ORIGINAL RESEARCH
Assessing Patient Satisfaction and Exploring Technical, Social, Individual Barriers of Using Mental Telehealth Services
Amani F. Alharthy, DrPH, MPH  ; Noura M. Alabdullah, BS
; Noura M. Alabdullah, BS  ; Raghad A. Alfulaij, BS
; Raghad A. Alfulaij, BS  ; Ghaida M. Alotaibi, BS
; Ghaida M. Alotaibi, BS  ; Nadin M. Alghamdi, BS
; Nadin M. Alghamdi, BS 
Department of Health Sciences, College of Health and Rehabilitation Sciences, Princess Nourah bint Abdulrahman University, Riyadh, Saudi Arabia
Keywords: Individual barriers, mental telehealth, patient satisfaction, social barriers, technical barriers
Abstract
Background: Telehealth services in Saudi Arabia have expanded under Vision 2030* to help enhance health access through digital platforms. However, limited research has explored barriers to access and satisfaction with mental telehealth services. This study aimed to identify the barriers that hinder access to mental telehealth services and assess patient satisfaction among the users.
Methods: A cross-sectional study was conducted among adults in Riyadh, Saudi Arabia, from September 2024 through April 2025. Statistical significance was p < 0.05.
Results: A total of 437 participants registered, of whom 69% were young adults aged 18 to 29 years, and 63% were females. Mental telehealth was used by 31%, of whom Labayh (an electronic platform specialized in psychological and family sessions) (69%) was the most utilized platform. Patient satisfaction was high at 92%. Technical problems, such as difficulty using apps and the need for technical assistance, were significantly higher among non-users compared to users (p < 0.001). The non-users of mental telehealth service providers reported higher perceived support from family and friends (p < 0.001). Personal barriers like professional qualification issues, privacy issues, and shame discussing personal issues via the internet were the strongest predictors of non-use (p < 0.001).
Conclusion: The findings highlight the fact that although patient satisfaction with Riyadh’s mental telehealth care is high, utilization is still influenced by individual, social, and technical barriers. Psychological issues needing resolution include social support facilitation, electronic literacy enhancement, and user-friendly sites ensuring facilitation, which are crucial in improving engagement and usability.
Plain Language Summary
In Saudi Arabia, telehealth has expanded as part of Vision 2030* to make healthcare more accessible through digital tools. While many people now use telehealth for general medical care, less is known about how people use telehealth for mental health support and what challenges they face. This study looked at the barriers that prevent people from using mental telehealth services and assessed how satisfied users are with these services. Adults living in Riyadh between September 2024 and April 2025 participated by using an online questionnaire. A total of 437 people completed the survey. Most were young adults aged 18 to 29 years. Only about one-third had used mental telehealth services, with Labayh (an electronic platform specialized in psychological and family sessions) being the most commonly used. Among the users, satisfaction was high (92%). However, people who had never used mental telehealth experienced more technical difficulties, such as apps being hard to use or needing technical assistance. They also reported receiving more support from family and friends, which might reduce the need for online mental health help. Personal concerns—such as privacy worries, doubts about professional qualifications, and discomfort discussing personal issues online—were the strongest barriers to use. Overall, even though users are highly satisfied with mental telehealth in Riyadh, several barriers prevent wider use. Improving digital skills, ensuring privacy, providing culturally sensitive support, and designing easier-to-use platforms may help more people access mental healthcare online.
*Vision 2030 emphasizes the advancement of digital health services, including mental health services in Saudi Arabia.
Citation: Telehealth and Medicine Today © 2025, 10: 653
DOI: https://doi.org/10.30953/thmt.v10.653
Copyright: © 2025 The Authors. This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See http://creativecommons.org/licenses/by-nc/4.0. The authors of this article own the copyright.
Submitted: November 19, 2025; Accepted: January 21, 2026; Published: February 14, 2026
Corresponding Author: Amani Alharthy, Email: Afalharthy@pnu.edu.sa
Competing interests and funding: None.
None.
Mental health disorders are a major global public health concern that afflict more than 1 billion individuals with high morbidity and mortality worldwide.1,2 In Saudi Arabia, the National Mental Health Survey estimates that 34.2% of the population has been diagnosed with various mental health issues.3 Despite this considerable prevalence, access to mental healthcare is still impeded by continued stigma, inadequate awareness, cultural beliefs, and the lack of specialist services,4 which emphasize the need for innovative strategies to enhance the accessibility and provision of mental healthcare.
In response to these challenges, Saudi Arabia has prioritized digital health transformation under Vision 2030*, which explicitly emphasizes the expansion of telehealth services to improve healthcare accessibility, efficiency, and equity across the Kingdom.5 As part of this national strategy, mental telehealth services have been increasingly integrated into the healthcare system to overcome geographical, social, and systemic barriers to care.
Although previous studies in Saudi Arabia generally report high satisfaction with mental telehealth services based on their convenience and easy access,6–8 persistent cultural, privacy, and gender-related concerns among female patients restrict full engagement and comfort with the platforms.9,10 These findings indicate a critical necessity for further investigation of the barriers to correct utilization of mental telehealth services.
