ORIGINAL CLINICAL RESEARCH
Exploring Dentists’ Perceptions and Capacity to Adopt Digital Records and Telediagnostics: A Step Toward AI and Teledentistry Integration in Dental Clinics
Ammar Ahmed Siddiqui, BDS, MDentPH, MFDS RCPSG, FRSPH UK, DDPHRCS Eng1  , Hassan Jan, BDS, MSc2
, Hassan Jan, BDS, MSc2  , Malik Zain Ul Abideen, BDS, MME3
, Malik Zain Ul Abideen, BDS, MME3  , Wajahat Hussain, BDS, M.PHIL4
, Wajahat Hussain, BDS, M.PHIL4  , Yasser Riaz Malik, BDS, M.intl.ph1
, Yasser Riaz Malik, BDS, M.intl.ph1  , Junaid Amin, DPT, MHPE5
, Junaid Amin, DPT, MHPE5  , Aimen Batool, BDS, MDSc6
, Aimen Batool, BDS, MDSc6  and Nashwa Alzaki A. Bushara, BDS, Clinical MD1
and Nashwa Alzaki A. Bushara, BDS, Clinical MD1 
1Department of Preventive Dental Sciences, College of Dentistry, University of Ha’il, Hail, Kingdom of Saudi Arabia; 2Department of Operative Dentistry and Endodontics, Peshawar Medical and Dental College, Peshawar, Pakistan; 3Department of Dental Education and Research, College of Dentistry, Bakhtawar Amin Medical and Dental College, Multan, Pakistan; 4Department of Science of Dental Materials, Multan Medical and Dental College, Multan, Pakistan; 5Department of Physiotherapy, College of Applied Medical Sciences, University of Ha’il, Ha’il, Kingdom of Saudi Arabia; 6Department of Community Dentistry, College of Dentistry, Bakhtawar Amin Medical and Dental College, Multan, Pakistan
Keywords: Artificial intelligence, dentist, electronic dental records, Pakistan, teledentistry, telediagnosis
Abstract
Background: Artificial intelligence (AI), electronic dental records (EDRs) and telediagnostics promise improvements in diagnostic accuracy, workflow efficiency, and access to specialist care. In Pakistan the transition from manual to digital dental practice is constrained by infrastructure, finance, and training gaps. This study explored dentists’ perceptions and capacity to adopt EDRs and telediagnostics in Multan, Pakistan.
Methods: A qualitative exploratory design was used. Semi-structured interviews (26 to 32 min) were conducted in person or via secure virtual platforms, audio-recorded, and transcribed verbatim. Data were analyzed using Braun and Clarke thematic analysis two researchers independently coded transcripts, and member-checking and peer debriefing supported trustworthiness. Reporting follows consolidated criteria for reporting qualitative research (COREQ).
Results: Purposive sampling recruited 15 licensed dentists practicing in Multan (≥ 1 year experience) across private, public, and mixed settings. Participants were aged 25 to 34 years (33.3%), 35 to 44 years (46.7%), and ≥ 45 years (20.0%). Among the dentists, 53.3% were general dentists, 46.7% were consultants, and 53.3% were male. Five themes emerged: (1) “Background and Digital Engagement” (extent of exposure; learning pathways); (2) “Current Practice and Workflow” (hybrid documentation; use of digital imaging/data sharing); (3) “Barriers and Enablers to Adoption” (financial/resource constraints, infrastructural/technical capacity, platform availability); (4) “Perceptions and Preparedness” (anticipated benefits for remote diagnosis; concerns regarding data privacy, reliability; variable practical readiness); and (5) “Recommendations for Policy and Governance” (awareness vs. implementation gap; call for incentives, guidelines, and targeted training). Participants reported pragmatic adoption of imaging and hybrid record-keeping but identified interconnected financial, technical, and governance barriers limiting broader uptake.
Conclusions: Dentists in Multan show early, uneven adoption of digital tools. To enable safe, equitable integration of telediagnostics and AI, policymakers and institutions should prioritize affordable, interoperable EDRs, accredited modular training, technical support, and clear governance mechanisms.
