ORIGINAL RESEARCH
Determinants of The Willingness to Adopt Telehealth Technology Among Health Professionals in a Tertiary Hospital
Michael Mensah, MSc1  ; Sampson Opoku, PhD2
; Sampson Opoku, PhD2  ; Annabel Aku Anum, MA3
; Annabel Aku Anum, MA3  ; Theophilus Brocke, MPH4
; Theophilus Brocke, MPH4  ; Enoch Makafui Mensah, BSc5
; Enoch Makafui Mensah, BSc5  ; Ernest Obeng Nsiah, BSc6
; Ernest Obeng Nsiah, BSc6  ; Yaa Adutwumwaa Owusu-Ansah, FGCNM7
; Yaa Adutwumwaa Owusu-Ansah, FGCNM7  ; Ernest Yeboah Asamo, PhD(c)7
; Ernest Yeboah Asamo, PhD(c)7 
1Researcher, Department of Research, Family Health Medical School, Family Health University College, Teshie-Accra, Ghana; 2Lecturer, Department of Community Health, Family Health Medical School, Family Health University College, Teshie-Accra, Ghana; 3Researcher, Department of Gastroenterology, Korle Bu Teaching Hospital, Accra, Ghana; 4Department of Obstetrics and Gynaecology, Korle Bu Teaching Hospital, Accra, Ghana; 5Biostatistician, Department of Mathematics and Statistics, College of Science, Kwame Nkrumah University of Science and Technology, Kumasi, Ghana; 6Researcher, Department of Mental Health and Addiction, Claresholm Centre for Mental Health and Addiction, Claresholm, Alberta, Canada; 7Researcher, Department of Politics and International Relations, Florida International University, Florida, United States
Keywords: Digital healthcare, electronic health records, Ghana, healthcare professionals, telehealth adoption, telehealth technology
Abstract
Background: Digitalization in healthcare, particularly through electronic health records and telehealth, is transforming healthcare delivery globally. However, challenges in adoption persist, particularly in resource-limited settings.
Aim: This study aimed to determine the factors influencing the willingness to adopt telehealth technology among health professionals in a tertiary hospital in Ghana.
Methods: A cross-sectional study was conducted from September 2021 to May 2022 at Korle Bu Teaching Hospital, targeting departments that had transitioned to the use of electronic health records. Stratified random sampling was used to recruit 223 doctors and nurses. Data were collected electronically and analyzed using SPSS version 26. Chi-square tests and multivariate logistic regression were applied to determine the relationship between variables.
Results: Of the 223 participants, 217 were included in the analysis. Among the 217 participants, 48% were willing to adopt telehealth technology. Factors associated with willingness to adopt telehealth included sex, qualification, profession, department, years in healthcare, work experience, knowledge and training in information technologies (IT), high IT proficiency, familiarity with telemedicine apps, and familiarity with telemedicine tools. These factors were significantly associated with willingness to adopt telehealth technology. From the logistic regression analysis, age group, familiarity with telehealth, and working years were significant predictors.
Conclusion: Demography and organizational factors impacted telehealth adoption at Korle-bu Teaching Hospital. To ensure successful integration into routine clinical practice, it is essential to implement hands-on training, tailor departmental strategies, and institute supportive policies, including digital infrastructure and literacy initiatives in the health facilities.
Plain Language Summary
This cross-sectional study assessed the readiness and willingness of healthcare professionals at Ghana’s Korle Bu Teaching Hospital (KBTH) to adopt digital technologies such as Electronic Health Records (EHRs) and telehealth. The study, which took place from September 2021 to May 2022, surveyed 217 doctors and nurses from departments that had already adopted EHRs. Using chi-square tests and multivariate logistic regression, the researchers found that 48% of the participants were willing to embrace telehealth. Several factors, including sex, qualifications, department, and IT knowledge, were significantly associated with the willingness for adoption. Specifically, the number of years a professional had been working was identified as a key predictor. The study concludes that a successful integration of telehealth at KBTH will require targeted interventions such as hands-on training and supportive policies to address these demographic, professional, and organizational factors.
Citation: Telehealth and Medicine Today © 2026, 11: 621
DOI: https://doi.org/10.30953/thmt.v11.621
Copyright: © 2026 The Authors. This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See http://creativecommons.org/licenses/by-nc/4.0. The authors of this article own the copyright.
