ORIGINAL RESEARCH
Beyond Technology: Social Support, Risk, and Economic Value in Physicians’ Telemedicine Adoption in Indonesia
Elika Setiawaty, PhD1  , Hartoyo Hartoyo, PhD2
, Hartoyo Hartoyo, PhD2  , Rita Nurmalina, PhD3
, Rita Nurmalina, PhD3  and Lilik Noor Yuliati, PhD4
and Lilik Noor Yuliati, PhD4 
1School of Business, IPB University, Bogor, West Java, Indonesia; 2Professor, School of Business, IPB University, Bogor, West Java, Indonesia; 3Professor, Faculty of Economics and Management, IPB University, Bogor, West Java, Indonesia; 4Professor, Department of Family and Consumer Sciences, IPB University, Bogor, West Java, Indonesia.
Keywords: Actual use behavior, economic value, perceived digital risk, self-efficacy, social support, telemedicine adoption
Abstract
Objectives: Adoption of technology by physicians is critical to improving healthcare delivery. This study examines the direct impact of economic value, perceived risk, and social support on the actual use of technology by physicians in Indonesia. The authors extend the traditional technology acceptance model (TAM) by focusing on actual use rather than intention. It also tests self-efficacy as a moderating factor.
Methods: A cross-sectional survey was conducted with 244 physicians. The proposed model integrates core TAM constructs with self-efficacy as a moderator. The relationships were tested using partial least squares structural equation modeling.
Results: The model shows that economic value and social support positively influence physicians’ actual use, while perceived risk has a negative effect. Self-efficacy strengthens the impact of social support but does not moderate the effects of economic value or perceived risk. These findings underline the critical role of peer and superior support in driving real usage behavior when physicians feel confident.
Conclusion: This study contributes novel evidence by directly measuring actual use, which is less explored in TAM research. The findings highlight the need to strengthen supportive environments and build physicians’ confidence to boost technology adoption. Future research should test this model across broader healthcare contexts and over time.
Plain Language Summary
Telemedicine can help physicians in Indonesia deliver better care, but using it in daily practice depends on more than just the availability of technology. The authors explored what drives physicians to move from intention to actual use. Clear economic value and strong social support from colleagues or supervisors encourage adoption, while concerns about digital risk can hinder use. Confidence in their ability also helps physicians turn support into real action. These findings suggest that hospitals should focus on providing training, reducing perceived risks, and creating supportive environments to help physicians successfully adopt telemedicine.
Citation: Telehealth and Medicine Today © 2025, 10: 615
DOI: https://doi.org/10.30953/thmt.v10.615
Copyright: © 2025 The Authors. This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0. The authors of this article own the copyright.
Submitted: July 30, 2025; Accepted: October 14, 2025; Published: December 20, 2025.
Corresponding Author: Elika Setiawaty, Email: elikaset06@yahoo.com
Competing interests and funding: No competing interests exist among the authors. The authors declare that they have no financial or non-financial relationships or activities that could have influenced the results or interpretation of this research.
The authors received no financial support for the research, authorship, and/or publication of this article.
The expansion of telemedicine services has continued beyond the COVID-19 pandemic. Yet its routine use remains inconsistent across user groups.1 In the period 2024–2025, the emergence of new telemedicine startups,2 stricter data privacy regulations,3 and growing economic concerns have shaped telemedicine decisions when adopting digital health services.4
Despite technological advances, many physicians remain cautious due to professional risks such as diagnostic limitations, data privacy concerns, and potential legal implications.4,5 Economic considerations also influence physicians’ willingness to adopt telemedicine, as they weigh whether online consultations fairly compensate their time and expertise. Moreover, institutional and peer support plays a critical role in shaping physicians’ confidence and motivation to engage in telemedicine.1,6 These trends highlight the need to examine how social, economic, risk-related, and psychological factors interact to drive physicians’ actual use of telemedicine platforms in daily practice.
While the Jaminan Kesehatan Nasional has been widely applied to explain technology adoption in healthcare,4,7,8 most empirical studies have focused on patients as end-users, leaving the perspective of physicians relatively underexplored.4,7,9,10 Prior research has primarily emphasized perceived usefulness and ease of use as key predictors of acceptance, yet has overlooked how external factors such as social support, perceived risk, and economic value shape physicians’ decisions to integrate telemedicine into their clinical routines.9,11 In addition, although self-efficacy has been investigated among patients, its role in influencing physicians’ confidence to deliver quality remote care remains insufficiently examined.8,12
In Indonesia, the adoption of telemedicine has continued to expand since the COVID-19 pandemic, driven by both government initiatives and private sector innovations. Various telemedicine platforms have emerged to address healthcare access disparities, particularly in remote and underserved regions.13 However, despite increasing availability, the integration of telemedicine into physicians’ daily practice remains inconsistent.13,14 Many physicians still prefer conventional face-to-face consultations due to concerns about diagnostic accuracy, patient trust, and regulatory uncertainties related to medical liability and data protection. In addition, disparities in digital infrastructure and uneven institutional support often hinder physicians’ willingness to deliver care remotely. Financial aspects also come into play, as not all physicians perceive telemedicine consultations as equally rewarding or sustainable compared to traditional practice. These contextual challenges highlight the pressing need to investigate the factors that shape physicians’ readiness and confidence to engage with telemedicine in the Indonesian healthcare system.13,15
This gap is particularly relevant in emerging economies, where healthcare professionals face unique challenges in balancing new digital workflows with conventional medical practice, especially from Indonesian physicians’ evidence.