Plain Language Summary
Digital technologies such as artificial intelligence (AI), electronic dental records (EDRs), and telediagnostics have the potential to improve diagnosis, patient management, and access to specialist care. However, in Pakistan, many dental clinics are still transitioning from paper-based to digital systems, facing challenges related to infrastructure, cost, and limited training.
This qualitative study explored how dentists in Multan perceive and use digital dental technologies. Fifteen licensed dentists from private and public clinics participated in 30-minute interviews discussing their experiences, practices, and challenges.
Most participants reported using digital imaging, but many relied on hybrid paper–electronic systems. While dentists acknowledged benefits such as improved efficiency and remote consultations, concerns were raised about financial barriers, unreliable internet connectivity, limited technical support, and data privacy.
Overall, digital adoption is emerging but inconsistent. Expanding affordable systems, structured training, stronger infrastructure, and clear regulatory frameworks are essential to support safe and effective implementation.
Citation: Telehealth and Medicine Today © 2026, 10: 635
DOI: https://doi.org/10.30953/thmt.v10.635
Copyright: © 2026 The Authors. This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, and enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See http://creativecommons.org/licenses/by-nc/4.0. The authors of this article own the copyright.
Submitted: October 10, 2025; Accepted: January 16, 2026; Published: March 26, 2026
Corresponding Author: Junaid Amin, Email: junaid768@hotmail.com
Competing interests and funding: The authors declare that they have no conflicts of interest related to this study.
The authors received no specific funding for this work from any public, commercial, or not-for-profit funding agencies.
The rapid advancement of digital technologies, particularly artificial intelligence (AI), is transforming healthcare systems worldwide. In addition, AI-powered diagnostics, digital record-keeping, and teledentistry are revolutionizing patient care in the dental profession.1 AI-driven imaging systems, automated diagnosis, and machine learning algorithms have enhanced clinical decision-making, improved efficiency, and facilitated remote consultations.2,3 Adoption of digital records and telediagnostics is a crucial step toward integrating AI and optimizing teledentistry practices. Digital records, often referred to as electronic health records (EHRs), are “computer-based dental documentation” that manage patient information, including identification data, clinical notes, treatment plans, and outcomes.4,5 However, telediagnostics, a subset of telemedicine, involves the remote diagnosis of patients through the transmission of clinical data and images to specialists for evaluation.
In the context of dentistry, telediagnostics refers to the remote diagnosis of dental conditions through the transmission of clinical information and images over distances. This approach enables dental professionals to assess patient cases without the need for an in-person visit, facilitating consultations and treatment planning. Telediagnostics is a component of teledentistry, which combines telecommunications and dentistry to improve access to oral healthcare, enhance service delivery, and reduce costs. However, despite these advancements, many developing countries, including Pakistan, face significant challenges in transitioning from traditional manual systems to digital dentistry.6–8
Pakistan’s dental healthcare system largely relies on conventional record-keeping and in-person consultations, which limit the potential benefits of AI and digital technologies. The lack of digital infrastructure, limited financial resources, and insufficient training in emerging dental technologies contribute to this slow transition.9 In cities such as Multan, where dentistry is expanding, understanding capacity among dentists to adopt digital records and telediagnostics is essential to bridging the gap between traditional practices and AI-driven innovations.
By assessing their readiness, willingness, and perceived barriers, this study aims to explore the feasibility of integrating digital solutions in routine dental practice.
Digital records enhance clinical efficiency by streamlining patient information management, reducing errors, and improving continuity of care.10 Likewise, telediagnostics, an essential component of teledentistry, enables remote consultations, which is particularly beneficial for rural and underserved populations with limited access to specialized dental care.4 AI-powered teledentistry can assist in early diagnosis, treatment planning, and remote monitoring, ultimately improving patient outcomes. However, the adoption of these technologies depends on multiple factors, including dentists’ familiarity with digital tools, institutional support, regulatory policies, and infrastructure availability.11
Several studies highlighted the potential for digital dentistry to improve healthcare delivery, yet empirical research on its adoption in Pakistan remains scarce.3 This study is the first of its kind in terms of qualitative research based on digital adoption by dentists working in South Punjab, a region where resource accessibility to urban health services is underdeveloped. In the context of Multan, provided here, there is perspective regarding the concept of digital preparedness in the environment where the barriers of insufficient infrastructure are present alongside the growing interest in global telehealth and AI-based innovations. This study aims to explore the perceptions and capacity of dentists in Multan toward adopting digital records and telediagnostics. The results will help to inform strategies for AI-driven teledentistry integration in Pakistan.