Submitted: August 11, 2025; Accepted: December 19, 2025; Published: January 24, 2026.
Corresponding Author: Mensah Michael, Email: mikdicksion.26@gmail.com
Competing interests and funding: The authors declare that no funding supported the development of this article.
The authors declare that they have no conflict of interest.
Digitalization in healthcare is a multifaceted emerging phenomenon. Although it is mainly driven by quick technological innovation, many of these innovations often fall short of meeting the practical needs and expectations of clinicians and patients. This situation contributes to the proliferation of poorly integrated digital solutions across health systems.2,3 Little is understood about how hospital digitalization can be accomplished or how this digitalization fosters an increase in hospital performance, both in terms of quality improvement and cost. Currently, information and communication technology (ICT) plays a pivotal role not only in enabling firms to achieve operational excellence but also in facilitating strategic competitive advantage.4,5,6
In Ghana, the healthcare sector comprises public and private facilities that together deliver healthcare nationwide. Although some of these institutions have begun adopting innovative and digital technologies in their operations, widespread implementation still lags behind.7 A 2017 mHealth study reported that progress in the integration of digital technologies within the health system remained limited, highlighting significant gaps in digital transformation.8 This is primarily due to strict regulations, stakeholder reluctance, unchanged cultural norms, and human factors in a modern technological world.9,10 A cross-sectional study in Nigeria suggests that offering telemedicine services to clients, particularly for emergency and chronic conditions, is a desirable approach. The same study reported that, the level of knowledge on telemedicine was relatively moderate, and cultural barriers were also significant. Results from other studies showed that health workers at varying levels had low knowledge of telemedicine.12 The advantages of telemedicine did not seem relevant to them. There are different levels of expertise and willingness to adopt telehealth technology among various worker groups.2,9,10
Findings from other lower- and middle-income countries (LMICs) demonstrated that the willingness of health workers to adopt telehealth is shaped by a consistent interplay of factors, including infrastructure deficits, institutional readiness, and personal attitudes.13–15 For example, in West African countries such as Ghana, Cameroon, Côte d’Ivoire, Liberia and Nigeria, the primary barriers to the use of digital technologies include poor internet connectivity and inconsistent electricity, alongside an absence of robust national policies and regulatory frameworks.13,16 In addition, countries such as Kenya, Uganda, and Ethiopia face similar technical challenges. These are frequently exacerbated by inadequate funding and local technical support to maintain systems.13,14,16 Despite these hurdles, studies show that health professionals with positive attitudes and strong digital literacy are more willing to use telehealth in some of these countires.17,18
Overcoming resistance to change and providing targeted training can significantly improve acceptance.18 Ultimately, successful adoption hinges on governments and healthcare organizations investing in reliable infrastructure, establishing clear policies, and providing comprehensive training to ensure that health workers are equipped and motivated to use these technologies.9,19 Besides, the above-mentioned findings from LMICs largely align with the technology acceptance model (TAM)-based studies, confirming that perceived usefulness (PU) and perceived ease of use (PEOU) are universal predictors of health worker willingness to adopt telehealth.2,3,20 The main distinction is that in LMICs, individual perceptions are overwhelmingly dependent on fundamental external factors: the availability of basic infrastructure (internet, electricity), training and digital literacy, and clear institutional policy.7,16 This means that for broader telehealth adoption policies to be effective in these regions, they must first prioritize essential infrastructure investment and robust regulatory frameworks before focusing solely on changing individual attitudes or system design.2,17 Studies on the use of TAM to focus on health professionals’ behavioral intent to adopt digital technologies among medical staff in Ghana are scarce. Hence, this study seeks to determine the factors affecting the willingness to adopt telehealth technology among health professionals in a tertiary hospital in Ghana.
Methodology
This cross-sectional study was conducted from September 1, 2021, to May 1, 2022, to assess the perception and usage of electronic health records (EHRs) among health professionals at KBTH in the Greater Accra Region, Ghana. KBTH is the largest hospital in Ghana and one of the biggest health facilities in West Africa. With steady growth from a 192-bed facility to a 2,000-bed facility, KBTH is the principal national referral center, serving a country with an estimated population of 30 million. Ethical clearance was taken from the KBTH Scientific Technical Committee and the Institutional Review Board. The KBTH began migrating to EHR in 2019, following a successful pretest at the Korle Bu Polyclinic that same year. The study targeted departments, including surgery, family medicine, obstetrics, and ophthalmology, which had already migrated to the EHR system during the study period. The sample included nurses and doctors in these departments.