Indonesia’s healthcare system is characterized by a mixed public–private provision model, with over half of hospitals operated by private entities, reflecting a diverse and complex structure.16,17 The country employs a substantial but unevenly distributed healthcare workforce, which poses challenges to equitable service delivery, especially in rural and remote regions. Indonesia has implemented a national social health insurance scheme (Jaminan Kesehatan Nasional) that covers approximately 73% of the population and aims to enhance financial protection and access to care.16,18 Nevertheless, disparities in healthcare utilization persist due to factors such as differential insurance coverage (including subsidized versus contributory schemes), reimbursement limitations, and variations in healthcare quality across facilities, necessitating ongoing policy attention to optimize the system’s efficiency and equity.16
To address this gap, the authors developed and analyzed an extended TAM framework by incorporating social support, perceived risk, economic value, and self-efficacy to explain physicians’ actual use of telemedicine.4,8,12 The model proposes that social support might encourage physicians’ confidence to use telemedicine, while perceived risk could deter its adoption due to concerns over diagnostic accuracy and legal responsibility.8 Economic value is expected to positively influence physicians’ motivation by highlighting the financial and time efficiency benefits of remote consultations.9,12 Furthermore, the moderating role of self-efficacy in translating these factors into actual behavioral outcomes is evaluated.19 This framework aims to advance the understanding of physicians’ technology adoption behavior by capturing the interplay of contextual and cognitive factors that drive their engagement with telemedicine services.
The proposed model includes six hypotheses (H1–H6), each reflecting a direct or moderated path among the core constructs. H1–H3 examine the direct effects of social support, perceived risk, and economic value on physicians’ actual use of telemedicine.8,12,20–23 Hypotheses H4–H6 specify the moderating role of self-efficacy in these relationships, testing whether physicians’ confidence in their ability to deliver remote care strengthens or weakens the influence of social support, perceived risk, and economic value on their actual use of telemedicine services.19,24,25 All hypothesized relationships are theoretically grounded in extensions of the TAM and social cognitive theory (Figure 1), and are empirically tested using structural equation modeling, with detailed results presented in the following sections.
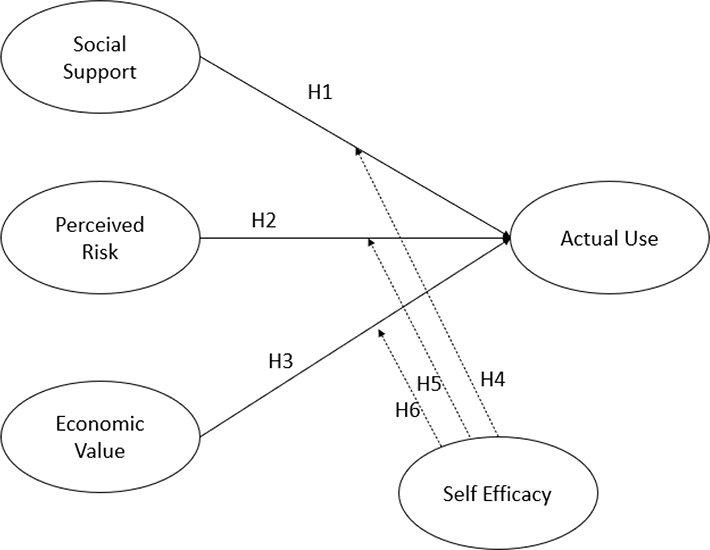
Fig. 1. The proposed research model includes six hypotheses (H1–H6): H1–H3 examine the direct effects of social support, perceived risk, and economic value on physicians’ actual use of telemedicine; H4–H6 assess the moderating role of self-efficacy in these relationships. See text for greater detail.