To address these gaps, this study investigates the technical, social, and personal obstacles influencing the use of mental telehealth services and patient satisfaction among Riyadh adults in Saudi Arabia. To enhance mental telehealth provision and utilization, culturally sensitive service delivery, and guide public health policy sensitive to national digital health ambitions, it is important to understand these determinants
Methods
Study Design and Setting
A cross-sectional descriptive quantitative study was conducted in Riyadh, Saudi Arabia, between September 2024 and April 2025. Riyadh was selected as the area of study due to its large and diverse population and the widespread availability of digital healthcare through public as well as private platforms. The setting provided a reasonable background to analyze the use of mental telehealth services and the determinants influencing their utilization.
Study Population and Sampling Method
The study was undertaken with adults aged 18 years and older living in Riyadh—both Saudi and non-Saudi residents. Those older than 65 years were excluded to limit potential bias due to age-related issues such as cognitive impairments and lower digital literacy. The required sample size was calculated at 372 participants at a confidence level of 95%, a margin of error of 5%, and an estimated prevalence of mental telehealth utilization using data from previous local studies. Ultimately, the final sample size comprised 437 study participants to have adequate power in the study and account for the non-response rate.
Non-probability sampling was used involving convenience sampling and the snowball sampling technique. The link to the survey was initially circulated through social media pages, university networks, and community groups, and it was encouraged that the link be passed on amongst one’s personal and professional connections to spread a wider net. This hybrid strategy was used to reach a broad demographic sample in Riyadh without compromising the practicability and efficiency of data collection.
Questionnaire Development and Validation
The questionnaire was developed following a thorough review of the literature and tailored to be compatible with Riyadh’s population’s sociocultural life. The questionnaire was divided into three main sections. The first section was designed to collect demographic information such as participants’ gender, age, marital status, level of education, geographic area, and number of family members living in a household.
The second section of the questionnaire encompassed barriers to the use of mental telehealth services, which were further classified into technical, social, and individual barriers. For example, the technical barriers included challenges such as lack of good internet connection, poor technical support, and poor digital infrastructure. On the other hand, the social barriers included stigma for mental health issues, cultural beliefs and norms, and societal attitudes that might discourage people from making use of mental telehealth services. Individual barriers assessed factors such as age, education, digital literacy, and socioeconomic status that might influence comfort and familiarity with digital channels.
The third section assessed patient satisfaction and was administered to only those participants who were previously users of mental telehealth services. This section assessed participants’ satisfaction with the availability, convenience, responsiveness, and general quality of mental telehealth services.
A pilot study was conducted between June and July 2024, approximately two to three months prior to the main data collection period, to assess the clarity, appropriateness, completeness, and cultural sensitivity of the questionnaire items. The pilot was administered to a group of adult Riyadh residents who met the same inclusion criteria as the main study population, ensuring that feedback reflected the perspectives of the target population rather than expert opinion alone. Participants in the pilot study provided feedback on item wording, question flow, comprehension, and sensitivity of mental health–related content. Based on this feedback, minor refinements were made to improve clarity and cultural relevance. Participants in the pilot study were not re-enrolled in the main study to avoid duplicate participation. In addition, the pilot survey link was closed prior to launching the final questionnaire, and the main survey was disseminated independently through separate distribution channels. The wording of some items was refined utilizing the feedback from the members of the pilot group. Cronbach’s alpha coefficient was used to perform reliability testing and demonstrated good internal consistency for all the domains. The Cronbach’s alpha of over 0.70 was achieved for individual, technical, and patient satisfaction domains. The social barriers framework also achieved an acceptable reliability (α > 0.70) after removing one item. “There is a stigma attached to receiving mental telehealth services in my community.”
Mental Telehealth Services Use (Ever Use)
The classification of mental telehealth service users and non-users was based on participants’ self-reported current or prior use of mental telehealth services. During data collection, participants were asked a direct questionnaire item inquiring whether they had ever used mental telehealth services for mental health–related care. Participants who responded “Yes” were classified as users, while those who responded “No” were classified as non-users. No minimum number of sessions, duration of use, or frequency threshold were applied; therefore, any prior use (at least once) of mental telehealth services was sufficient for classification as a user. Participants who reported never having used mental telehealth services at any time were classified as non-users. This operational definition was applied consistently throughout the analysis to compare utilization patterns, perceived barriers, and satisfaction outcomes between the two groups.
Data Collection Procedure
Data were collected using an online, self-administered questionnaire distributed to adult residents of Riyadh. The main data collection phase was conducted between September 2024 and April 2025 using a secure web-based survey platform designed to ensure participant anonymity and data protection. Participants who completed the pilot study were not eligible to participate in the main survey. To prevent duplicate participation, the pilot survey was closed prior to launching the final questionnaire, and the main survey link was distributed independently after completion of the pilot phase.
