NARRATIVE/SYSTEMATIC REVIEWS/META-ANALYSIS
Telemedicine Growth: A Comparative Study of Global and Indian Scenarios
S. Hemalatha PhD (CSE)1  ; Kiran Mayee Adavala PhD (CSE)2
; Kiran Mayee Adavala PhD (CSE)2  ; Pullela SVVSR Kumar PhD (CSE)3
; Pullela SVVSR Kumar PhD (CSE)3  ; N. Muthuvairavan Pillai PhD4
; N. Muthuvairavan Pillai PhD4  ; S. Muruganandam PhD (CSE)5
; S. Muruganandam PhD (CSE)5  ; G. Krishna Mohan PhD (CSE)6
; G. Krishna Mohan PhD (CSE)6 
1Department of Computer Science and Business Systems, Panimalar Engineering College , Chennai, Tamil Nadu, India; 2Associate Professor, CSE(AIML), Kakatiya Institute of Technology and Science, Warangal, India; 3Professor, Department of Computer Science and Engineering, Aditya University, Surampalem, Andhra Pradesh, India; 4Department of Computer Science and Business Systems, RMD Engineering College, Chennai, India; 5Associate Professor, Department of Computer Science and Business Systems, Panimalar Engineering College, Chennai, India; 6Professor, Department of CSE, Koneru Lakshmaiah Education Foundation, Guntur, India
Keywords: Digital health, ehealth, global health, India, remote consultation, telemedicine, telehealth adoption
Abstract
Telemedicine is remote healthcare as a result of expansion of digital technologies worldwide. This was especially true after the COVID-19 pandemic. The practical use of telemedicine varies among countries depending on the views and acceptance by the population. Here, the authors focus on exploring telemedicine growth in the global and Indian scenarios with secondary data collected from the World Health Organization, McKinsey, Statista, government medical reports, and peer-reviewed literature. The authors present an analysis of its market growth, enabling technologies, telemedicine regulatory framework, and adoption challenges. Globally, the telemedicine market exceeded 22,545 INR in 2024 in response to the latest application of technology in telemedicine (e.g. 5G, artificial intelligence, and integrated health policies). In India, telemedicine is growing with respect to the compound annual growth rate of 31%, which is supported by government initiatives such as eSanjeevani and the National Digital Health Mission for rural connectivity gaps and infrastructure limitations. This article highlights an assessment of the Indian and global scenarios with the support of policy maturity and technology adoption. Finally, it highlights the unique opportunities to strengthen rural healthcare systems. The authors conclude that robust telemedicine policies and stronger public and private collaboration will accelerate and promote the success of telehealth delivery.
Citation: Telehealth and Medicine Today © 2026, 11: 620 - https://doi.org/10.30953/thmt.v11.620
DOI: https://doi.org/10.30953/thmt.v11.620
Copyright: © 2026 The Authors. This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See http://creativecommons.org/licenses/by-nc/4.0. The authors of this article own the copyright.
Submitted: August 9, 2025; Accepted: January 2, 2026; Published: March 31, 2026
Corresponding Author: S. Muruganandam, Email: smuruganandam.csbs@panimalar.ac.in
Note: 50 Indian Rupee (INR), ≈ $.01, ≈ .009 €.
Competing interests and funding: There is no conflict of interest among the authors for publication of this article.
There is no Internal or external funding received for the research carried out and the publication.
Telemedicine is a healthcare delivery model that enables real-time interaction between healthcare professionals and patients through digital communication technologies.1 Telemedicine helps to overcome limitations of distance, cost, and accessibility. The concept was first explored in the United States during the 1950s, when radiographic images were transmitted over telephone lines.2,3 With the advent of the internet, satellite communication, and mobile technologies telemedicine has expanded worldwide. Despite this progress, initial adoption was limited due to infrastructure challenges and social resistance.4
People were homebound during the COVID-19 pandemic. They adapted to telemedicine for consultation on health-related issues worldwide.5 Telemedicine supported COVID-19 restricted movement of social distancing and virtual care as an alternative solution for these patients. Many organizations and healthcare departments were supported to develop and support telemedicine for remote patient services.6,7 Later, people gradually began using hybrid telemedicine consultant and in-person consultations.
In India, significant growth of telemedicine has occurred over the past five years, driven by initiatives such as the Ayushman Bharat Digital Mission (ABDM), eSanjeevani, and the release of the 2020 Telemedicine Practice Guidelines (TMGs). The private sector also introduced mobile teleconsultation services, particularly targeting urban populations.8 However, widespread adoption remains constrained by challenges such as digital literacy gaps, regulatory ambiguities, limited rural penetration, and infrastructure deficits. Low- and middle-income countries, including India, continue to explore solutions to promote telemedicine adoption and share best practices internationally.9
Unlike prior research that treats the development of global and Indian telemedicine separately. This article presents the unique contribution by systematically comparing these trajectories. In addition, the authors analyze and highlight different technological uses, telehealth policy, and healthcare access support in global and Indian health strategies. Finally, the comparative significance reveals opportunities to enhance rural healthcare access and telemedicine growth. The article is organized as follows: Section 2 examines the literature on global and Indian telemedicine, identifying research gaps and theoretical perspectives. Section 3 details the research methodology. Section 4 explores global telemedicine trends and challenges. Section 5 reviews India’s telemedicine progress. In Section 6 a comparative analysis is discussed. Section 6 reviews, while the challenges are discussed in Section 7. Conclusions and future enhancements are discussed in Section 8 and Section 9 9 suggests future research directions.
Literature Review
The pivotal role of developing telemedicine worldwide10 supports the innovation of Indian telemedicine technology.
This literature review elaborates on the telemedicine environment in India and globally by focusing on advancements in policies, collaboration of private and public platforms, platform adaptation, and challenges in the integration of telehealth.
Global Landscape of Telemedicine
Globally, telehealth has become an essential component of healthcare delivery,11 gaining wide acceptance during the COVID-19 pandemic. In high-income countries such as the United States, Canada, and across Europe, remote consultations expanded rapidly.12 A McKinsey report (2022)13 found that U.S. telehealth utilization stabilized at levels nearly 38 times higher than before the pandemic.14 Similarly, other countries, including Sweden, Germany, and Australia, integrated telemedicine into national electronic health record programs to improve chronic disease management.15 A comprehensive review of telemedicine efficiency is offered for multiple chronic disease management, health behavior, and clinical care.16
In addition, WHO released evidence that demonstrates high patient satisfaction, improved clinical outcomes, and reductions in missed appointments.17 Even though the advanced technologies (e.g. artificial intelligence [AI], wearable devices, and 5G connectivity) enhance diagnostic and triage capabilities,18 challenges in telehealth persist for data privacy, physician licensing, and reimbursement models. Each contributes to uncertainty over telemedicine’s long-term sustainability among nations of the Organisation for Economic Co-operation and Development.19 Importantly, research remains skewed toward high-income countries, with limited insights from low- and middle-income contexts.20
Telemedicine in India
India’s telemedicine development, while influenced by international trends, is largely shaped by policy initiatives and context-sensitive adaptations. In March 2020, the Ministry of Health and Family Welfare (MoHFW) introduced the TMGs, establishing a formal regulatory structure for remote healthcare consultations across the country.21 Following this, the government launched the eSanjeevani platform, which by 2024 supported over 120 million consultations—primarily benefiting rural and smaller urban populations.22
Meanwhile, private sector companies including Practo, 1 mg, Apollo Telehealth (leading Indian digital health platforms offering online doctor consultations, pharmacy, and diagnostics, with Practo focusing on doctor discovery/appointments) and Tata Health have expanded telemedicine services notably in urban and semi-urban areas.23 However, in the rural regions, they are limited in the use of guidelines due to the lack of proper internet connectivity and literacy in digital knowledge.24 Obstacles in the healthcare framework in India, especially in East India (Figure 1) (e.g. Uttar Pradesh, Bihar, and Jharkhand), include data privacy concerns, linguistic diversity, digital literacy disparities, and uneven infrastructure distribution, continue to hinder telemedicine.25,26
Fig. 1. East India (Uttar Pradesh, Bihar, and Jharkhand).