Sampling and Sample Size Determination
Using a stratified random sampling technique, 223 participants were included in the study after consenting to participate, and a total of 217 were analyzed. From sampling frames of the target population in each stratum, participants were selected randomly without replacement.
Data Collection Procedure
Data collection was conducted through a cross-sectional survey using a structured, self-administered questionnaire developed in Google Forms. To facilitate broad and timely participation, the survey link was disseminated electronically via a professional WhatsApp platform, which was already in use for official communication among the study population. This approach ensured convenient access to the questionnaire while maintaining respondents’ anonymity and minimizing disruptions to their clinical duties. Prior to data collection, participants were informed of the study’s purpose, scope, and the voluntary nature of their participation. Informed consent was obtained electronically at the beginning of the questionnaire, and participants were assured that their responses would be confidential and handled securely. The survey was open for a defined period, during which periodic reminders were issued to enhance the response rate.
The questionnaire was structured into three main sections, each designed to capture specific dimensions relevant to the study objectives. The first section collected socio-demographic and professional background information, including age, sex, educational qualification, clinical role, department, and years of experience. The second section assessed general knowledge and competencies related to digitalization and information and ICTs, including prior training and self-assessed proficiency in IT use. The third section focused on participants’ perceptions and willingness to adopt telehealth technologies, incorporating questions related to awareness, attitudes, perceived usefulness, and readiness for integration into clinical practice.
This digital data collection method was particularly suited to the study context, enabling real-time monitoring of responses, minimizing data entry errors, and ensuring cost-effective and scalable administration among geographically dispersed healthcare professionals (HCPs). Pretesting was conducted to validate and assess the clarity of data collection instruments, and necessary revisions were made before the actual study.
Independent Variables
The independent predictor variables comprise a comprehensive set of attributes that characterize the HCPs participating in the study. These include background characteristics and indicators of digital readiness. Sex (male/female) was included to explore potential gender-based differences in attitudes toward digital technology adoption, acknowledging evidence of gender disparities in digital engagement in some contexts. Educational qualifications were measured across five categories: certificate, diploma/higher national diploma (HND), bachelor’s degree, master’s degree (MSc/MA/MPhil), and doctorate. This variable captures the extent of formal education, which may correspond with differential exposure to information technologies and evidence-based practice, both of which are relevant to digital health uptake.
The professional role was classified primarily as doctor or nurse, recognizing that differences in clinical responsibilities, decision-making authority, and patient interaction may influence digital tool usage and acceptance. Departmental affiliation included categories such as medicine, obstetrics and gynecology, polyclinic, surgery, and unspecified. This variable reflects the clinical context in which HCPs operate, presenting varied demands and opportunities for integrating digital health.
Years of experience in healthcare practice were categorized into three groups: 1 to 2 years, 3 to 5 years, and longer than 6 years. Similarly, tenure at Korle Bu Teaching Hospital, measured using the same groupings, was included to assess the influence of institutional experience on digital technology adoption, particularly exposure to existing technological infrastructures or initiatives within the hospital.
Exposure to practical IT knowledge during training was considered an indicator of foundational digital literacy acquired through formal education. Participation in IT training programs was included to measure formal enhancement of IT competencies, which might support greater confidence in engaging with digital health platforms. Self-assessed IT knowledge level and self-assessed IT proficiency were included as subjective measures of cognitive and functional competence in information technology use, respectively. These indicators capture the respondents’ perceptions of their digital capabilities, which are often influential in shaping behavioral intentions.
Preference for digital storage of personal files was examined as a proxy for general digital orientation. This variable reflects the extent to which individuals integrate digital solutions into their everyday information management practices, which may translate into professional settings. Familiarity with telemedicine applications and telemedicine tools was assessed to measure specific exposure to key digital health technologies. These variables capture both awareness and practical experience with digital health systems that facilitate remote care delivery and are considered essential for determining readiness for broader digital health adoption.
Dependent Variables
The outcome variable for this study was willingness to adopt telehealth technology. This construct reflects the degree to which HCPs are prepared to incorporate telehealth technology into their clinical practice. It was further categorized into two groups: willing (Yes) and not willing (No).