Methodology
This qualitative exploratory study was conducted to assess the capacity of dentists to adopt electronic dental records (EDRs) and telediagnostics in Multan, Pakistan. The study captured dental practitioners’ experiences, attitudes, and contextual constraints in dental practice settings.
Purposive sampling was used to recruit practicing dentists. The population was stratified by age, sex, years of practice, and designation. All dentists have a permanent license from the Pakistan Medical and Dental Counsil (PMandDC), currently practicing in Multan with a minimum of 1 year of clinical experience, and have a willingness to participate.
Dentists not actively engaged in clinical practice, having a provisional PMDC license, and practicing outside Multan were excluded. Recruitment continued until thematic saturation was achieved. Participants were approached through their official contact numbers. A total of 40 dentists were invited to participate. Twenty-seven (67.5% response rate) expressed willingness to participate. Data collection ceased after 15 interviews (saturation was reached at interview,12 and two additional interviews were conducted to confirm saturation).
Data were collected using semi-structured in-depth interviews, developed through an extensive review of the relevant literature and refined with input from subject-matter experts.13 The interview guide (see Appendix) was designed to elicit insights on several core themes: awareness and understanding of digital records, telediagnostics, and teledentistry; current usage and perceived benefits; barriers to adoption such as infrastructural and financial limitations; and expectations regarding the future integration of AI-driven solutions in dental care. Interviews were conducted in settings that assured privacy and comfort, either face-to-face within clinical environments or via secure virtual platforms, with each session lasting between 26 and 32 min. All interviews were audio-recorded with participants’ prior informed consent. Detailed field notes were maintained to capture nonverbal cues and contextual nuances.
Each interview was transcribed verbatim, and the transcripts were subsequently analyzed manually using Braun and Clarke thematic analysis framework.12 Two researchers independently coded the initial five transcripts, compared coding decisions, and reconciled discrepancies through discussion. Throughout analysis, constant comparison, and peer debriefing supported theme development and ensured analytic consistency. Member checking was done to ensure trustworthiness in findings.
Ethical permission was obtained from the institutional review board of Bakhtawar Amin Dental College and Hospital (286/23/COD), and all participants provided written informed consent prior to their involvement.
The study methods and findings are reported in accordance with the Consolidated Criteria for Reporting Qualitative Research (COREQ).14
Results
A total of 15 dentists from Multan participated in this study. The participants represented diverse backgrounds in terms of age, sex, years of experience, and level of expertise. Among the respondents, 5 (33.3%) were aged 25 to 34 years, 7 (46.7%) were aged 35 to 44 years, and 3 (20.0%) were older than 45 years. Eight participants (53.3%) were male and 7 (46.7%) were female. Regarding professional experience, 4 (26.7%) had 2 to 5 years of experience and 5 (33.3%) had 6–10 years. Four (26.7%) had 11 to 15 years, and 2 (13.3%) had more than 15 years of experience. With respect to areas of expertise, eight participants (53.3%) were general dentists, while the remaining seven (46.7%) were consultants with postgraduate clinical qualifications. Table 1 provides a summary of these demographics.