Key Frameworks and Models
A well-established framework is required to implement and expand telemedicine. In 2019 digital health was classified by the WHO into four domains—client, healthcare providers, healthcare systems, and data services—for their digital health strategy.27 This core domain framework was promoted for telemedicine by different regions of sub-Saharan Africa,28 Latin America,29 and sub-Saharan Africa.30 Even in India, the National Digital Health Mission (NDHM) adapted the WHO strategy to advance initiatives such as unique health identifiers, including ABHA, EHRs, and a federated data system designed across various healthcare providers.31
In the United States, the long-term sustainability of telehealth programs was evaluated32 using the effectiveness, adoption, implementation, and maintenance model, and cross-border interoperability among European Union (EU) member states.33 This enabled the European eHealth Digital Service Infrastructure.
Comparative Analysis: Global Versus Indian Scenario
The global and the India telemedicine market34,35 comparative overview36 is outlined in Table 1. On a global scale, telemedicine is valued between $250 and $300 billion. With the support of AI, networks, and the latest insurance models, India’s telemedicine growth is largely supported by government-led initiatives such as eSanjeevani and the rapid expansion of mobile internet access, which has resulted in telemedicine achieving approximately 700 million INR.
| Dimension | Global scenario | Indian scenario |
| Market Size (2024 est.) | $250 to 300 billion 213 to 256 billion € |
INR 5,500 crore* |
| Key enablers | AI, 5G, EHRs, Insurance reimbursement | Government schemes (eSanjeevani), mobile penetration |
| Adoption drivers | Aging population, COVID-19, insurance incentives | Pandemic necessity, government digital health push |
| Barriers | Licensing, reimbursement models, privacy laws | Infrastructure gaps, language diversity, digital illiteracy |
| Popular specialties | Psychiatry, cardiology, endocrinology | General medicine, dermatology, mental health |
| Integration with national ID | Yes (e.g., NHS number in UK, SSN in the U.S.). | Yes (ABHA Health ID under NDHM) |
| Challenges | Interoperability and sustainability post-pandemic | Rural outreach, physician training, data protection |
| Future focus | AI, remote monitoring, predictive care | mHealth, multilingual platforms, rural IoT infrastructure |
| *crore: a unit in the Indian numbering system meaning ten million; 5G: fifth-generation technology; ABHA: Ayushman Bharat Health Account; AI: artificial intelligence; EHRs: electronic health records; ID: identification; IoT: Internet of Things; NDHM: National Digital Health Mission in India; NHS: National Health Service (UK); SSN: social security number (U.S.). | ||
Aging populations and insurance incentives are influencing international telemedicine growth. In India, the progress is mainly policy driven, which was accelerated during the COVID-19 epidemic. But there are challenges for the Indian and global market, where the complexities in licensing are a major obstacle. After the pandemic, long-term sustainable telemedicines were included in the data security and AI-powered healthcare models, which support healthcare innovation and services.
Given that high-income countries benefited by using the technological infrastructure, well established framework, and insurance coverage, in India telemedicine continues to grow with the support of government initiative to create awareness about telemedicine in rural and urban peoples.
The literature demonstrates that while global telemedicine research emphasizes technology readiness, reimbursement models, and regulatory harmonization, Indian studies dominant barriers, highlighting digital literacy, infrastructural inequities, and rural access as. Despite their richness in the literature, few studies directly compare these trajectories. This lack of comparative analysis obscures opportunities to translate global lessons into context-specific strategies for India. Addressing this gap, presenting studies systematically is in contrast to global and Indian telemedicine developments, offering insights into shared challenges, divergent priorities, and opportunities for cross-learning.
Methodology
This section investigates the development and expansion of telemedicine in India using global research with qualitative and quantitative analysis from the peer-reviewed publications and institutional reports.37 This methodology used transparency, productibility, and analysis to ensure that the findings accurately move telemedicine toward adaptation and integration.
Collected Data Sources
The primary data for this article were taken from the combination of global and national repositories and health reports from official and academic databases. Global data were obtained from the WHO,38 digital health reports, and telehealth adoption surveys conducted between 2020 and 2023 by McKinsey & Company.13 Apart from that, market insights and regional use statistics are collected via Statista to provide a comparative understanding of global telemedicine trends.39
Indian telemedicine-specific data were gathered from authorized sources (e.g. National Institution for Transforming India Aayog,40 as well as from MoHFW.41 Data from health-related initiatives were taken from the eSanjeevani platform and the NDHM.42 PubMed, Scopus, and the Web of Science databases were used to collect scholarly literature sources that specifically focus on peer-reviewed scientific research articles, clinical results outcome studies, and policy information analyses published between 2019 and 2025. The reason for this time frame was to capture the telemedicine evolution of pre-pandemic and post-pandemic developments.
Data Collection Method
The Preferred Reporting Items for Systematic Reviews and Meta-Analyses43 guidelines supported undertaking the systematic literature review to certify a transparent research process. Across the selected database, this strategy was applied using the telemedicine-related keywords (e.g. telemedicine, teleconsultation, digital health, Indian and global health systems and eHealth adoption, and health insurance).44
The database inclusion criteria consisted of articles published in peer-reviewed journals, white papers, reports, and telemarket analyses between 2019 and 2025. The focus was on telemedicine adoption, digital framework for health, practices of telemedicine in India and globally. In addition, empirical data, health policies, quantitative indicators using the telehealth growth, investment inflows, and patient feedback measures were also considered. Exclusion criteria included non-peer reviewed journal materials, conference abstracts, editorial opinions, as well the lack of empirical data. Data not related to the telemedicine were also considered for exclusion. From this inclusion and exclusion process, 428 records were initially collected from the database. After removing duplicates of 72 records, 365 articles were screened for relevance, with 112 full text papers assessed for the eligibility. Based on the inclusion and exclusion criteria, 99 articles were compromised qualitatively and quantitatively, including government policies, annual health reports, and market dashboards. Thus the total number reviewed was 99.