Variable Selection for Logistic Regression
Both theoretical relevance and empirical evidence guided the selection of variables for the logistic regression model. Initially, a set of potential predictor variables was identified based on existing literature, conceptual frameworks related to technology adoption (e.g. TAM and Unified Theory of Acceptance and Use of Technology), and the study objectives. To ensure model parsimony and reduce the risk of overfitting, a two-step approach was employed:
Bivariate Analysis
Each independent variable was first assessed for its association with the dependent variable—willingness to adopt telehealth technology—using chi-square tests for categorical variables. Variables with a p-value < 0.20 in the bivariate analysis were considered eligible for inclusion in the multivariable logistic regression model.
Multivariate Logistic Regression
All eligible variables were entered into a multivariable logistic regression model using the enter method (simultaneous inclusion). The final model retained variables that were statistically significant at p < 0.05 and/or contributed meaningfully to the model, as indicated by changes in the adjusted odds ratios and confidence intervals. Multicollinearity was assessed using variance inflation factors (VIFs), and variables with VIFs greater than 10 were excluded to ensure model stability and accuracy.
Data Management and Analysis
Data were only accessed by investigators on a password-protected computer. The complete data were transferred from Google Forms to Excel in Microsoft Office 365 for cleaning and analysis. The final analysis was performed using RStudio statistical software. Descriptive statistics were performed using frequency, proportion, mean, and standard deviation to describe the data on socio-demography, as well as the use and knowledge of EHR and other ICT tools. Associations between variables were evaluated using the chi-square test of independence, examining the relationship between independent variables and the willingness to adopt telehealth. Multivariate logistic regression, using a forest plot, was employed to report predictors of willingness to adopt telehealth. The acceptance error level was set at a p-value of 0.05.
Results
There were 49% of participants willing to adopt telehealth (Figure 1). Out of 223 participants, 217 were included in the analysis. Among the 217 HCPs who participated, there 57 (26.2%) were male and 160 (73.8%) were females. Most participants hold a bachelor’s degree, with 68 (31.3%) in the Obstetrics and Gynecology Department (p < 0.001, [Appendix A]).
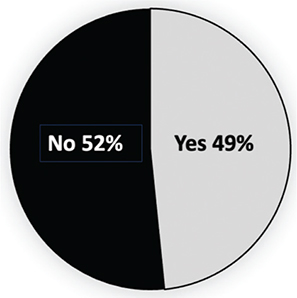
Fig. 1. Distribution of the willingness of participants to adopt telehealth technology.
Males demonstrated a higher willingness (38/57, 66.7%) compared to females (67/160, 41.9%; p = 0.001). Educational qualification strongly influenced adoption, with holders of a doctorate degree showing the greatest willingness (45/48, 93.8%), while those with bachelor’s degrees were less willing (21/68, 30.9%; p = 0.000). Professionally, doctors were far more willing (48/58, 82.8%) than nurses (57/159, 35.8%; p = 0.000). Among departments, the medicine staff showed a significant willingness (52/60, 86.7%; p = 0.000).
There was a significant association between the department (p = 0.000) and years of working at KBTH (p = 0.000) with the willingness to adopt telehealth technology. HCPs in the Medicine Department and those with 3 to 5 years of experience at KBTH were more likely to adopt telehealth technology. Regarding practical insight and training in IT, a majority of the participants (94.6% and 72.1%, respectively) had some level of exposure to IT. However, only 34.6% of the participants reported having a high level of IT knowledge.
A multivariate logistic regression analysis revealed key predictors of willingness to adopt telehealth. Younger age groups (24 to 50 years) showed significantly higher willingness. Conversely, 3 to 5 years of experience at Korle Bu Teaching Hospital was associated with less willingness. Individuals familiar with telehealth tools showed willingness to adopt telehealth technology Figure 2.