Methods
Research Design and Sampling Method
This study employed a cross-sectional survey analyzed using Partial Least Squares Structural Equation Modeling (PLS-SEM),26 which is well-suited for modeling complex latent constructs. Data were collected through an online survey distributed via an appropriate platform such as Google Forms to ensure ease of access and wide reach. A stratified sampling method was used to select 300 respondents, with equal representation of age groups: 50% of participants were above the median age, and 50% were below it. Out of the total distributed questionnaires, 244 valid responses were returned and included in the final analysis. Following this, the refined online survey was distributed to 300 physicians using a purposive sampling strategy, resulting in 244 complete and eligible responses from licensed physicians, yielding a valid response rate of 81.3%. Participants included general practitioners and specialists with prior experience in telemedicine, recruited through national medical associations, hospital networks, and a central telemedicine platform.
Measurement
The constructs were adapted from established frameworks such as actual use, perceived risk and economic,27–29 social support12,30,31 and self-efficacy,32,33 ensuring content and convergent validity among constructs and indicators. Therefore, factors like social support, self-efficacy, perceived digital risk, and economic value were measured using five-point Likert scales, while actual use was captured through frequency-based items. The measurement instruments for this study were adapted and contextualized to fit the specific focus of our research model. Five latent constructs were assessed using self-reported items grouped as follows: (1) four items measuring social support, (2) four items assessing perceived risk, (3) four items evaluating economic value, (4) four items measuring actual use of the system, and (5) four items assessing self-efficacy as a moderating variable.
Respondents reported engaging with multiple telemedicine modalities that reflect the evolving digital healthcare landscape in Indonesia. The most frequently cited forms of use included video consultations, which enable real-time interaction and clinical assessment; telephone-based consultations, often utilized for follow-up care or quick medical advice; and chat-based applications, providing asynchronous communication that allows patients to send questions and receive guidance at their convenience. These modalities capture the range of digital practices adopted by physicians and highlight the heterogeneity of telemedicine delivery formats, each with distinct implications for accessibility, efficiency, and perceived clinical value.
Responses were recorded using a five-point Likert scale ranging from 1 (strongly disagree) to 5 (strongly agree). The items were selected and adapted from established measurement scales validated in prior studies to ensure conceptual relevance and reliability within the context of this study. To ensure the instruments were culturally and contextually appropriate, a standardized multi-step adaptation procedure was carried out: initial translation and back-translation were conducted by bilingual experts in social sciences and consumer behavior; pre-testing was performed with a pilot group of 30 respondents to check item clarity, relevance, and local appropriateness; and minor wording revisions were made to enhance comprehension while preserving the conceptual integrity of each construct. This process ensured that the measurement instruments accurately captured the intended dimensions and were suitable for the target population.
Results and Discussion
Respondents’ Profile
A total of 244 physicians participated in the survey, with 44.3% (n = 108) identified as male and 55.7% (n = 136) as female. The majority (76.2%, n = 186) were classified as Millennials (born between 1981 and 1996), while 23.8% (n = 58) were non-Millennials (born before 1981). Regarding professional background, 61.5% (n = 150) were general practitioners and 38.5% (n = 94) were specialists. These distributions indicate a diverse respondent pool in terms of gender, age, and professional role, which strengthens the validity of the study’s conclusions on telemedicine adoption behavior. The detailed demographic characteristics of the respondents are presented in Table 1.
Outer Model Pls-Sem
In PLS-SEM, the measurement model, commonly referred to as the outer model, specifies how latent variables are measured by their observed indicators. Before assessing the structural (inner) model, it is essential to evaluate the reliability and validity of the outer model to ensure that the constructs are measured consistently and accurately.26
Each indicator should have a factor loading (λ) greater than 0.70 to demonstrate that it adequately reflects the associated latent construct. The internal consistency reliability (ICR) for all constructs, assessed through both Cronbach’s alpha and Composite Reliability (CR), exceeded the recommended threshold of 0.70, indicating satisfactory consistency among the indicators. Convergent validity was also supported, as all constructs achieved average variance extracted (AVE) values greater than 0.50, confirming that each construct explains more than half of the variance in its indicators. In addition, discriminant validity was established using the Fornell–Larcker criterion, which showed that the square root of each construct’s AVE was higher than its correlations with other constructs, indicating that the latent variables are distinct and measure separate concepts as intended.26,34 The overall results of the outer model can be seen in Table 2.
Overall, the results of the outer model assessment indicate that all measurement indicators and constructs in this study are statistically acceptable. All factor loadings meet or exceed the recommended thresholds, ICR (CR) values are above 0.70, and the AVE values surpass 0.50 for all constructs. The measurement results demonstrate that the social support construct is robustly measured by four indicators, with factor loadings ranging from 0.841 to 0.921. Specifically, recommendations from seniors or mentors (λ = 0.921) and colleagues (λ = 0.904) emerged as the strongest contributors, while encouragement from family (λ = 0.841) and support from supervisors (λ = 0.879) also showed substantial loadings. The construct achieved an AVE of 0.786, Cronbach’s alpha of 0.909, and a CR of 0.936, indicating that the items consistently and reliably capture the intended dimension of social support.