Applied Analytical Framework
The analytical framework to access telemedicine included descriptive and statistical evaluation. The metrics included mean values, growth percentages, compound annual growth rate (CAGR), and percentage change to evaluate telemedicine adoption rates and market expansion patterns45 for quantitative analyses. Threephases of data pre-pandemic (2019), pandemic (2020 to 2021), and post-pandemic (2022 to 2024)46 to capture the telemedicine growth. The SWOT (strengths, weaknesses, opportunities, and threats) and PESTLE (political, economic, social, technological, legal, and environmental) frameworks47 were employed for qualitative strategic analyses. Finally, the visualization included the charts and tables that illustrate the Indian and global telemedicine eco systems.
Global Telemedicine Growth
Evolution and Timeline
Global telemedicine has grown rapidly from the teleconsultation service to modern healthcare services for rapid medical consultation. Between 1990 and 2010, telemedicine primarily provided limited video consultation services to rural populations with the support of limited video conferencing technologies.48 However, this development was slow due to the limitation of technological usage and environment uncertainty.
The COVID-19 pandemic (2020 to 2022) marked a major turning point. Lockdowns, social distancing, and overwhelmed healthcare facilities combined to create urgent demand for virtual care alternatives, resulting in an exponential increase in telehealth use worldwide.
According to telemedicine research,49 during the first six months of the epidemic the telemedicine consultation reached 50-fold in global countries such as the U.S. with similar rates in Europe and part of Asia. Post-pandemic, the telemedicine model has stabilized into a hybrid care system, which combines in-person and virtual consultations. In parallel the telehealth market size gets expanded from $50 billion in 2019 and crossed $250 billion by the year 2024 end. This impact reached a CAGR of over 25%, as reported by Nkurunziza et al.50
Regional Growth Trends
The United States continues to be the global leader in telemedicine innovation and adoption. During the COVID-19 epidemic the U.S. government combined the temporary expansion of Medicare coverage for telehealth with insurer reimbursement models. The telehealth market was projected to exceed $120 billion by 2025.51
The EU funding under the EU4Health program52 and patient data privacy is maintained under the General Data Protection Regulation (GDPR). Nations such as Germany and Netherlands have introduced legalized digital prescriptions and reimbursed teleconsultations with public insurance systems.53
China integrates the AI-powered diagnostic tools for digitizing the telehealth system, tele pharmacy and triage system.54 The modern invented platform such as the Ping a Good Doctor supported over 400 million registered users and scale the digital adoption.55
African countries introduced the Short Message Service (SMS)-based teleconsultation with low bandwidth apps to support the infrastructure.56 eHealth strategies are focused on primary care57 in Rwanda and Kenya according to WHO, 2023.
Key Enablers of Growth
The technological, regulatory and economic factors are the accelerated global telemedicine uptake factors with the aid of technological infrastructure, policy and regulation, insurance integration. The 5G networks, cloud computing and Internet of Things (IoT) are the technological infrastructure of telemedicine. The AI/ML (machine learning)-used algorithm provides support for this technological infrastructure to enhance the accuracy, radiology, dermatology and mental health screening.1 Health Insurance Portability and Accountability Act (HIPAA) in the U.S. and GDPR in the EU have clarified legal frameworks for policy and regulation in telemedicine operation with the support of data security and cross-border services.58 Integrating telehealth into reimbursement models supports public and private insurers. For instance, the U.S. has expanded the coverage by the Centers for Medicare & Medicaid Services to more than 80 telehealth services.59
Global Challenges and Barriers
The digital divide, data privacy, cyber security, licencing, and cross border regulation are the major global challenges and barriers to telemedicine. The International Telecommunication Union estimates that over 2.7 billion people worldwide were still offline as on 2023.60 Digital divide supports a reliable internet, smart mobile devices, and overcoming the digital literacy in low-income countries and rural areas. Digital health information is sensitive, requiring data privacy and cyber security protection to overcome a data breach, surveillance, and ethical usage. High profile hospital systems are highlighted in vulnerabilities in current medical platforms.61 A lack of harmonized telemedicine standards across countries impedes international collaboration and patient mobility in virtual care. Regulatory heterogeneity also affects the scalability of global telemedicine platforms.62 The global telemedicine sector has demonstrated impressive growth in scale, innovation, and policy integration, yet it remains challenged by infrastructural and regulatory limitations. The next phase of global digital health will likely focus on standardization, equitable access, and personalized AI-integrated virtual care ecosystems.
Indian Telemedicine Growth
This section discusses telemedicine growth initiatives taken by the Indian government to promote telemedicine in India. The discussion includes Indian government initiatives, market trends, private sector growth, digital divine, and the role of telemedicine in the COVID-19 pandemic.
Indian Government-Led Initiatives
The Indian government63 has played a major role in promoting the telemedicine through the policy forming and nationwide digital health platform initiatives. Three leading initiatives are eSanjeevani, the ABDM and the National Digital Health Mission (MDHM). eSanjeevani was launched by the MoHFW as India’s first national telemedicine service, which operates in eSanjeevani outpatient department (doctor-to-patient) and eSanjeevani Ayushman Bharat—Health and Wellness Centres (AB-HWC) (doctor-to-doctor). This scheme supported 120 million consultations, as the outcome of the production of the world’s largest digital health platforms (MoHFW, 2024).64
Under ABDM, a unique Ayushman Bharat Health Account (ABHA) is issued to every individual, linking their EHRs to a federated data architecture.65 The mission also promotes interoperability between telemedicine providers, hospitals, and pharmacies. The NDHM serves as the digital foundation for India’s healthcare ecosystem, emphasizing data privacy, electronic prescriptions, teleconsultation interoperability, and the standardization of health information technology.66 These initiatives align with the WHO’s digital health framework’s, aim to provide equitable, accountable, and secure access to virtual healthcare services.
Market Trends and Private Sector Growth
In India, telemedicine experienced rapid expansion, when India was granted formal legal recognition for remote consultation through the TMG, which was introduced in India in March 2020.67 A recent study by Bagga et al.68 predicted that the telemedicine market is projected to grow at a CAGR of 31% between 2020 and 2025, the medical market sector expected a market valuation INR 5,857 crore (about USD 700 million).69 The key market private players including Practo,70 Tata Health,71 Apollo Telehealth.72 Practo offer e-prescription, virtual consultation, and home diagnostics across 100+ Indian cities. Tata Health operates a hybrid care model in Tata hospitals. Apollo Telehealth services provide healthcare to over 40,000 patients daily with corporate and government partnership.
