ORIGINAL RESEARCH
Evaluation of an Effective Telehealth Model for Healthcare Services for the Homeless: The Remote Area Medical Experience
Joslyn Russell1, Kim Worley2, Amanda Weber, MS2, Holly Smith, AS, AEMT, NREMT2, Stephen Blackstock2 and Paul Hart, MD3 
1Senior Student Volunteer, University of South Dakota, Vermillion, South Dakota, USA; 2RAM (Remote Area Medical Volunteer Corp), Rockford, Tennessee, USA; 3Formerly, Volunteer Physician, University of Massachusetts Medical School, Worcester, Massachusetts, USA
Keywords: access barriers, chronic disease management, healthcare, homeless, remote area medical, telehealth
Abstract
Telehealth is an increasingly used means of providing healthcare to the homeless. However, authors have noted barriers to offering healthcare using this option. Difficulty in reaching patients, inability to obtain basic vital signs, trouble providing necessary medications for common conditions, and problems with some individuals using the technology. Remote Area Medicine employs a different model to overcome these issues. Clinics are held within a homeless shelter with all the needed equipment. A nurse is present to obtain medical information and assist the providers by obtaining vital signs, etc. Basic medications are provided free of charge if the patient is uninsured. Additionally, a medical van has been outfitted with telehealth access to allow those patients not in the shelter to access care. This article documents 6 months of patient data showing the effectiveness of this program.
Plain Language Summary
Homeless individuals face profound challenges in accessing healthcare. Chronic conditions such as heart disease, diabetes, and HIV/AIDS are up to six times more prevalent in this population than in the public. In addition, mental health disorders occur 20% more frequently in this group. This study examines 6 months of data from Remote Area Medical’s (RAM) telehealth initiative, which integrates shelter-based clinics and mobile units to reduce healthcare barriers. The RAM hybrid model distinguishes itself from other telehealth efforts through its in-person support infrastructure, offering both flexibility and continuity of care. The findings underscore the feasibility and impact of this approach for improving care delivery among vulnerable populations.
Citation: Telehealth and Medicine Today © 2025, 10: 573 - https://doi.org/10.30953/thmt.v10.573
DOI: https://doi.org/10.30953/thmt.v10.573
Copyright: © 2025 The Authors. This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0. The authors of this article own the copyright.
Submitted: April 13, 2025; Accepted: July 15, 2025; Published: September 15, 2025
Corresponding Author: Paul Hart, Email: plh7275@gmail.com
Competing interests and funding: There are no conflicts of interest by any authors.
There were no funding sources for this research.
Homelessness in the United States continues to rise, with over 770,000 individuals experiencing homelessness as of January 2024—an 18% increase from 2023.1 This population’s access to preventative care, chronic disease management, and follow-up services is fragmented and frequently inadequate. Emergency departments often become the default care site, which drives up healthcare costs and compromises patient outcomes.
Living without a stable shelter exacerbates obstacles to health maintenance, including the inability to store medications, maintain hygiene, and access timely care. Furthermore, while telehealth shows promise, widespread implementation remains difficult due to low smartphone ownership, limited digital literacy, and financial barriers to connectivity. Nevertheless, telehealth models incorporating human support, such as onsite clinical staff, have improved marginalized populations’ satisfaction and outcomes.2
Established programs like Boston Health Care, Sharon, Massachusetts, US for the Homeless and the University of California, Los Angeles (UCLA), Mobile Clinic Project have demonstrated success, though many initiatives struggle to scale due to operational or funding limitations.
The Remote Area Medical (RAM) hybrid approach—delivering care via mobile units and shelter partnerships—addresses many systemic constraints. In addition, RAM’s annual budget is significantly lower ($80,000, €69,000) than that of the Boston and UCLA programs, reflecting its more focused scope and extensive volunteer participation.
Boston Health Care for the Homeless provides case managers, low-cost cell phones with unlimited minutes, and biweekly calls assessing equipment needs, medication access, food security, transportation, and utilities. In contrast, the RAM model provides only medical care, with a nurse onsite to assist the patient. Patients are seen either in shelters or in RAM’s mobile van. And the UCLA Mobile Clinic Project is state funded with a $25 million (€22 million) grant, and is largely run by students. It offers additional services (e.g., teleultrasound).
This observational study reviews 650 patient visits over 6 months in 2024.
Methods
The program design reflects current best practices in care for underserved populations, including integrated care coordination, nurse-led diagnostic support and embedded patient education. Similar approaches have increased healthcare engagement in prior studies treating vulnerable groups.2,3
Patients were seen at two primary sites: Knox Area Rescue Ministries (KARM) homeless shelter (400 beds), Knoxville, Tennessee, US, and CareCuts nongovernmental organization (NGO) mobile RAM van, Knoxville, Tennessee, US Each location is equipped with telehealth-ready examination rooms. Volunteer primary physicians and experienced volunteer nurses provided care. Nursing students were observed under instructor’s supervision. The nurse obtained vital signs, confirmed allergies and medications, and remained during consultations to assist with lung and heart auscultation, skin lesion photography, otoscope and throat examination, wound dressing, and sample medication provision. For hearing-impaired patients, nurses facilitated communication.