The self-efficacy constructs likewise demonstrated excellent measurement properties, with all four indicators showing strong factor loadings between 0.903 and 0.920. Items related to physicians’ confidence in operating telemedicine systems, resolving technical problems, making accurate clinical decisions, and performing routine activities all loaded well above the minimum threshold. The AVE for self-efficacy was 0.830, with Cronbach’s alpha and CR values of 0.932 and 0.951, respectively, confirming high internal consistency and convergent validity.
Similarly, perceived digital risk, economic value, and actual use constructs were all statistically supported. Perceived digital risk showed factor loadings ranging from 0.876 to 0.926, with an AVE of 0.793, Cronbach’s alpha of 0.917, and CR of 0.939. Economic value was measured with loadings between 0.855 and 0.940, achieving an AVE of 0.830, alpha of 0.931, and CR of 0.951. Finally, actual use demonstrated factor loadings from 0.829 to 0.885, with an AVE of 0.735, Cronbach’s alpha of 0.880, and CR of 0.917. These results confirm that all constructs fulfill the recommended statistical criteria, providing a solid foundation for the structural model analysis. Table 2 shows the overall results of the outer model PLS-SEM in this study.
The results of the discriminant validity assessment using the Fornell–Larcker criterion (Table 3) indicate that each construct’s square root of AVE (shown on the diagonal) is higher than its correlations with other constructs (off-diagonal values). For example, the square root of AVE for actual use is 0.857, which is greater than its correlations with economic value (0.571), self-efficacy (0.549), and social support (0.559). Similarly, economic value has a square root of AVE of 0.911, exceeding its correlations with actual use (0.571), self-efficacy (0.749), and social support (0.589).
Perceived risk shows a square root of AVE of 0.892, which is substantially higher than its negative correlations with other constructs, such as actual use (–0.136) and economic value (–0.170). Self-efficacy demonstrates strong discriminant validity as well, with a square root of AVE of 0.910 that surpasses its correlations with economic value (0.749), actual use (0.549), and social support (0.656). Social support has a square root of AVE of 0.887, which is greater than its correlations with other constructs. Overall, these results confirm that each construct is empirically distinct from the others, fulfilling the Fornell–Larcker criterion for discriminant validity. This supports the adequacy of the measurement model and strengthens confidence in the structural relationships examined in the subsequent analysis.
Inner Model Pls-Sem
In PLS-SEM, the inner model refers to the structural model that specifies the hypothesized relationships among latent constructs. To ensure its adequacy, the inner model must be evaluated by examining the R-squared values for predictive accuracy and the Variance Inflation Factor (VIF) to detect any multicollinearity issues. Once these assessments meet acceptable standards, hypothesis testing is conducted to determine the significance and strength of the structural paths.35 Table 4 shows the results of VIF in the study.
Therefore, the inner model continues with the R-squared and model assessment analysis. The R-squared value of 0.425 (as shown in Figure 2) indicates that the predictors in the model collectively explain 42.5% of the variance in actual use. The adjusted R-squared of 0.408 confirms that this explanatory power remains substantial even after accounting for the number of predictors in the model. The model fit indices indicate an acceptable fit, with the SRMR value for both the saturated and estimated models at 0.064, which is below the recommended threshold of 0.08. Additionally, the chi-square, d_ULS, d_G, and NFI values support the overall fit of the structural model, with an NFI of 0.855 suggesting a satisfactory level of model–data correspondence.35,36
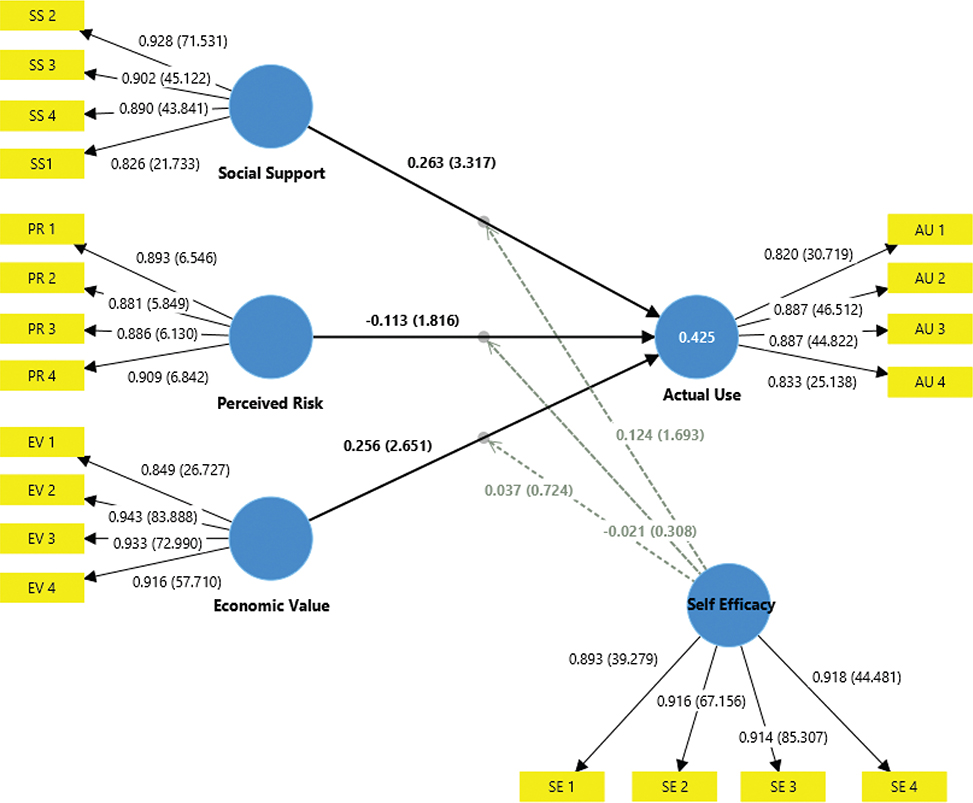
Fig. 2. Structural model of social support, perceived risk, economic value, and self-efficacy to explain physicians’ actual use of telemedicine. AU: actual use; PR: perceived digital risk; SE: self-efficacy; SS: social support.