The Urban-Rural Divide
Telemedicine penetration in rural areas is less compared with the urban areas in India due to an urban-rural disparity.24 High concentrations of housing and infrastructure in urban areas facilitate higher internet penetration (> 70%) as a result of greater awareness and digital literacy, as well as better access to smartphones, which combine to adopt faster uptake.24
Conversely, in rural regions more that 60% of Indians still face issues of poor broad band coverage, low digital awareness, and a lack of trained telehealth mediators.73 The internet and Mobile Association of India (IAMAI, 2023) report that only 24% of rural households have stable internet connectivity, comparing to 60% in urban areas.74 The comparison reveals that urban residents can get connectivity with primary health centers or community health workers to access telehealth consultations.75
Telemedicine’s Role During the COVID-19 Pandemic
Telemedicine use accelerated in India during the national lockdown between the 2020 and 2021 when physical access to clinics and hospitals was limited and telemedicine became the primary mode of health consultation.76 The Indian Council of Medical Research (ICMR, 2022) authorized telemedicine for more than 65% of outpatients during the COVID waves.77 Especially, eSanjeevani AB-HWC64 enables real-time discussions with specialists. Private apps such as Practo70 reported a 10x growth in online consultations. Mental health services saw a huge demand from Tier 2 and Tier 3 cities.78 During this period, telemedicine scalability in India incorporated the public health system into long-term integration.
Challenges and Structural Barriers
Telemedicine ecosystem has made commendable progress in India; however, it continues to face the multiple systematic and infrastructural challenges (e.g., digital divide, limited internet bandwidth and electricity supply, smart phone use).79 First, there is a significant need for multilingual telemedicine platforms due to language and literacy barriers.80 In India there are more than 22 official languages and numerous dialects. The next challenge in India is digital literacy among older adults and lower economic groups. Although the regulatory and reimbursement issues81 provide the telemedicine legal framework, there exist challenges in data storage, misdiagnosis, insurance coverage, and universal billing code system. Finally, efforts must be undertaken to facilitate rural integration, technology usage, and other factors needed to sustain all of the Indian population.
Comparative Analysis: Global Versus Indian Telemedicine Scenario
This section discusses a comparative evaluation of the global and Indian telemedicine ecosystems with respect to shared outlines and divergent paths formed by distinct technological, regulatory, and socio-economic factors.82–84 Table 2 summarizes key aspects of the telemedicine landscapes both globally and in India, Table 3 compares global and Indian market values between 2000 and 2024, which is illustrated in Figure 2.
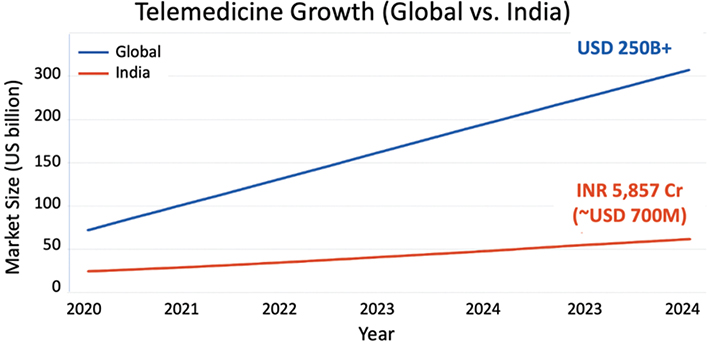
Fig. 2. Telemedicine market growth. Cr, crore: used to symbolize 10 million, INR: Indian Rupee, USD: U.S. dollar.
Market Size and Economic Scale
When comparing the market size globally versus India, the global telemedicine market is larger. Statista 2024, revealed that the global market crossed $250 billion in 2024.9 Whereas the Indian market a CAGR of 31%, remains at ~USD 700 million.85 This comparison reflects the infrastructure maturity, income, health investment, etc. However, government in India has initiated potential scalability through ABDM and increased public–private partnerships.
Technology Ecosystem
The technology ecosystem is accepted globally; therefore, telemedicine can be easily integrated into advanced technologies such as wearable health monitors, AI-driven diagnostics, and 5G-enabled remote surgery.86 Real-time integration into EHRs87 is successful globally, but in India telemedicine platforms are mobile centric, with smartphones app, WhatsApp bots, and interactive voice response (IVR) systems,88 However, this model reaches Tier 2 and 3 cities but not in rural areas.
Regulatory Landscape
The U.S. and EU have established regulatory frameworks such as HIPAA and GDPR to ensure data privacy in the digital health ecosystems.89 This framework improves the cross-platform interoperability, whereas in India, regulatory evaluation is more recent. Telemedicine Practice Guidelines (2020) provide valid legal teleconsultation and an NDHM/ABDM architecture supports privacy in the health data ecosystem.90 In India, the government applies telemedicine regulations to the population, which facilitates its use widely.
Key Barriers to Adoption
Key barriers to adoption of telehealth globally include physician licencing, integration of health systems, and patient data governance.91 In India, imparting the infrastructural and socio-cultural is difficult apart from key barrier adoption. The IAMAI observed that only 37% of rural Indian households have internet access. And this limits the potential of telehealth to reach remote populations.92
Opportunities and Strategic Potential
When comparing strategic opportunities globally versus Indian scenarios, countries globally make use of the AI-driven remote monitoring and interoperable insurance platform’s93 Startups and health tech giants are exploring cloud-based virtual hospitals, remote chronic care, and robot-assisted surgery94 for better opportunities. On the other hand, in India, with over 65% of the population residing in rural areas,95 the government plans to link 150,000 HWCs under Ayushman Bharat96 to digital teleconsultation hubs to offer the opportunities to all Indians. Finally, this comparison reveals that the global and Indian telemedicine ecosystems differ in scale, technology, and policy maturity.
Discussion
This article reveals that while India’s telemedicine growth path broadly aligns with global trends, it is characterized by distinct local challenges and contextual innovations.97 The COVID-19 pandemic served as a critical catalyst globally and within India, triggering rapid digital health adoption across clinical, administrative, and public health domains. However, the evolution of telemedicine in India has diverged in terms of scale, infrastructure readiness, technological sophistication, and user demographics.98 Globally, countries with robust digital infrastructure and universal health coverage systems, such as the United States, Germany, Sweden, and Australia, witnessed swift institutionalization of telemedicine through insurer reimbursement models, EHR integration, and AI-powered clinical decision support.96 In contrast, India’s strategy has been policy-driven and resource-awareness, with a greater focus on equitable access than on technological complexity.
Rural Telemedicine: A Transformational Opportunity
India’s rural health divide signifies the most important barrier and the greatest opportunity for telemedicine expansion.35 More than 65% of India’s population lives in rural zones, several of which lack professional access and appropriate primary care. Initiatives such as eSanjeevani AB-HWC,64 which connect frontline workers in remote HWCs with district and tertiary care physicians via real-time video consultation, are redefining how care is delivered beyond urban geographies. Early impact assessments from the Ministry of Health (2023)41 designate better access to maternal care, dermatology, and chronic disease management in rural clusters through teleconsultation hubs. If scaled and stabilized, such models can decentralize specialist care, reduce travel costs for patients, and enhance early intervention rates in non-communicable diseases.