Prescriptions were called into a local pharmacy. Insured patients used their coverage, while donated funds assisted the uninsured. Controlled substances were not prescribed. If needed, referrals were made to a local physician group. The providers entered encounter data into an electronic medical record. For this research, the primary author reviewed each record to extract data for analysis into an Excel spreadsheet. Each patient received a number to maintain confidentiality.
Results
The data for the 650 patient visits during the first 6 months of 2024 were analyzed. The reasons for the patient visit, medical histories, and medications are listed in Table 1. The medical history entered was categorized into the following general areas based on the patient’s discussion with the nurse.
The patient population showed a concentration of middle-aged adults, with the majority falling between 40 and 59 years of age—aligning with US national demographics for unhoused populations. The distribution of gender reflected national statistics, with a higher proportion of males (61.1%). Acute care needs were the primary reason for visits; however, only 21% of patients returned for follow-up. The details of patient visits are listed in Table 2.
Approximately, 60% of patients did not have a primary care provider despite some having insurance coverage. Nearly one in five visits were for chronic medication refills, underscoring the demand for longitudinal care. The high percentage of patients with multiple visits suggests successful engagement with the telehealth program for ongoing care needs.
Antibiotics were prescribed in 43% of encounters—a notably higher rate than the 13.6% to 19.1% reported in studies of emergency settings (Denny et al., 2019 and that by Lowery et al)4 This might suggest an indication of inappropriate care. However, several studies reveal that homeless individuals who present for care have a greater need for antibiotics than housed individuals. A systematic review by Waddell et al.5 highlights that homeless individuals have a higher prevalence and incidence of various infectious diseases, which often necessitate antibiotic treatment. Furthermore, the study by Ly et al.6 on homeless individuals hospitalized in infectious disease units in Marseille, France, reported that respiratory tract infections, which typically require antibiotic treatment, were significantly more common among homeless patients compared with housed controls.
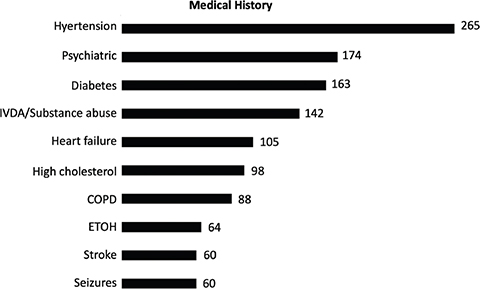
Fig. 1. Comparison of patient medical histories.
The most frequently prescribed medications were to treat hypertension, followed by psychiatric and respiratory medications. Over-the-counter medications such as acetaminophen/paracetamol, ibuprofen, and allergy medications were given to the patients, if required, at the time of the visit. The most frequently prescribed drugs are listed in Figure 2.
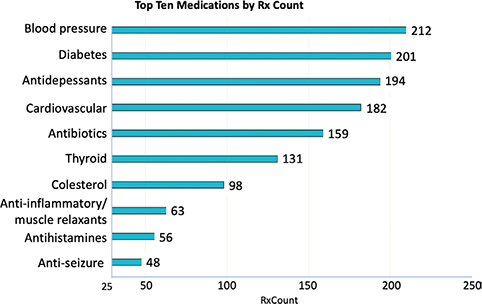
Fig. 2. The most frequently prescribed drugs.
Emergency department costs that were potentially avoided ranged from $945,000 to $2.83 million (€814,402 to €2.44 million). This is a stark contrast to the estimated $14,000 (€12,060) cost to operate the RAM telehealth program over the study period. The cost comparison is based on the FAIR Health (TalktoMira claim database, 2.5 billion records) inflation-adjusted estimate.7
More than 80% of patient encounters included education, compared to just 20% for insured individuals nationally.8
Unlike another report,9 psychiatric problems were not the primary reason for seeking care.
Discussion
The RAM telehealth model offers significant benefits in addressing healthcare gaps among homeless populations. Key strengths include the presence of trained nursing staff, the ability to initiate treatment immediately, and a flexible care delivery structure that adapts to patient mobility. Additionally, care is delivered in a very convenient manner. The shelter residents do not need an appointment or access to a telephone, and they are seen when they present for care during the three sessions per week when the telehealth is available. This also applies to the patients seen in the mobile van. The sites chosen are in areas where the unhoused frequent, providing easy access to care.
In “Experiences with Telehealth Among Homeless Older Adults,” in the study by Zahir and colleagues,10 participants reported significant challenges obtaining the necessary technology and connectivity for video visits. Notably, perceptions of telehealth differed by modality—many were skeptical of phone-only appointments for physical health issues (“I needed you to see…”), yet they expressed generally positive views of tele-mental health services.
Adams and colleagues2 reviewed their experience.5 Even though they had a smaller sample size of 125 patients, they concluded, “The survey results demonstrate that telehealth is a healthcare delivery method for people experiencing homelessness that is feasible, accepted by patients and providers, and increases access to healthcare. Using telehealth to increase access to care has the potential to reduce disparity in health outcomes for this vulnerable population and modify high-cost healthcare utilization patterns.