After ensuring that the measurement model and model fit criteria were satisfactorily met, the structural relationships hypothesized in this study were tested to examine factors influencing physicians’ actual use of telemedicine (as shown in Table 5 and Figure 2). The results show that economic value has a significant positive effect on actual use (β = 0.256, p = 0.004). This indicates that physicians perceive telemedicine as a tool that adds tangible economic benefits, such as reducing operational costs and enabling them to serve more patients efficiently.21,37 The previous studies highlighted that perceived economic and performance advantages are key drivers for technology adoption in healthcare settings.21,37
Perceived digital risk was found to have a significant negative effect on actual use (β = −0.113, p = 0.035), indicating that concerns about legal protection, data security, and potential technical failures continue to act as barriers for physicians when integrating telemedicine into daily practice. This result is consistent with previous studies who emphasized that perceived risks and privacy concerns can dampen physicians’ willingness to rely on new health information technologies.22,38 Despite technological advancements, this persistent risk perception underlines the importance of providing robust legal frameworks and technical support to mitigate these barriers.22,38
Furthermore, social support was the strongest predictor among the direct effects (β = 0.263, p < 0.001), reinforcing the view that professional encouragement from mentors, colleagues, and supervisors significantly motivates physicians to adopt telemedicine.8,12 The previous studies demonstrated that physicians are more likely to adopt telemedicine systems when they perceive strong endorsement and encouragement from senior colleagues and department heads.8 The support from peers and supervisors not only provides practical guidance but also reduces uncertainty and resistance by signaling professional approval of the new system.7,28,39 Hence, social influence within hospitals can positively affect physicians’ attitudes toward using health information technology, as professional networks create a sense of shared norms and collective confidence.39 Such support mechanisms help overcome common barriers like lack of familiarity or perceived complexity by fostering a climate where adopting new tools becomes a professionally expected and supported behavior.29 Taken together, these studies underline that in professionalized environments like hospitals, social and managerial encouragement is a powerful lever for accelerating technology uptake.
However, the moderating effects reveal more nuanced dynamics. The interactions between self-efficacy and both economic value (β = –0.021, p = 0.379) and perceived risk (β = 0.037, p = 0.234) were not statistically significant, indicating that self-efficacy does not strengthen or weaken the effect of these factors on actual use in this context. Interestingly, only the interaction between self-efficacy and social support was significant (β = 0.124, p = 0.045), suggesting that physicians with higher self-efficacy are more responsive to social influence when deciding to adopt telemedicine. In other words, when users feel confident in their ability to use the platform (high self-efficacy), they are more likely to be influenced by social factors such as recommendations or behaviors of important others (social influence) in their decision to actually engage in the use of the healthcare platform.40 Self-efficacy enhances the effect of social influence because confident users are better able to translate social pressure or encouragement into actual use behavior. Overall, these findings highlight the fact that while individual confidence is crucial, its ability to moderate the impact of contextual factors may vary, which opens avenues for future studies to explore these dynamics in different healthcare contexts and professional cultures.40
Conclusion
This study involved 244 physicians in Indonesia and extends the TAM by testing self-efficacy as a moderating factor on actual use of technology. Unlike most TAM-based studies that focus only on intention to use, this research directly investigates actual use, which provides stronger and more practical evidence of real adoption behavior (a perspective still rarely studied in depth, especially in the context of healthcare professionals in developing countries).