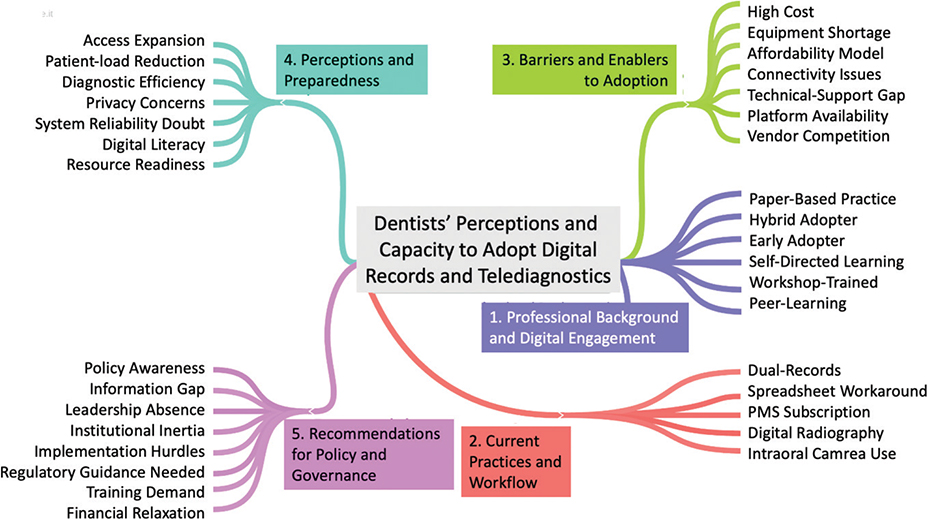
Thematic analysis of interview transcripts generated five broad themes with two to three subthemes that summarize the general views of the dentists about using digital records and telediagnostics in Multan (Figure 1).
Image Credit: Author Malik Zain Ul Abideen with Media element by coggle.it.15
The first theme, “Professional Background and Digital Engagement,” points to differences in practitioners’ exposure to digital versus paper-based record systems. This theme highlights variability in digital experience. Some dentists still follow manual, paper-based protocols, whereas others have begun adopting EDR systems through workshops and self-directed learning.
The second theme, “Current Practices and Workflow,” outlines how documentation and imaging are actually conducted in regular care, with the adoption of hybrid paper and digital record systems as well as increasing use of digital imaging tools in recent years through inexpensive digital X-ray software.
The third theme, “Barriers and Enablers to Adoption,” includes financial and resource barriers and infrastructural and technical capacity barriers that directly limit dentists’ ability to adopt EDRs and telediagnostics. Moreover, features of available digital platforms are making this transition affordable for private clinics.
The fourth theme, “Perceptions and Preparedness,” includes the anticipations of clinicians regarding the utility of remote diagnosis, unresolved fears of data privacy and system stability, and the inconsistent practical maturity of the clinics already equipped with limited digital solutions.
Lastly, “Recommendations for Policy and Governance” consolidate the provision of national efforts by regulators, perceived local and institutional gaps in implementation, and specific solicitation of incentives, clear direction, and focused training to facilitate safe, equitable adoption.
Discussion
This qualitative research explored the perceptions of dentists about implementing digital dental records and telediagnostics in Multan, Pakistan. This study identified five interrelated themes describing Pakistani dentists’ digital engagement and the barriers/enablers to telediagnostic adoption, including (1) professional background and digital engagement; current practice and workflow; (2) barriers and enablers to adoption; (3) perceptions and preparedness; (4) recommendations for policy and governance that reflect that the dental sector is minimally digitalized; and (5) barriers that currently hinder broader adoption.
There are differences in the level of digital engagement for dental record and diagnosis purposes among participants. This mirrors an Indian study (2024) reporting uneven teledentistry awareness that highlighted varied awareness and skills in the use of teledentistry.15 Moreover, a multicentric study conducted in India in 2025 reported that awareness and adoption of digital tools in dental education vary by educational status, gender, and institution.16 This trend indicates that workforce preparedness is disproportionate and that application will not be automatic across all areas where digital tools are available. Instead, adoption occurs along a gradient defined by previous exposure, access to training, and institutional preferences and resources.
The theme “Current Practice and Workflow” highlighted the adaptation of hybrid documentation practices and digital imaging (digital X-rays and intraoral cameras) that is fairly well-established in most practices, but overall, teledentistry services. The findings are consistent with a review published in 2023 that concluded while digital imaging is commonly adopted, comprehensive digital record-keeping systems are less frequently utilized in dental practices.17 This might be due to incurring immediate costs and disruption experienced with completely digitizing systems, especially in resource-constrained settings.