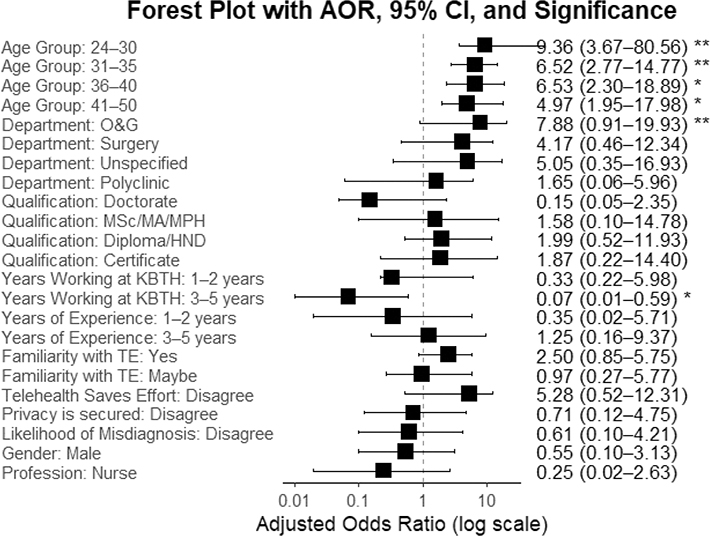
Fig. 2. Predictors of willingness to adopt telehealth technology.
Discussion
This study aimed to determine the factors influencing the willingness to adopt telehealth technology among HCPs in a tertiary hospital in Ghana. Our findings, interpreted through the TAM, indicate that prior IT training significantly boosts PEOU. Concurrently, a professional’s specific role and years of institutional experience strongly influence the perceived usefulness of telehealth in their daily workflow.
These insights directly support Ghana’s National eHealth Strategy by highlighting the need for workforce capacity building. The study’s observation of a higher proportion of female respondents reflects the demographic reality of the healthcare workforce, particularly in nursing. While the study found no statistically significant impact of gender on HCPs’ willingness to adopt telehealth, this specific finding should be contextualized. The broader literature suggests that female patients and clinicians may exhibit higher utilization rates of telehealth. This disparity is often attributed to the perceived convenience and flexibility telehealth offers in balancing professional responsibilities with caregiving roles.10,12,19 Thus, while intrinsic willingness among HCPs might not vary by gender, external factors related to work-life balance could influence actual engagement patterns.
The greater representation of bachelor’s degree holders among respondents, coupled with a strong association with telehealth adoption, highlights the pivotal role of formal education. This suggests that comprehensive degree programs are likely to equip HCPs with greater exposure to digital tools and a foundational understanding of technology, fostering higher acceptance. This aligns with prior research, which consistently links higher education levels to increased acceptance of technology.10,17
Conversely, this study observed that specific vocational qualifications did not significantly influence adoption, reinforcing that a broader academic background may be more influential in shaping general technology readiness. This highlights the importance of integrating digital health competencies into the core of healthcare curricula.
The variation in departmental distribution, with higher numbers from Ob/Gyn and medicine, suggests that the nature of the healthcare facility and its specific services can influence the relevance of telehealth. The observed trend toward significance for the Ob/Gyn department implies that the perceived relevance and practical applicability of telehealth may vary across specialties. For instance, specialties requiring frequent follow-ups or consultations for non-complex conditions might find telehealth more immediately beneficial than those that rely heavily on physical examinations or invasive procedures.2 This highlights the importance of tailoring telehealth implementation strategies to the unique needs and requirements of specific healthcare settings.
Previous reports indicated that early- and mid-career professionals are more receptive to new technology.2,12 This is likely due to their digital naivety, primary responsibility, and having reached a level of clinical competence that enables them to seek out health system solutions and assume supervisory roles, unlike junior staff or clinicians, who might be overwhelmed with foundational learning and with limited access to digital health tools.7,9 This dynamic aligns with the organizational or internal culture at KBTH, where that mid-level staff, often with digital health tools such as EMRs, compares with junior medical staff and consultants. This situation afford them an affinity for digital health tools such as telehealth in health service delivery.21
This suggests that familiarity with a specific healthcare facility’s operational environment and existing workflows can positively influence telehealth adoption.18,22 This could be attributed to a deeper understanding of how telehealth can be effectively integrated into established practices and a greater comfort level with organizational processes. This finding suggests that general professional experience alone may not be sufficient to guarantee acceptance of telehealth. Instead, direct experience with specific telehealth technologies and workflows within a given organizational context appears to be more critical, fostering greater comfort and acceptance among HCPs.21,23
There was a significant association between general familiarity with telehealth tools and willingness to adopt them. This crucial distinction suggests that a conceptual understanding of telehealth is insufficient; practical knowledge and hands-on experience are essential for effective adoption. Also, familiarity with telehealth technology strongly predicts willingness to adopt, a finding consistent with the PEOU construct.20,24 This practical exposure reduces anxiety and risk perception, fundamentally increasing a health worker’s confidence and self-efficacy in utilizing the system. Literature highlights that hands-on experience, rather than theoretical knowledge alone, is critical for cementing positive attitudes toward technology.2,3 Therefore, implementing comprehensive, practical training programs is essential for health systems aiming to achieve successful, widespread telehealth integration.