The results also imply that clear economic benefits and strong peer or superior support can encourage physicians to actually use technology, whereas high perceived risk discourages it. Furthermore, self-efficacy strengthens the relationship between social support and actual use but does not significantly moderate the effects of economic value or perceived risk. This highlights the fact that physicians’ confidence plays a more important role in leveraging social support than in influencing economic or risk perceptions.
These findings support prior evidence that peer and superior support can play a critical role in driving technology adoption in healthcare organizations. Beyond these results, future research should explore additional factors that may influence technology adaptation, such as institutional support, organizational culture, or sociodemographic characteristics. Considering these broader dimensions will enrich the understanding of how healthcare professionals adopt telemedicine in diverse contexts.
Limitations
This study has some limitations. First, it focused only on physicians in Indonesia, which might limit the generalizability of the findings to other healthcare professionals or different healthcare systems. Second, this study used a cross-sectional design, so it does not capture changes in behavior or self-efficacy over time.
Despite these limitations, the novelty of this research lies in its direct focus on actual use rather than intention and its extension of the TAM by integrating self-efficacy as a moderator providing fresh insights into how individual confidence interacts with social factors to shape real usage behavior.
Going Forward
Future research should expand on these findings by including other potential moderating or mediating variables such as organizational culture, trust in digital systems, or the quality of training provided. Longitudinal or mixed-method designs could enrich understanding of how self-efficacy develops and how interventions can sustain or enhance it.
Finally, studies involving other healthcare professionals or broader regional contexts would help validate and strengthen the generalizability of this study’s conclusions on actual technology use in healthcare practice. Moreover, this study did not examine other relevant factors, such as institutional support (e.g. organizational policies, infrastructure availability) or physicians’ sociodemographic characteristics (e.g. age, gender, digital literacy), which may also shape telemedicine adoption. Future research should address these aspects, incorporate longitudinal or mixed-method designs, and expand the sample to broader regional and professional contexts.
Contributors
Conceptualization: ES, HH, RN, and LN; Methodology: ES; Software: ES; Validation: ES; Formal Analysis: ES; Investigation: ES; Resources: ES; Data Curation: ES; Writing Original Draft Preparation: ES, HH, RN, and LN; Writing Review and Editing: ES; Visualization: ES; All authors, ES, HH, RN, and LN, have read and agreed to the published version of the manuscript.
Data Availability Statement (DAS), Data Sharing, Reproducibility, and Data Repositories
AI-assisted tools, including language refinement and grammar correction software (Grammerly, Quillbot), were used for improving linguistic clarity and formatting of the manuscript. No part of the analytical work, dataset processing, or result generation was performed using AI-generated content.
Application of AI-Generated Text or Related Technology
None used.
Acknowledgments
The authors thank the Department of Information Technology, Annamalai University, and the Department of Computer Science and Engineering, SRM Institute of Science and Technology (Trichy Campus), for providing computational resources and academic guidance. The authors also acknowledge open-access datasets such as NIH ChestX-ray14, COVID-CXR, Montgomery, and Shenzhen repositories for enabling this study.
References
- Tabaeeian RA, Hajrahimi B, Khoshfetrat A. A systematic review of telemedicine systems use barriers: primary health care providers’ perspective. J Sci Technol Policy Manag. 2024;15:610–35.
- Chakraborty I, Ilavarasan PV, Edirippulige S. What helps age-tech startups scale-up? Some insights. International Entrepreneurship and Management Journal. 2025 Dec 1;21(1): 1–32. https://doi.org/10.1007/s11365-025-01081-w
- Balogun AY. Strengthening compliance with data privacy regulations in U.S. healthcare cybersecurity. Asian J Res Comput Sci. 2025 Jan 18;18(1):154–73. https://doi.org/10.9734/ajrcos/2025/v18i1555
- Sengupta A, Sarkar S, Bhattacherjee A. The relationship between telemedicine tools and physician satisfaction, quality of care, and patient visits during the COVID-19 pandemic. Int J Med Inform. 2024 Oct 1;190 (106151). https://doi.org/10.1016/j.ijmedinf.2024.106151
- Orsayeva R, Berestova A, Krasilnikova V, Timoshin A. Telemedicine during COVID- 19: features of legal regulation in the field of administrative liability for errors committed by medical institutions. Vol. 15: 1–16, Egyptian Journal of Forensic Sciences. Springer Science and Business Media Deutschland GmbH; 2025. https://doi.org/10.1186/s41935-025-00443-3
- Susanti R, Syarkani Y, Ratna D, Handayani S, Waluyo I. Impact of telemedicine on hospital financial models. Jurnal Multidisiplin Indonesia. 2025. Feb 4;2:93–109.