Participants also highlighted enablers and barriers of digital adaptation. The findings underscore that barriers are multifactorial and interdependent. Financial constraints, unreliable connectivity, interoperability concerns, and the uneven availability and affordability of suitable platforms were repeatedly highlighted. This concurs with evidence from low- and middle-income settings where cost, infrastructure, and platform suitability are consistent impediments to teledentistry and EDR adoption.18 However, the developed countries have started to institutionalize teledentistry programs, as reported in a study conducted across 19 countries in 2022.19
The theme “Perceptions and Preparedness” reflected both benefits and limitations of telediagnostics and AI to enhance access (especially to remote patients) and significant concerns about data privacy, clinical boundaries of remote diagnosis, and system stability. The findings are consistent with another study conducted in 2021 that highlighted several constraints related to teledentistry, including lack of government initiatives, compensation strategy, legal issues, technical base, and limitations in telediagnosis.20 Participants focused on practical preparedness, that is, scaled-down, practical systems at hand now, as opposed to aspirational, fully-fledged solutions for step-by-step digital transformation.
On “Policy and Governance,” participants were superficially familiar with the national digital health vision but stated that there was a large gap between on paper and practical implementation. This discrepancy between paper policy and restricted downstream support is not unique and likely explains why national strategies do not always become routine clinical practice. Additionally, the results are consistent with the 2020 study.19 Participants also believed that incentives, explicit regulations, tax exemptions, and structured training and education are practical leverages and can be used by policymakers and professional organizations to speed adoption without compromising the quality and equity. The findings also aligned with a study conducted in 2020 that stated policymakers should address barriers to teledentistry by updating workforce, reimbursement, incentivization, and legal policies.21
The findings highlighted that specific capacity-building initiatives that boost the digital skills of clinicians, institutional policy and implementation plans, and uniform digital record-keeping guidelines are needed from regulators. Some of the measures that can be taken by the government and relevant stakeholders include subsidization of core technologies, enhanced infrastructure, and promotion and facilitation of digital clinics/institutions. These steps will help increase the transformation toward teledentistry and facilitate the implementation of AI-based tools in similar areas.
Strengths
The strengths of the study included purposive sampling for inclusion of different practice types, age groups, designations, and experience levels, resulting in a multi-perspective image of the readiness landscape. The analytic method aggregated closely related concerns (e.g. training as both barrier and enabler) into thematic constructs, which were easier to interpret in the context of policy and practice. Moreover, the findings are consistent with the constructs of the Technology Acceptance Model (e.g. perceived usefulness and perceived ease of use) and Diffusion of Innovation theory (e.g. relative advantage, compatibility, and complexity). Perceived usefulness was revealed by the interest of the participants in streamlined workflows, and the apprehension of training, cost, and disruption of workflow was associated with complexity and compatibility barriers. Such theoretical connections put Multan in a position where this area can be part of the general global trends in the usage of digital technologies through planning and facilitation.
Limitations
The limitations included a sample drawn exclusively from Multan, which limits geographic generalizability across Pakistan’s diverse health systems and urban–rural divides. Self-selection and social desirability might have biased responses toward aspirational statements about technology, and participants might have portrayed greater digital readiness than actually practiced. This was mitigated by ensuring anonymity, emphasizing that there were no right or wrong answers, and reassuring participants that their responses would not affect professional standing. Moreover, this cross-sectional qualitative design captures perceptions at a single point in time. And during recruitment, fewer senior clinicians were available and willing to participate, which reflects the informal impression of a younger practicing workforce in private clinics in Multan. This imbalance might bias the findings toward greater openness to digital technologies, and perspectives of older clinicians are therefore under-represented.
Future multi-site qualitative or mixed-methods studies with larger and more demographically varied samples are needed to examine the transferability of these findings and to better understand how the identified barriers and enablers manifest across different regions.