Mere awareness does not translate into willingness or effective utilization without practical guidance and opportunities to actively use technology for healthcare purposes. Perceived risks, such as performance limitations due to patient technical proficiency or privacy concerns related to data security, can also influence adoption and often necessitate practical training to mitigate these risks.18,19
Strengths and Limitations
This study’s strength is its timely investigation of telehealth adoption at Ghana’s largest hospital, providing crucial, context-specific data. It successfully identifies key determinants, such as age and IT familiarity, which are vital to shaping local digital health policy.
However, its limitations include a single-center design, which restricts the generalizability of the findings. The cross-sectional nature prevents causal inference, while the digital survey method and self-reported data introduce risks of selection and social desirability bias.
Conclusion
Telehealth has demonstrated immense potential to revolutionize healthcare delivery, offering unparalleled convenience and access. However, its equitable and effective integration hinges on a nuanced understanding of the factors influencing its adoption. While HCPs’ willingness is shaped by educational attainment, professional experience within specific organizational contexts, and the critical provision of practical training, patient adoption is significantly impacted by socioeconomic, geographic, and racial/ethnic disparities.
Moving forward, a concerted effort combining targeted education and hands-on training for professionals, tailored departmental implementation strategies, and comprehensive policy interventions will be essential to fully realize the transformative potential of telehealth for all.
Contributors
Mensah Michael contributed conceptualization, methodology, software, data collection, formal analysis, writing the original draft, and reviewing and editing. Opoku Sampson: Proved supervision, formal analysis, writing, reviewing, and editing. Annabel Aku Anum contributed conceptualization, project administration, supervision, writing, reviewing, and editing. Theophilus Brocke and Enoch Makafui Mensah participated in the investigation, software, data collection, writing, reviewing, and editing. Ernest Obeng Nsiah contributed validation, visualization, writing, reviewing, and editing. Yaa Adutwumwaa Owusu-Ansah contributed validation, writing, reviewing, and editing. Ernest Asamoa contributed software, writing, reviewing, and editing.
Data Availability Statement (DAS), Data Sharing, Reproducibility, and Data Repositories
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Application of AI-Generated Text or Related Technology
AI-generated text or related technology was not used.
Acknowledgment
The authors are grateful to Mr. Charles Yeboah for his assistance with the collection of data.
References
- WHO Guideline Recommendations on Digital Interventions for Health System Strengthening. Geneva: World Health Organization; 2019. 1, Introduction [cited 2025 Aug 08]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK541905/
- Allison CO, Prucka SK, Fitzgerald-Butt SM, et al. Characterization of adults concerning the use of a hypothetical mHealth application addressing stress-overeating: an online survey. Int J Environ Res Public Health. 2024;8(1):1–11. https://doi.org/10.1371/journal.pone.0309119
- Putteeraj M, Bhungee N, Somanah J, Moty N. Assessing E-Health adoption readiness using diffusion of innovation theory and the role mediated by each adopter’s category in a Mauritian context. Int Health. 2022;14(3):236–49. https://doi.org/10.1093/inthealth/ihab035
- Owoyemi A, Owoyemi J, Osiyemi A, Boyd A. Artificial Intelligence for Healthcare in Africa. Front Digit Health. 2020;2. https://doi.org/10.3389/fdgth.2020.00006
- Bee P, Lovell K, Airnes Z, Pruszynska A. Embedding telephone therapy in statutory mental health services: a qualitative, theory-driven analysis. BMC Psychiatry. 2016;16(1):1–11. https://doi.org/10.1186/s12888-016-0761-5
- Shaarani I, Jounblat M, Jounblat H, Ghanem A, Mansour R, Taleb R. Developing and validating a tool to assess telemedicine acceptance among physicians during pandemic using a technology acceptance model. Telemed e-Health. 2023;29(6):903–11. https://doi.org/10.1089/tmj.2022.0348