- Lee AT, Ramasamy RK, Subbarao A. Understanding psychosocial barriers to healthcare technology adoption: a review of TAM technology acceptance model and unified theory of acceptance and use of technology and UTAUT frameworks. Healthcare (Switzerland). 2025;13:1–35. https://doi.org/10.3390/healthcare13030250
- Bîlbîie A, Puiu AI, Mihăilă V, Burcea M. Investigating physicians’ adoption of telemedicine in romania using technology acceptance model (TAM). Healthcare (Switzerland). 2024 Aug 1;12(15).
- Senthilrajah T, Ahangama S. The Sri Lankan enigma: demystifying public healthcare information systems acceptance. BMC Health Serv Res. 2025 Dec 1;25(1). https://doi.org/10.1186/s12913-024-12173-8
- Wang Z, Wang Y, Zeng Y, Su J, Li Z. An investigation into the acceptance of intelligent care systems: an extended technology acceptance model (TAM). Sci Rep. 2025 Dec 1;15(1). https://doi.org/10.1038/s41598-025-02746-w
- Hussain A, Zhiqiang M, Li M, Jameel A, Kanwel S, Ahmad S, et al. The mediating effects of perceived usefulness and perceived ease of use on nurses’ intentions to adopt advanced technology. BMC Nurs. 2025 Dec 1;24(1). https://doi.org/10.1186/s12912-024-02648-8
- Tan SH, Wong CK, Yap YY, Tan SK. Factors influencing telemedicine adoption among physicians in the Malaysian healthcare system: a revisit. Digit Health. 2024 Jan 1;10: 1–26.https://doi.org/10.1177/20552076241257050
- Mutiah F, Sibuea H, Candra M. Telemedicine regulation in Indonesia: legal frameworks, challenges, and future directions. Jurnal Multidisiplin Indonesia. 2025;4(4):242–51. https://doi.org/10.58344/jmi.v4i4.2267
- Sugandi MS, Mulyana D, Elita RFM, Rusmana A. Lessons learned from the pandemic in indonesia: enhancing doctor-patient medical communication to improve diagnostic certainty in telemedicine. J Law Sustain Dev. 2023 Nov 14;11(11):e2076. https://doi.org/10.55908/sdgs.v11i11.2076
- Amir AS. User experience in accessing and utilizing digital health systems: a phenomenological study exploring the lived experiences of medical practitioners and patients on telemedicine platforms in Indonesia. J Digit Health Innov Med Technol. 2025;1: 29–37.
- Cheng Q, Fattah RA, Susilo D, Satrya A, Haemmerli M, Kosen S, et al. Determinants of healthcare utilization under the Indonesian national health insurance system—a cross-sectional study. BMC Health Serv Res. 2025 Dec 1;25(1). https://doi.org/10.1186/s12913-024-11951-8
- Mahendradhata Y, Andayani NLPE, Hasri ET, Arifi MD, Siahaan RGM, Solikha DA, et al. The capacity of the Indonesian healthcare system to respond to COVID-19. Front Public Health. 2021 Jul 7;9: 1–9. https://doi.org/10.3389/fpubh.2021.649819
- Husin L, Idris F, Liberty IA. The role of BPJS Kesehatan in improving health access equity in Indonesia. Public Health Policy Admin J. 2025 [cited 2025 Jul 20]. Available from: https://publichealthadminjournal.org/index.php/publichealthadmin
- Tian Y, Chan TJ. Predictors of mobile payment use applications from the extended technology acceptance model: does self-efficacy and trust matter? Sage Open. 2024 Oct 1;14(4):1–17. https://doi.org/10.1177/21582440241292525
- Chaudhary P, Payal, Nain P, Pooja, Rana P, Verma P, et al. Perceived risk of infection, ethical challenges and motivational factors among frontline nurses in Covid-19 pandemic: prerequisites and lessons for future pandemic. BMC Nurs. 2024 Dec 1;23(1). https://doi.org/10.1186/s12912-023-01653-7
- Hodson N, Powell BJ, Nilsen P, Beidas RS. How can a behavioral economics lens contribute to implementation science? Implement Sci. 2024 Dec 1;19(1). https://doi.org/10.1186/s13012-024-01362-y
- Chen SY, Kuo HY, Chang SH. Perceptions of ChatGPT in healthcare: usefulness, trust, and risk. Front Public Health. 2024;12. https://doi.org/10.3389/fpubh.2024.1457131
- Lerch SP, Hänggi R, Bussmann Y, Lörwald A. A model of contributors to a trusting patient-physician relationship: a critical review using a systematic search strategy. BMC Prim Care. 2024 Dec 1;25(1). https://doi.org/10.1186/s12875-024-02435-z