Conclusions
This study highlights both the opportunities and challenges associated with the adoption of digital records and telediagnostics in dental practice. While the study recognized potential benefits of EDRs and telediagnostics, it also highlighted significant barriers, including limited financial, technological, training, and infrastructure resources. The study also highlighted the transition of most practices into hybrid systems due to the recent entry of market-competitive low-cost digital record and teledentistry platforms. The study also recommended regulator-enforced guidelines, policies, and technological training through infrastructure development and appropriate resource allocation to facilitate effective digital integration in dentistry.
Contributions
Conceptualization: Ammar Ahmed Siddiqui, Junaid Amin; Methodology: Ammar Ahmed Siddiqui, Yasser Riaz Malik; Data Collection: Ammar Ahmed Siddiqui, Hassan Jan; Transcription and Thematic Coding: Hassan Jan; Data Analysis and Interpretation: Ammar Ahmed Siddiqui, Malik Zain Ul Abideen; Literature Review and Manuscript Preparation: Wajahat Hussain, Junaid Amin; Data Validation, Editing, Formatting, and Referencing: Aimen Batool; Critical Revision and Intellectual Input: Yasser Riaz Malik, Junaid Amin, Nashwa Alzaki A. Bushara; Final Approval: All authors.
Data availability Statement (DAS), Data Sharing, Reproducibility, and Data Repositories
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Application of AI-Generated Text or Related Technology
No AI tools were used for data analysis, data interpretation, generation of results, or development of primary scientific conclusions. All intellectual content, study design, analysis, and final decisions regarding manuscript content remain the responsibility of the authors. However, AI-based language support was utilized to improve clarity, grammar, and sentence structure.
References
- Mahesh Batra A, Reche A. A new era of dental care: harnessing artificial intelligence for better diagnosis and treatment. Cureus. 2023;15(11):e49319. https://doi.org/10.7759/cureus.49319
- Yadav P, Asdullah M, Gupta J, Khan MH. Enhancing dental care through artificial intelligence: a comprehensive overview. Int J Oral Health Dent. 2025;9(4):247–50. https://doi.org/10.18231/j.ijohd.2023.047
- Al-Zubaidi SM, Shaikh GM, Malik A, Zain Ul, Abideen M, Tareen J, et al. Exploring faculty preparedness for artificial intelligence-driven dental education: a multicentre study. Cureus. 2024;16(7):e64377. https://doi.org/10.7759/cureus.64377
- Surdu A, Foia CI, Luchian I, Trifan D, Budala DG, Scutariu MM, et al. Telemedicine and digital tools in dentistry: enhancing diagnosis and remote patient care. Medicina (Kaunas). 2025;61(5):826. https://doi.org/10.3390/medicina61050826
- Shah SMM. Harnessing electronic patient records for AI innovation: balancing data privacy and diagnostic advancement. J Khyber Coll Dent. 2024;14(4):1. https://doi.org/10.33279/jkcd.v14i4.843
- Fahim A, Saleem Z, Malik KA, Komal Atta K, Rizwan Mahmood R, Mohammad Khursheed Alam MK, et al. Exploring challenges and mitigation strategies towards practicing teledentistry. BMC Oral Health. 2022;22(1):658. https://doi.org/10.1186/s12903-022-02685-2
- Minervini G, Russo D, Herford AS, Gorassini F, Meto A, D’Amico C, et al. Teledentistry in the management of patients with dental and temporomandibular disorders. Biomed Res Int. 2022;2022:7091153. https://doi.org/10.1155/2022/7091153
- Malpe M, Choudhari SG, Nagtode N, Gharde PM. Beyond the chair: exploring the boundaries of teledentistry. Cureus. 2024;16(6):e62286. https://doi.org/10.7759/cureus.62286
- Rehman AU. Navigating dentistry’s AI revolution: opportunities in Pakistan. J Khyber Coll Dent. 2024;14(1):1. https://doi.org/10.33279/jkcd.v14i01.716
- Pereira KA. Toward enhanced healthcare efficiency: the impact of digitizing medical records. Rev Sist. 2024;14(3):709–14. https://doi.org/10.56238/rcsv14n3-020
- Kaushik R, Rapaka R. A patient-centered perspectives and future directions in AI-powered teledentistry. Discoveries. 2024;12(4):e199. https://doi.org/10.15190/d.2024.18