Technological Integration and the Role of AI/IoT
The telemedicine relies on AI-driven diagnostics, IoT integration, and patient monitoring for population health management.97 High-income countries98 previously integrated wearables (e.g. heart rate sensors, glucose monitors), smart imaging systems, and clinical decision algorithms) into virtual care pathways. India, though at initial stage in this development, is starting to integrate such technologies in urban telehealth platforms. For instance, platforms such as Practo23 and mfine69 with AI-driven dermatology assessment tools and chatbot triage systems, support technological advancement in telemedicine. Furthermore, pilot projects funded under the Digital India HealthTech Mission are investigating low-cost IoT-enabled kits for home-based monitoring of vital signs in patients with chronic diseases. Still, these combinations continue to be focused in metros and corporate hospitals. Connecting the tech-access gap between urban and rural India will require considerable investment in infrastructure, literacy, and localized algorithm development.
Role of Public–Private Partnerships and Policy Ecosystems
To achieve telemedicine success, collaboration among multistake collaboration is essential. The government has taken initiatives with NDHM42,66 and ABDM99,65,90 to get reliable ground work. Such private partnerships include Apollo Telehealth’s23,71 partnerships and Tata Trust support for AI-based maternal care monitoring in tribal areas. Collaborations with telecom providers enable low-bandwidth video consultations in underserved regions. This private sector organization provides innovation and consumer centric design for promoting the reach of telemedicine. In addition, medical legal accountability and data protection laws for digital health platforms were regularised under the Digital Personal Data Protection Act, 2023 (India).
Study’s Limitations
This article largely depended on secondary data sources, which may support telemedicine adoption in remote areas. Quickly developing telehealth policies and technological deployment were limited assessments. Moreover, rural acceptance metrics are controlled by digital literacy and network access, which might bias influence assessments toward urban-centric insights. These restrictions should guide careful understanding of conclusions and notify upcoming experimental revisions.
Synthesis and Suggestions
Policy driven and mobile-first models are examples of approaches for the rapid expansion of Indian telemedicine, whereas global AI-driven strategies offer predictive care and sophisticated support for telemedicine growth. Furthermore, telemedicine in India and similar low- and middle-income countries depend on the digital divide, technological adaptation, digital literacy, and public and a private partnership policy framework.
Conclusion
This article reviewed telemedical growth globally and in India, reflecting the broader digital health transformation by the COVID-19 pandemic. Comparative analysis was done with global countries and India, where the telemedicine framework scheme to promote the telemedicine consultation and legal framework to support telemedicine safety, licencing and insurance policies were discussed. Next, the technological adoption with the telemedicine acceptance globally and in India was discussed. Globally, countries have already initiated technological adaptation with wearable devices, Artificial intelligence and the IoT support success in telemedicine advancement, while India needs more initiatives to promote the telemedicine. These include addressing the digital divide, rural area promotion, broad band connectivity, and digital literacy, which Practo and the mfine app are supporting telemedicine. Finally, support and collaboration between private and public sector stakeholders are needed to address regularity and reimbursement challenges. Finally, the authors conclude that India is well positioned to emerge as a global leader in scalable telemedicine solutions as it continues innovation to ensure the equitable healthcare access for all as in the global community.
Contributions
S. Hemalatha conceived of the research, designed the overall methodology, and supervised the study. Kiran Mayee Adavala conducted the literature review and contributed to the theoretical framework. Pullela SVVSR Kumar was responsible for data collection, preprocessing, and experimental implementation. N. Muthuvairavan Pillai performed data analysis, validation of results, and interpretation of findings. S. Muruganandam contributed to the development of algorithms/models and assisted in result visualization and performance evaluation. G. Krishna Mohan drafted the original manuscript and coordinated revisions. All authors reviewed, edited, and approved the final manuscript.
Data Availability Statement (DAS), Data Sharing, Reproducibility, and Data Repositories
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Application of AI-Generated Text or Related Technology
None.
Acknowledgments
The authors thank their respective institutions for providing the necessary infrastructure and support to carry out this collaborative research. The authors also acknowledge the valuable feedback and suggestions received from colleagues and reviewers, which helped improve the quality of this manuscript.
References
- Alenoghena CO, Ohize HO, Adejo AO, Onumanyi AJ, Ohihoin EE, Balarabe AI, et al. Telemedicine: a survey of telecommunication technologies, developments, and challenges. J Sens Actuator Netw. 2023;12(2):20. https://doi.org/10.3390/jsan12020020
- Dodge M, Werner K. Telemedicine: history, foundation, and clinical implementation. In: Patel D, editor. Digital health. London: Academic Press; 2025. p. 41–62.
- Hyder M, Razzak J. Telemedicine in the United States: an introduction for students and residents. J Med Internet Res. 2020;22(11):e20839. https://doi.org/10.2196/20839
- Zobair KM, Sanzogni L, Sandhu K. Telemedicine healthcare service adoption barriers in rural Bangladesh. Aust J Inf Syst. 2020;24:1–20.
- Nosike CJ, Nosike UC. Navigating the challenges and seizing the opportunities amidst the COVID-19 pandemic: a comprehensive review. Niger J Afr Stud. 2024;6(1):1–15.
- Thompson M, Walker O. Global integration of AI-powered telemedicine: innovations, challenges, and the future of healthcare delivery. Preprints. 2025. https://doi.org/10.20944/preprints202505.0323.v1
- Giansanti D, Costantini G. Artificial intelligence in public health: bridging today’s trends with tomorrow’s possibilities. Bioengineering. 2025;12(6):559. https://doi.org/10.3390/bioengineering12060559
- Mukherjee K. Research on healthcare innovations in India: before, during and beyond COVID-19. SSRN Electron J. 2021. https://doi.org/10.2139/ssrn.3984999
- Jones-Esan L, Somasiri N, Lorne K. Enhancing healthcare delivery through digital health interventions: a systematic review on telemedicine and mobile health applications in low and middle-income countries (LMICs). Res Square. 2024. https://doi.org/10.21203/rs.3.rs-5189203/v1
- Ali SA, Arif TB, Maab H, Baloch M, Manazir S, Jawed F, et al. Global interest in telehealth during COVID-19 pandemic: an analysis of Google Trends™. Cureus. 2020;12(9):e10487. https://doi.org/10.7759/cureus.10487
- Qizi YFU. Telemedicine in the digital era: navigating the international legal landscape to expand global healthcare access. Int J Legal Inf. 2024;52(2):155–65. https://doi.org/10.1017/jli.2024.37
- Wosik J, Fudim M, Cameron B, Gellad ZF, Cho A, Phinney D, et al. Telehealth transformation: COVID-19 and the rise of virtual care. J Am Med Inform Assoc. 2020;27(6):957–62. https://doi.org/10.1093/jamia/ocaa067
- Alam S, Gupta A, Panas A. McKinsey on healthcare: weathering the storm. 2022.
- Morrison C, Rimpiläinen S, Bosnic I, Thomas J, Savage J. Emerging trends in digital health and care: a refresh post-COVID. Digital Health & Care Institute; 2022.