- Kim BJ, Kim MJ. The influence of work overload on cybersecurity behavior: a moderated mediation model of psychological contract breach, burnout, and self-efficacy in AI learning such as ChatGPT. Technol Soc. 2024 Jun 1;77. https://doi.org/10.1016/j.techsoc.2024.102543
- Yang P, Xu R, Le Y. Factors influencing sports performance: a multi-dimensional analysis of coaching quality, athlete well-being, training intensity, and nutrition with self-efficacy mediation and cultural values moderation. Heliyon. 2024 Sep 15;10(17):1–13. https://doi.org/10.1016/j.heliyon.2024.e36646
- Sarstedt M, Ringle CM, Hair JF. Partial least squares structural equation modeling. In: C. Homburg et al. (eds), Handbook of market research. Springer Nature Switzerland AG 2021. p. 1–47. https://doi.org/10.1007/978-3-319-06152-8_15-2
- Shaarani I, Jounblat M, Jounblat H, Ghanem A, Mansour R, Taleb R. Developing and validating a tool to assess telemedicine acceptance among physicians during pandemic using a technology acceptance model. Telemed e-Health. 2023 Jun 1;29(6):903–11. https://doi.org/10.1089/tmj.2022.0348
- Stoumpos AI, Kitsios F, Talias MA. Digital transformation in healthcare: technology acceptance and its applications. Int J Environ Res Public Health. 2023 Feb 1;20(4): 1–44.
- Alsahli S, Hor SY, Lam MK. Physicians’ acceptance and adoption of mobile health applications during the COVID-19 pandemic in Saudi Arabia: extending the unified theory of acceptance and use of technology model. Health Inf Manag J. 2024;54(3):255–67. https://doi.org/10.1177/18333583241300534
- de Blanes Sebastián MG, Antonovica A, Sarmiento Guede JR. What are the leading factors for using Spanish peer-to-peer mobile payment platform Bizum? The applied analysis of the UTAUT2 model. Technol Forecast Soc Change. 2023 Feb 1;187:1–16. https://doi.org/10.1016/j.techfore.2022.122235
- Meng D, Guo Z. Influence of doctor-patient trust on the adoption of mobile medical applications during the epidemic: a UTAUT-based analysis. Front Public Health. 2024;12. https://doi.org/10.3389/fpubh.2024.1414125
- Ram S, Sheth JN. Consumer resistance to innovations: the marketing problem and its solutions. J Consum Market. 1989;6(2):5. https://doi.org/10.1108/EUM0000000002542
- Kaur P, Dhir A, Singh N, Sahu G, Almotairi M. An innovation resistance theory perspective on mobile payment solutions. J Retail Consum Serv. 2020 Jul 1;55:1–16. https://doi.org/10.1016/j.jretconser.2020.102059
- Henseler J, Ringle CM, Sarstedt M. A new criterion for assessing discriminant validity in variance-based structural equation modeling. J Acad Mark Sci. 2015 Jan 1;43(1):115–35. https://doi.org/10.1007/s11747-014-0403-8
- Ringle CM, Sarstedt M, Sinkovics N, Sinkovics RR. A perspective on using partial least squares structural equation modelling in data articles. Data Brief. 2023 Jun 1;48:1–21. https://doi.org/10.1016/j.dib.2023.109074
- Hair JF, Risher JJ, Sarstedt M, Ringle CM. When to use and how to report the results of PLS-SEM. Eur Bus Rev. 2019;34:2–24. https://doi.org/10.1016/j.dib.2023.109074
- Dann D, Teubner T, Adam MTP, Weinhardt C. Where the host is part of the deal: social and economic value in the platform economy. Electron Commer Res Appl. 2020 Mar 1;40: 100923. https://doi.org/10.1016/j.elerap.2019.100923
- Marafon DL, Basso K, Espartel LB, de Barcellos MD, Rech E. Perceived risk and intention to use internet banking: the effects of self-confidence and risk acceptance. Int J Bank Market. 2018;36(2):277–89. https://doi.org/10.1108/IJBM-11-2016-0166
- Li W, Guo J, Liu W, Tu J, Tang Q. Effect of older adults willingness on telemedicine usage: an integrated approach based on technology acceptance and decomposed theory of planned behavior model. BMC Geriatr. 2024 Dec 1;24(1):765. https://doi.org/10.1186/s12877-024-05361-y
- Bashir L, Madhavaiah C. Trust, social influence, self-efficacy, perceived risk and internet banking acceptance: an extension of technology acceptance model in Indian context. Metamorphosis. 2015;14(1):25–38. https://doi.org/10.1177/0972622520150105
Copyright Ownership: This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0. The authors of this article own the copyright.