- Clarke V, Braun V. Thematic analysis. J Posit Psychol. 2017;12(3):297–98. https://doi.org/10.1080/17439760.2016.1262613
- Kallio H, Pietilä A-M, Johnson M, Kangasniemi M. Systematic methodological review: developing a framework for a qualitative semi-structured interview guide. J Adv Nurs. 2016;72(12):2954–65. https://doi.org/10.1111/jan.13031
- Tong A, Sainsbury P, Craig J. Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. Int J Qual HealthCare. 2007;19(6):349–57. https://doi.org/10.1093/intqhc/mzm042
- Professional dentists’ perceptions and capacity to adopt digital records and telediagnostics. [cited 2025 Oct 01]. Available from: https://coggle.it/diagram/Zl1ihenmC-IwWse2/t/dentists%E2%80%99-perceptions-and-capacity-and-telediagnostics
- Sujatha P, Kanitkar AA, Ranjeri S, Annu A, Patil A, Biradar I. Assessment of knowledge and attitude regarding teledentistry among dental professionals: a cross-sectional study. Cureus. 2024;16(3):e55954. https://doi.org/10.7759/cureus.55954
- Dabbiru R, Pakk S, Chintada V, Chintada VR, Kumar M, Kumar S, et al. Knowledge, awareness and attitude of pre-practitioners, interns, post-graduates and dental educators towards the digitalization of OPD in dental schools: a multi-centric questionnaire based study. Bull Stomatol Maxillofac Surg. 2025;21(2): 146–55. https://doi.org/10.58240/1829006X-2025.2-146
- Lelyana N. Strategic analysis in the application of digital technology in dental practice. J Soc Interact Humanit. 2023;2(3):253–74. https://doi.org/10.55927/jsih.v2i3.6441
- Hui CY, Abdulla A, Ahmed Z, Goel H, Habib GMM, Hock TT, et al. RESPIRE Group. Mapping national information and communication technology (ICT) infrastructure to the requirements of potential digital health interventions in low- and middle-income countries. J Glob Health. 2022;12:04094. https://doi.org/10.7189/jogh.12.04094
- El Tantawi M, Lam WYH, Giraudeau N, Virtanen JI, Matanhire C, Chifamba T, et al. Teledentistry from research to practice: a tale of nineteen countries. Front Oral Health. 2023;4:1188557. https://doi.org/10.3389/froh.2023.1188557
- Shuborna NS, Islam SS, Jahan SS, Apu EH, Noor OB. Teledentistry: limitations and challenges. Update Dent Coll J. 2021;11(2):1–3. https://doi.org/10.3329/updcj.v11i2.56045
- DentaQuest Partnership for Oral Health Advancement. Fast-track to teledentistry: removing barriers to care while maximizing overall health. Boston, MA: DentaQuest Partnership for Oral Health Advancement; 2020. https://doi.org/10.35565/DQP.2020.2010
Copyright Ownership: This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, and enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See http://creativecommons.org/licenses/by-nc/4.0. The authors of this article own the copyright.
Addendum
Interview Guide
Can you briefly describe your experience in dental practice and your familiarity with digital records and telediagnostics?
How do you currently document patient records, including diagnoses and treatment plans? What digital tools (e.g. computers, smartphones) do you use in this process?
How do you utilize imaging tools (such as X-rays or intraoral cameras) in your clinic, and how is diagnostic data shared with specialists?
What are the primary obstacles you face or anticipate facing in adopting digital records and telediagnostics?
What type of training or support would help you more effectively integrate digital tools and prepare for the future use of AI-driven diagnostics and teledentistry in your practice?
How do you envision the role of EDRs and telediagnostics in enhancing dental care, particularly in relation to diagnosis and treatment planning for remote patients? What potential benefits or concerns do you associate with its implementation?
Are you aware of any national policies (for example, Pakistan’s Digital Health Vision) that promote digital healthcare? How do you feel these policies impact your practice, and what policy changes or support mechanisms would you recommend to facilitate broader digital adoption?
-
Is there anything else you would like to share about your experience with or concerns about the adoption of digital records and telediagnostics?