- Greenhalgh J. Understanding the complexities of collecting and using PRO data in a primary care context. BMJ Qual Saf. 2022;31(3):175–8. https://doi.org/10.1136/bmjqs-2021-013315
- Rajkumar E, Gopi A, Joshi A, Thomas AE, Arunima NM, Ramya GS, et al. Applications, benefits and challenges of telehealth in India during COVID-19 pandemic and beyond: a systematic review. BMC Health Serv Res. 2023;23:7. https://doi.org/10.1186/s12913-022-08970-8
- Kamau JK. Reducing patient no-show rates in a mental health outpatient clinic [Internet]. Walden Dissertations and Doctoral Studies; 2025. Available from: https://scholarworks.waldenu.edu/dissertations/17396 [2 August 2025].
- Ahmed S, Yong J, Shrestha A. The integral role of intelligent IoT system, cloud computing, artificial intelligence, and 5G in the user-level self-monitoring of COVID-19. Electronics. 2023;12(8):1912. https://doi.org/10.3390/electronics12081912
- Sklar T, Robertson C. The states’ hodgepodge of physician licensure regulations. J Law Med Ethics. 2024;52(2):419–21. https://doi.org/10.1017/jme.2024.113
- Owolabi EO, Mac Quene T, Louw J, Davies JI, Chu KM. Telemedicine in surgical care in low- and middle-income countries: a scoping review. World J Surg. 2022;46:1855–69. https://doi.org/10.1007/s00268-022-06549-2
- Mathew M. Integrated health care delivery and telemedicine: existing legal impediments in India. In: Dutta P, Chakrabarti S, Bhattacharya A, Dutta S, Shahnaz C, editors. Emerging technologies in data mining and information security. Lecture Notes in Networks and Systems. Vol. 490. Singapore: Springer; 2023. p. 713–24.
- Srivastava A. Connecting care: global best practices & the rise of Indian digital health ecosystem. New Delhi: Blue Rose Publishers; 2024.
- Narwadiya SC, Rao DR. Telemedicine in India: an impact analysis. Intell Hosp. 2025;1(1):100004. https://doi.org/10.1016/j.inhs.2025.100004
- Sindakis S, Showkat G. The digital revolution in India: bridging the gap in rural technology adoption. J Innov Entrep. 2024;13:29. https://doi.org/10.1186/s13731-024-00380-w
- Vasanthan L, Natarajan SK, Babu A, Kamath MS, Kamalakannan S. Digital health interventions for improving access to primary care in India: a scoping review. PLoS Glob Public Health. 2024;4(5):e0002645. https://doi.org/10.1371/journal.pgph.0002645
- Jeffery R. Health policy and federalism in India. Territ Polit Gov. 2021;10(1):67–85. https://doi.org/10.1080/21622671.2021.1899976
- Kolasa K, Kozinski G. How to value digital health interventions? A systematic literature review. Int J Environ Res Public Health. 2020;17(6):2119. https://doi.org/10.3390/ijerph17062119
- Ahmed MM, Okesanya OJ, Olaleke NO, Adigun OA, Adebayo UO, Oso TA, et al. Integrating digital health innovations to achieve universal health coverage: promoting health outcomes and quality through global public health equity. Healthcare (Basel). 2025;13(9):1060. https://doi.org/10.3390/healthcare13091060
- Aremu SO, Oruye ML, Adamu EI, Vuetkung NM, Jonathan DA, Janjaro AG, et al. In Sub-Saharan Africa. Discov Public Health. 2025;22:285. https://doi.org/10.1186/s12982-025-00689-1
- Awosiku OV, Gbemisola IN, Oyediran OT, Egbewande OM, Lami JH, Afolabi D, et al. Role of digital health technologies in improving health financing and universal health coverage in Sub-Saharan Africa: a comprehensive narrative review. Front Digit Health. 2025;7:1391500. https://doi.org/10.3389/fdgth.2025.1391500
- Raj GM, Dananjayan S, Agarwal N. Inception of the Indian Digital Health Mission: Connecting…the…Dots. Health Care Sci. 2023;2:345–51. https://doi.org/10.1002/hcs2.67
- Glasgow RE, Battaglia C, McCreight M, Ayele R, Maw AM, Fort MP, et al. Use of the reach, effectiveness, adoption, implementation, and maintenance (RE-AIM) framework to guide iterative adaptations: applications, lessons learned, and future directions. Front Health Serv. 2022;2:959565. https://doi.org/10.3389/frhs.2022.959565
- Deimel L, Hentges M, Thiel R. The European health data space and the future of cross-border healthcare. In: Scheuer A, Studzinski J, editors. Digital maturity in hospitals. Cham: Springer; 2025.
- Malhotra P, Ramachandran A, Chauhan R, Soni D, Garg N. Assessment of knowledge, perception, and willingness of using telemedicine among medical and allied healthcare students studying in private institutions. Telehealth Med Today. 2020;5(4). https://doi.org/10.30953/tmt.v5.228
- Venkataraman A, Fatma N, Edirippulige S, Ramamohan V. Facilitators and barriers for telemedicine systems in india from multiple stakeholder perspectives and settings: a systematic review. Telemed J E Health. 2024;30(5):1341–56. https://doi.org/10.1089/tmj.2023.0297
- Kadu A, Singh M. Comparative analysis of e-health care telemedicine system based on internet of medical things and artificial intelligence. In: 2021 2nd International Conference on Smart Electronics and Communication (ICOSEC). Trichy, India; 2021. p. 1768–1775.
- Talvekar S, Khonde T, Hajbe J, Patle S. The evolving role of telemedicine in expanding access to healthcare: benefits, barriers, and future directions. In: 2025 International Conference on Machine Learning and Autonomous Systems (ICMLAS). Prawet, Thailand; 2025. p. 1198–1202.
- Krzyzanowski M, Cohen A. Update of WHO air quality guidelines. Air Qual Atmos Health. 2008;1: 7–13. https://doi.org/10.1007/s11869-008-0008-9
- Zou T, Cheshmehzangi A. ICT adoption and booming E-commerce usage in the COVID-19 Era. Front Psychol. 2022;13:916843. https://doi.org/10.3389/fpsyg.2022.916843
- Pushp A, Gautam RS, Tripathi V, Kanoujiya J, Rastogi S, Bhimavarapu VM, et al. Impact of financial inclusion on India’s economic development under the moderating effect of internet subscribers. J Risk Financ Manag. 2023;16(5):262. https://doi.org/10.3390/jrfm16050262
- Verma A, Rana A, Monga H, Chaudhary A, Singh J. Distribution management of drugs/medicines and vaccines vis-à-vis Free Drugs Service Initiative (FDSI) of Ministry of Health and Family Welfare (MoHFW), Government of India in the Indian states. In: Proc 9th Int Conf Reliability, Infocom Technologies and Optimization (ICRITO). Noida, India; 2021. p. 1–5.