One area of concern is the risk of malpractice for the volunteer providers. The RAM provides malpractice insurance for all providers.
In an article published by Fogel and Kvedar,11 the authors noted that “based on data available from the USA before the pandemic, telemedicine claims made by patients increased by over 2,800% from December 2019 to December 2020, forming 6.5% of all medical malpractice claims in December 2020. To date, there have been no malpractice suits started or threatened against RAM or the providers.
One of the reasons that RAM has not had lawsuits may be our model of having visual contact between the patient and the provider. In a study by Zahir et al.,10 audio-only telehealth for physical health showed lower patient satisfaction among homeless populations, with participants expressing concerns that “without visual and tactile information, the clinician could not make a diagnosis.” This aligns with general telehealth malpractice trends where diagnostic errors are the primary concern. The RAM model with a nurse present with the patient avoids this issue, as individuals do not need to rely on having a cell phone or any technical knowledge to use an app and all patients were able to interact with their provider on the monitor.
Limitations
A matched comparison with local emergency room visits was not possible due to HIPAA constraints. We could not independently verify the accuracy of the medical history, medications said to be prescribed or results of any diagnostic tests that our patients reported.
Conclusion
RAM’s hybrid telehealth model provides an effective, practical, low-cost solution for delivering healthcare to homeless individuals. Integrating in-person nursing support and remote physician consultation improves care access, reduces emergency room reliance, and enhances health literacy. Future public health initiatives should consider adopting and expanding on this model to improve outcomes for underserved populations nationwide.
Author Contributions
The lead author reviewed all patient data and entered it into the spreadsheets. All the other authors contributed to the writing of the paper, reviewing each other’s suggestions and agreeing on the final format.
Data Availability Statement (DAS), Data Sharing, Reproducibility, and Data Repositories
All data are available for any researcher and will be provided by asking Dr. Hart. The results can be reproduced in any medical journal.
Application of AI-Generated Text or Related Technology
Artificial intelligence in Excel was used to help generate the charts and search for exact references.
Acknowledgments
We want to thank the KARM shelter and Care Cuts staff, whose support made this project possible.
References
- Tanya de Sousa T, Henry M. US Department of Housing and Urban Development. The 2024 annual homelessness assessment report (AHAR) to congress. The U.S. Department of Housing and Urban Development. [cited 2024 Dec 12]. Available from: https://www.huduser.gov/portal/sites/default/files/pdf/2024-AHAR-Part-1.pdf.
- Adams CS, Player MS, Berini CR, et al. A telehealth initiative to overcome healthcare barriers for people experiencing homelessness. Telemed E Health. 2021;27(8):851858. https://doi.org/10.1089/tmj.2021.0127
- DeLaCru-Jiron EJ, Hahn LM, Donahue AL, et al. Telemental health for the homeless population: lessons learned when leveraging care. Curr Psychiatry Rep. 2023;25(1):16. https://doi.org/10.1007/s11920-022-01400-w
- Denny KJ, Gartside JG, Alcorn K, et al. Appropriateness of antibiotic prescribing in the emergency department. J Antimicrob Chemother. 2019;74(2):515520. https://doi.org/10.1093/jac/dky447
- Waddell CJ, Saldana CS, Schoonveld MM, et al. Infectious diseases among people experiencing homelessness: a systematic review of the literature in the United States and Canada, 2003–2022. Public Health Reports (Washington, DC 1974). 2024;139(5):532548. https://doi.org/10.1177/00333549241228525
- Ly TDA, Dao TL, Hoang VT, Braunstein D, Brouqui P, Lagier JC, et al. Pattern of infections in French and migrant homeless hospitalised at Marseille infectious disease units, France: a retrospective study, 2017–2018. Travel Med Infect Dis. 2020;36:101768. https://doi.org/10.1016/j.tmaid.2020.101768
- FAIR Health tNGO. Total Navigation and Guidance Offering FAIR Health. 2025. https://www.fairhealthconsumer.org
- McClellan W. The physician and patient education: a review. Patient Educ Couns. 1986;8(2):151163. https://doi.org/10.1016/0738-3991(86)90086-8
- Barry R, Anderson J, Tran L, et al. Prevalence of mental health disorders among individuals experiencing homelessness: a systematic review and meta-analysis. JAMA Psychiatry. 2024;81(7):691–99. https://doi.org/10.1001/jamapsychiatry.2024.0426
- Zahir A, Yip D, Garcia C, Smith AN, Dhatt Z, Duke M, et al. “I Needed for You to See What I’m Talking About”: experiences with telehealth among homeless-experienced older adults. Gerontol & Geriatr Med. 2023;9:1–8. https://doi.org/10.1177/23337214231172650
- Fogel AL, Kvedar JC. Reported cases of medical malpractice in direct-to-consumer telemedicine. JAMA. 2019;321(13):1309–10. https://doi.org/10.1001/jama.2019.0395
Copyright Ownership: This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See http://creativecommons.org/licenses/by-nc/4.0. The authors of this article own the copyright.