- Feroz A, Kadir MM, Saleem S. Health systems readiness for adopting mhealth interventions for addressing non-communicable diseases in low- and middle-income countries: a current debate. Glob Health Action. 2018;11(1). https://doi.org/10.1080/16549716.2018.1496887
- Kim MO, Coiera E, Magrabi F. Problems with health information technology and their effects on care delivery and patient outcomes: a systematic review. J Am Med Informatics Assoc. 2017;24(2):246–260. https://doi.org/10.1093/jamia/ocw154
- Su XV, Sutiman I, Suut SKWM, et al. Perception of primary care doctors towards telemedicine in Kuching, Sarawak: a cross-sectional study. Malays Fam Phys. 2024;19. https://doi.org/10.51866/oa.505
- Sin DYE, Guo X, Yong DWW, et al. Assessment of willingness to Tele-monitoring interventions in patients with type 2 diabetes and/or hypertension in the public primary healthcare setting. BMC Med Inform Decis Mak. 2020;20(1):1–11. https://doi.org/10.1186/s12911-020-1024-4
- Shi J, Guo Y, Yang F, Kulkarni S. Telehealth use and work stress among Chinese health care providers during the COVID-19 pandemic. Decis Mak Anal. 2023;2(1):1–10. https://doi.org/10.55976/dma.2202411881-10
- Ojo JO, Ipinnimo TM, Afolayan AC, et al. Factors associated with willingness to use mHealth interventions for medication adherence among people living with HIV attending a tertiary hospital in sub-Saharan Africa. PLoS One. 2024;19(8). https://doi.org/10.1371/journal.pone.0309119
- Onsongo S, Kamotho C, Rinke De Wit TF, Lowrie K. Experiences on the utility and barriers of telemedicine in healthcare delivery in Kenya. Int J Telemed Appl. 2023;2023. https://doi.org/10.1155/2023/1487245
- Kyei KA, Onajah GN, Daniels J. The emergence of telemedicine in a low-middle-income country: challenges and opportunities. Ecancermedicalscience. 2024;18:1–9. https://doi.org/10.3332/ecancer.2024.1679
- Mensah NK, Adzakpah G, Kissi J, et al. Health professional’s readiness and factors associated with telemedicine implementation and use in selected health facilities in Ghana. Heliyon. 2023;9(3):e14501. https://doi.org/10.1016/j.heliyon.2023.e14501
- Gbolahan O, Kokori E, Osaghae O, Lawal ZD, Olaogun T. Telehealth in Africa: evolution and transformative impact before, during and after COVID-19: a narrative review. J Glob Health Sci. 2023;5(2):1–11. https://doi.org/10.35500/jghs.2023.5.e14
- Stuijt DG, van Doeveren EEM, Kos M, et al. Remote patient monitoring using mobile health technology in cancer care and research: patients’ views and preferences. JCO Clin Cancer Inform. 2024;8. https://doi.org/10.1200/CCI.24.00092
- Schürmann F, Westmattelmann D, Schewe G. Factors influencing telemedicine adoption among health care professionals: qualitative interview study. JMIR Form Res. 2025;9. https://doi.org/10.2196/54777
- Yan M, Sun W, Tan C, Wu Y, Liu Y. Analysis of factors influencing the willingness of chinese older adults to use mHealth Devices: nationwide cross-sectional survey study. J Med Internet Res. 2025;27. https://doi.org/10.2196/66804
- Rouidi M, Elouadi A, Hamdoune A. Acceptance and use of telemedicine technology by health professionals: development of a conceptual model. Digit Health. 2022;8. https://doi.org/10.1177/20552076221081693
- Mensah M. Health professionals’ preference and use of electronic health records in a tertiary care hospital in Ghana: a cross-sectional study. Telehealth and Medicine Today. 10(2). https://doi.org/10.30953/thmt.v10.593
- Knop M, Mueller M, Niehaves B. Investigating the use of telemedicine for digitally mediated delegation in team-based primary care: mixed methods study. J Med Internet Res. 2021;23(8). https://doi.org/10.2196/28151
- Xiong S, Lu H, Peoples N, et al. Digital health interventions for non-communicable disease management in primary health care in low-and middle-income countries. NPJ Digit Med. 2023;6(1). https://doi.org/10.1038/s41746-023-00764-4
- Kung LH, Yan YH, Kung CM. Exploring telemedicine usage intention using technology acceptance model and social capital theory. Healthcare. 2024;12(13):1–9. https://doi.org/10.3390/healthcare12131267
Copyright Ownership: This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See http://creativecommons.org/licenses/by-nc/4.0. The authors of this article own the copyright.