- Bhandari Y, Das A, Kumar P. Digital literacy of the Indian health workforce: a core requirement for healthcare delivery in the 21st century. J Surg Spec Rural Pract. 2025;6(1):9–12. https://doi.org/10.4103/jssrp.jssrp_6_25
- Sarkis-Onofre R, Catalá-López F, Aromataris E, Lockwood C. How to properly use the PRISMA Statement. Syst Rev. 2021;10:117. https://doi.org/10.1186/s13643-021-01671-z
- Huguet M, Sarazin M, Perrier L, Augusto V. How we can reap the full benefit of teleconsultations: economic evaluation combined with a performance evaluation through a discrete-event simulation. J Med Internet Res. 2022;24(5):e32002. https://doi.org/10.2196/32002
- Cheng TC, Yip W. Policies, progress, and prospects for internet telemedicine in China. Health Syst Reform. 2024;10(2). https://doi.org/10.1080/23288604.2024.2389570
- Venturoli S, Bertoldi A, Manaresi E, Lazzarotto T, Gallinella G. Epidemiology of parvovirus B19 infection in an Italian metropolitan area, 2012–2024: COVID-19 pre-pandemic, pandemic and post-pandemic trends. J Med Virol. 2025;97(3):e70296. https://doi.org/10.1002/jmv.70296
- Patel C, Sinha K. Digitalization of healthcare system in India—a perspective and PESTLE analysis. In: Kaiser MS, Bandyopadhyay A, Ray K, Singh R, Nagar V, editors. Proceedings of trends in electronics and health informatics. Lecture Notes in Networks and Systems, vol. 376. Singapore: Springer; 2022.
- Portz J, Moore S, Bull S. Evolutionary trends in the adoption, adaptation, and abandonment of mobile health technologies: viewpoint based on 25 years of research. J Med Internet Res. 2024;26:e62790. https://doi.org/10.2196/62790
- Wong MYZ, Gunasekeran DV, Nusinovici S, Sabanayagam C, Yeo KK, Cheng CY, et al. Telehealth demand trends during the COVID-19 pandemic in the top 50 most affected countries: infodemiological evaluation. JMIR Public Health Surveill. 2021;7(2):e24445. https://doi.org/10.2196/24445
- Nkurunziza JMV, Udahemuka JC, Dusenge JB, Umutesi F. Overview of trending medical technologies. Glob Clin Eng J. 2022;43:16–46.
- Koppel R.Estimating the United States’ cost of healthcare information technology. In: Kiel JM, Kim GR, Ball MJ, editors. Healthcare information management systems. Health Informatics. Cham: Springer; 2022.
- Bincoletto G. Data protection issues in cross-border interoperability of electronic health record systems within the European Union. Data Policy. 2020;2:e3. https://doi.org/10.1017/dap.2020.2
- Hashiguchi TCO. Bringing health care to the patient: an overview of the use of telemedicine in OECD countries. OECD Health Working Papers. 2020;(116):1–101. https://doi.org/10.1787/8e56ede7-en
- Awala EV, Olutimehin D. Revolutionizing remote patient care: the role of machine learning and AI in enhancing tele-pharmacy services. World J Adv Res Rev. 2024;24(3):1133–1149. https://doi.org/10.30574/wjarr.2024.24.3.3831
- Jiang X, Xie H, Tang R, Du Y, Li T, Gao J, et al. Characteristics of online health care services from China’s largest online medical platform: cross-sectional survey study. J Med Internet Res. 2021;23(4):e25817. https://doi.org/10.2196/25817
- Cuadros DF, Huang Q, Mathenjwa T, Gareta D, Devi C, Musuka G. Unlocking the potential of telehealth in Africa for HIV: opportunities, challenges, and pathways to equitable healthcare delivery. Front Digit Health. 2024;6:1278223. https://doi.org/10.3389/fdgth.2024.1278223
- Prata N, Weidert K, Dushimeyesu E, Kanyamanza E, Blaise D, Umutesi S, et al. Innovation through telemedicine to improve medication abortion access in primary health centers: findings from a pilot study in Musanze District, Rwanda. BMC Public Health. 2025;25:1681. https://doi.org/10.1186/s12889-025-22629-z
- Tschider C, Compagnucci MC, Minssen T. The new EU–US data protection framework’s implications for healthcare. J Law Biosci. 2024;11(2):lsae022. https://doi.org/10.1093/jlb/lsae022
- Brotman JJ, Kotloff RM. Providing outpatient telehealth services in the United States: before and during coronavirus disease 2019. Chest. 2021;159(4):1548–1558. https://doi.org/10.1016/j.chest.2020.11.020
- Ejiogu C. The role of satellite internet in bridging the digital divide. 2025. Available from: https://www.theseus.fi/handle/10024/893826
- Ahmed Z, Osifowokan AS, Filani A, Donkor AA. Comprehensive analysis of cyber attacks and data breaches in the US health sector: identifying vulnerabilities and developing proactive defense strategies. Comput Sci IT Res J. 2025;6(2):1–12. https://doi.org/10.51594/csitrj.v6i2.1833
- Omboni S, Padwal RS, Alessa T, Benczúr B, Green BB, Hubbard I, et al. The worldwide impact of telemedicine during COVID-19: current evidence and recommendations for the future. Connect Health. 2022;1:7–35. https://doi.org/10.20517/ch.2021.03
- Garg V, Kumar H, Bansal R, Bhardwaj A. Envisioning digital health technology innovations for 2025: enhancing digital interventions in the post-COVID-19 era. In: Garg V, Goyal M, Kumar H, editors. Innovations in healthcare technologies in India. Singapore: Springer; 2025.
- Choudhary S, Ghosh P. eSanjeevani—National Telemedicine Service: evolution, opportunities, and challenges. Indian J Prev Soc Med. 2024;55(4):253–8.
- Mishra US, Yadav S, Joe W. The Ayushman Bharat Digital Mission of India: an assessment. Health Syst Reform. 2024;10(2). https://doi.org/10.1080/23288604.2024.2392290
- Aggarwal L, Roy M. A strategic roadmap to the successful implementation of digital health records in India [Internet]. Seven Editora; 2023. Available from: https://sevenpubl.com.br/editora/article/view/3146 [2 August 2025].
- Dorsey ER, Topol EJ. Telemedicine 2020 and the next decade. Lancet. 2020;395(10227):859.
- Bagga G, Singh H, Hood MM. Revolutionizing Indian healthcare: the impact of digital health, AI, telemedicine, and data security. IOSR J Bus Manag. 2024;26(9):30–4. https://doi.org/10.9790/487X-2609013034
- Goel M. Bilateral S&T cooperation: India with neighbouring countries. In: Science diplomacy for South Asian countries. Singapore: Springer; 2021. https://doi.org/10.1007/978-981-16-3025-5_6
- Viswanadham N. Ecosystem model for healthcare platform. Sādhanā. 2021;46:188. https://doi.org/10.1007/s12046-021-01708-y
- Sinha N, Rahul R. India’s digital health transformation: advancements and challenges in telemedicine. J Kebidanan Manna. 2024;3(2):55–66. https://doi.org/10.58222/jkm.v3i2.1200
- Saha B. Telehealth transformation in India: a study on Apollo Hospitals. Cambridge Scholars Publishing; 2025.
