lake R, Long J, Westbrook J, et al. Vital signs monitoring on general wards: clinical staff perceptions of current practices and the planned introduction of continuous monitoring technology. Int J Qual Health Care. 2016;28(4):515–21. https://doi.org/10.1093/intqhc/mzw062
- Alam N, Hobbelink EL, van Tienhoven AJ, van de Ven PM, Jansma EP, Nanayakkara PWB. The impact of the use of the early warning score (EWS) on patient outcomes: a systematic review. Resuscitation. 2014;85(5):587–94. https://doi.org/10.1016/j.resuscitation.2014.01.013
- Downey CL, Tahir W, Randell R, Brown JM, Jayne DG. Strengths and limitations of early warning scores: a systematic review and narrative synthesis. Int J Nurs Stud. 2017;76:106–19. https://doi.org/10.1016/j.ijnurstu.2017.09.003
- Haller G, Myles PS, Wolfe R, Weeks AM, Stoelwinder J, McNeil J. Validity of unplanned admission to an intensive care unit as a measure of patient safety in surgical patients. Anesthesiology. 2005;103(6):1121–9. https://doi.org/10.1097/00000542-200512000-00004
- Beckett D, Gordon C, Paterson R, Chalkley S, Macleod D, Bell D. Assessment of clinical risk in the out of hours hospital prior to the introduction of Hospital at Night. Acute Med. 2009;8(1):33–8. https://doi.org/10.52964/AMJA.0229
- Chan M, Estève D, Fourniols J-Y, Escriba C, Campo E. Smart wearable systems: current status and future challenges. Artif Intell Med. 2012;56(3):137–56. https://doi.org/10.1016/j.artmed.2012.09.003
- Kowalski R, Capan M, Lodato P, Mosby D, Thomas T, Arnold R, et al. Optimizing usability and signal capture: a proactive risk assessment for the implementation of a wireless vital sign monitoring system. J Med Eng Technol. 2017;41(8):623–9. https://doi.org/10.1080/03091902.2017.1382589
- Kooij L, Peters GM, Doggen CJM, van Harten WH. Remote continuous monitoring with wireless wearable sensors in clinical practice, nurses perspectives on factors affecting implementation: a qualitative study. BMC Nurs. 2022;21(1):53. https://doi.org/10.1186/s12912-022-00832-2
- Leenen JPL, Leerentveld C, van Dijk JD, van Westreenen HL, Schoonhoven L, Patijn GA. Current evidence for continuous vital signs monitoring by wearable wireless devices in hospitalized adults: systematic review. J Med Internet Res. 2020;22(6):e18636. https://doi.org/10.2196/18636
- Weenk M, van Goor H, Frietman B, Engelen LJ, van Laarhoven CJ, Smit J, et al. Continuous monitoring of vital signs using wearable devices on the general ward: pilot study. JMIR MHealth UHealth. 2017;5(7):e91. https://doi.org/10.2196/mhealth.7208
- Ruppel H, Funk M, Whittemore R, Wung S-F, Bonafide CP, Powell Kennedy H. Critical care nurses’ clinical reasoning about physiologic monitor alarm customisation: an interpretive descriptive study. J Clin Nurs. 2019;28(15–16):3033–41. https://doi.org/10.1111/jocn.14866
- Dash S, Shakyawar SK, Sharma M, Kaushik S. Big data in healthcare: management, analysis and future prospects. J Big Data. 2019;6(1):54. https://doi.org/10.1186/s40537-019-0217-0
- Sendelbach S, Funk M. Alarm fatigue. AACN Adv Crit Care. 2013;24:378–86. https://doi.org/10.4037/NCI.0b013e3182a903f9
Copyright Ownership: This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0.