- Al-Emran M, Griffy-Brown C. The role of technology adoption in sustainable development: overview, opportunities, challenges, and future research agendas. Technol Soc. 2023;73:102240. https://doi.org/10.1016/j.techsoc.2023.102240
- Gizaw Z, Astale T, Kassie GM. What improves access to primary healthcare services in rural communities? A systematic review. BMC Prim Care. 2022;23:313. https://doi.org/10.1186/s12875-022-01919-0
- Chakraborty I, Ilavarasan PV, Edirippulige S. COVID-19 as a catalyst for telehealth growth in India: some insights. J Int Soc Telemed EHealth. 2021;9:e3(1–4). https://doi.org/10.29086/JISfTeH.9.e3
- Mahapatra P, Sahoo KC, Pati S. A longitudinal qualitative study on physician experience in managing multimorbidity across the COVID-19 pandemic in Odisha, India. Sci Rep. 2024;14:12866. https://doi.org/10.1038/s41598-024-60473-0
- Bhattacharya S, Bhattacharya C. Sustainable human resource planning for hospitals in tier 2/3 cities: evidence from India. Int J Organ Anal. 2023;31(2):476–507. https://doi.org/10.1108/IJOA-07-2020-2289
- Ramakrishnappa V. Exclusion of Scheduled Tribes in access to digital services in India: bottlenecks and the way forward. East Afr Scholars J Econ Bus Manag. 2022;5(9):251–5. https://doi.org/10.36349/easjebm.2022.v05i09.001
- Sharma AE, Lisker S, Fields JD, Aulakh V, Figoni K, Jones ME, et al. Language-specific challenges and solutions for equitable telemedicine implementation in the primary care safety net during COVID-19. J Gen Intern Med. 2023;38:3123–33. https://doi.org/10.1007/s11606-023-08304-2
- Sitarz M, Gliwa A, Dudzińska E. Telemedicine as a new form of medical services—legal aspect. Teka Kom Prawniczej PAN Oddz W Lublinie. 2023;16(2):519–36. https://doi.org/10.32084/tkp.8112
- Davidescu AA, Manta EM, Birlan I. Economic policies for sustainable healthcare: a comparative analysis of telemedicine in Europe. In: Sustainability development through green economics. Emerald Publishing; 2024. p. 191–217.
- Dileep VN. The coming of age of digital technologies in global health within the Indian context: a review. J Egypt Public Health Assoc. 2024;99:22. https://doi.org/10.1186/s42506-024-00169-5
- Iodice G, Tregua, M, Bifulco F. Sustainability and innovation perspectives in social enterprises: a comparative analysis across Asia and Europe. In: Remondes J, Remondes F, Serrano V, editors. New trends for the governance of non-profit organizations. IGI Global Scientific Publishing; 2025. p. 141–72.
- Malafeyev O, Zaitseva I, Qodirov A, Smirnova T, Yuldasheva S, Kaznacheeva O.Blockchain technologies as a driver of international online-commerce in the global healthcare marketplace. In: 6th Int Conf Control Syst, Math Modeling, Autom Energy Efficiency (SUMMA). Lipetsk, Russia; 2024. p. 211–6.
- Gupta M, Singh K, Kochhar N, Kumar N, Krishnan N, Sreedhara VB, et al. The India Development Update (IDU) [Internet]. World Bank; 2024. Available from: https://thedocs.worldbank.org/en/doc/18e328e242c0a01bfcb5693e425bb0d8-0310012024/original/WB-IDU-September-2024.pdf [2 August 2025].
- The Synergy of 5G and Artificial Intelligence (AI) in modern healthcare. Int J Environ Sci. 2025;11(11s):1040–52. https://doi.org/10.64252/jxk9pz54
- Onigbogi O, Ojo OY, Kinnunen U-M, Saranto K. Mobile health interventions on vaccination coverage among children under 5 years in low and middle-income countries: a scoping review. Front Public Health. 2025;13:1392709. https://doi.org/10.3389/fpubh.2025.1392709
- Fernandes F, Chaltikyan G. Analysis of legal and regulatory frameworks in digital health: a comparison of guidelines and approaches in the European Union and United States. J Int Soc Telemed EHealth. 2020;8:e11(1–13). https://doi.org/10.29086/JISfTeH.8.e11
- Nambiar U, Tandon A, Gupta AK, Sivapuram MS, Ajarananda V. DHM2-TS framework for evaluation of tele-health platforms and solutions: a multi user-centered perspective. In: Pandey R, Gupta A, Pandey A, editors. The Internet of Medical Things (IoMT) and telemedicine frameworks and applications. IGI Global Scientific Publishing; 2023. p. 207–29.
- Xia L, Cao Z, Zhao Y. Paradigm transformation of global health data regulation: challenges in governance and human rights protection of cross-border data flows. Risk Manag Healthc Policy. 2024;17:3291–304. https://doi.org/10.2147/RMHP.S450082
- Setia P. Digital technologies and inclusion: the SAID model for policymaking and program development. Ahmedabad: Indian Institute of Management; 2024.
- Askari S, Ghofrani A, Taherdoost H. Fintech-enabled telemedicine: global healthcare advancement. In: Taherdoost H, Le N, Madanchian M, Farhaoui Y. editors. Exploring Global FinTech Advancement and Applications. IGI Global Scientific Publishing; 2024. p. 313–30.
- Twomey M. Healthcare technology international perspective report [Internet]. 2022. Available from: https://hih.ie/downloads/knowledge-network/innovation-publications/HIHI_2022_International_Perspective-Report.pdf [2 August 2025].
- Ferari C, Mitchell K, Crigger C, Zupper S, Wildasin A, Ost M, et al. Bridging the gap—building surgical subspecialty telemedicine clinics in the rural setting. Urol Pract. 2022;9(2):126–33. https://doi.org/10.1097/UPJ.0000000000000284
- Bajpai N, Wadhwa M. India’s experience with ICT in the health sector: lessons for sub-Saharan Africa [Internet]. ICT India Working Paper. 2021;51. Available from: https://www.econstor.eu/bitstream/10419/249840/1/ICT-India-Working-Paper-51.pdf [2 August 2025].
- Singh M, Chand K, Singh M. Navigating challenges and innovations in global healthcare. In: Kukreti M, Chatterjee S, Banerjee A, editors. Driving global health and sustainable development goals with smart technology. IGI Global Scientific Publishing; 2025. p. 303–38.
- Mishra V, Sharma MG. Digital transformation evaluation of telehealth using convergence, maturity, and adoption. Health Policy Technol. 2022;11(4):100684. https://doi.org/10.1016/j.hlpt.2022.100684
- Wilson D, Sheikh A, Görgens M, Ward K; World Bank. Technology and universal health coverage: examining the role of digital health. J Glob Health. 2021;11:16006. https://doi.org/10.7189/jogh.11.16006
- Kadarpeta RSR, Anand JS, Achungura G. Strengthening public financing of primary healthcare in India: a perspective. Health Serv Insights. 2024;17:1–7. https://doi.org/10.1177/11786329241249289
Copyright Ownership: This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See http://creativecommons.org/licenses/by-nc/4.0. The authors of this article own the copyright.