The survey link was disseminated through multiple channels, including social media platforms (Twitter, WhatsApp, and Telegram), university email lists, and community networks, to reach a diverse adult population. Each invitation included an introductory message outlining the study objectives, eligibility criteria, voluntary participation, confidentiality assurances, and informed consent procedures. Only participants who provided electronic consent could access the questionnaire.
The questionnaire was optimized for web browsers and mobile devices (smartphones and tablets) using responsive design principles. User-friendly features included clear sectioning of questions, logical sequencing, adequate white space to reduce visual fatigue, simple navigation with forward and backward movement between pages, and automatic saving of responses during completion to minimize data loss. These design features were intended to enhance usability across devices and improve completion rates.
Survey completion was conducted using an asynchronous approach, allowing participants to complete the questionnaire at their convenience. Responses were saved automatically by the survey platform during active completion; however, incomplete surveys that were exited prior to submission were not stored as finalized entries. Participants were encouraged to complete the questionnaire in one session, which typically required 20 to 30 minutes. The survey was designed for self-completion, though participants were not restricted from seeking general assistance (e.g., clarification of wording) if needed. No real-time supervision was required, and self-completion was not used as an exclusion criterion.
To address participant support, contact information for the research team was provided in the survey introduction, allowing respondents to seek clarification regarding study-related questions if necessary. No technical or content-related inquiries requiring intervention were reported during the data collection period. To prevent multiple submissions by the same individual, the survey platform was configured to limit responses to one submission per device and browser session, and duplicate entries were screened during data cleaning based on response patterns and completion timestamps. All submitted responses were automatically recorded and stored in an encrypted database accessible only to the principal investigator and authorized research team members. No identifying or personal information (e.g., names, email addresses, IP addresses, or phone numbers) was collected, ensuring full anonymity of participants.
Vision 2030 emphasizes the advancement of digital health services, including mental health services in Saudi Arabia.
Statistical Analysis
Descriptive statistics, including frequencies, percentages, means, and standard deviations (if applicable) were utilized to delineate demographic data and key study variables. Bivariate examination, including the chi-square test, was applied to identify correlations between dichotomous variables. A p-value less than 0.05 was considered statistically significant. Data were examined using the Statistical Package for the Social Sciences (SPSS, version 26.0).
Ethical Considerations
Ethical approval of the study was obtained from the Princess Nourah Bint AbdulRahman University Institutional Review Board (IRB Log No. 24-0930). The study complied with the ethical guidelines of the Declaration of Helsinki on human subject research. Study participation was voluntary, and no incentives were given. Prior to accessing the online survey, all respondents reviewed an electronic informed consent form that defined study objectives, procedures, possible benefits, and the right to withdraw at any time without penalty. Confidentiality and anonymity were strictly maintained during the study. No identifying data were collected, and data were stored safely on passworded computers accessible only to the research team. The data gathered were used solely for research purposes and were represented at the aggregated level to ensure participant confidentiality.
Results
Demographic Features of Participants
The demographic details of the 437 study participants are listed in Table 1. The majority were young adults aged 18% to 29% (69%), predominantly female (63%), and the majority were single (67%). Nearly 65% had a bachelor’s degree, and 5% had postgraduate studies. Family size was generally medium, as 58% of the sample reported five to nine members in the family, and monthly household income predominantly ranged from 5,000 to 20,000 Saudi Riyals (3.4 SAR = 1 USD = 0.76 EU) (approximately 62%). Most participants were Saudi nationals (95%), residing in Riyadh in general, although the greatest proportion was from the northern (29%) and eastern (23%) regions of Riyadh. Only 31% of the participants reported previous experience with mental telehealth services, as shown in Appendix A.
| Technical barriers | Response | Non-users n (%) | Users n (%) | Total n (%) | Chi-square | P-value |
| Unexpected breakdowns hinder the use of mental telehealth care apps. | Agree | 177 (40.50) | 80 (18.31) | 257 (58.81) | 22.88 | p < 0.0001* |
| Neutral | 84 (19.22) | 15 (3.43) | 99 (22.65) | |||
| Disagree | 42 (9.61) | 39 (8.92) | 81 (18.54) | |||
| Using mental telehealth apps is complicated. | Agree | 91 (20.82) | 26 (5.95) | 117 (26.77) | 31.30 | p < 0.0001* |
| Neutral | 90 (20.59) | 16 (3.66) | 106 (24.26) | |||
| Disagree | 122 (27.92) | 92 (21.05) | 214 (48.97) | |||
| Using mental telehealth services is more expensive than traditional in-person visits. | Agree | 73 (16.70) | 40 (9.15) | 113 (25.86) | 8.07 | p = 0.0177* |
| Neutral | 91 (20.82) | 23 (5.26) | 114 (26.09) | |||
| Disagree | 139 (31.81) | 71 (16.25) | 210 (48.05) | |||
| There is a need for technical support for me to use mental telehealth apps. | Agree | 139 (31.81) | 42 (9.61) | 181 (41.42) | 30.49 | p < 0.0001* |
| Neutral | 93 (21.28) | 25 (5.72) | 118 (27.00) | |||
| Disagree | 71 (16.25) | 67 (15.33) | 138 (31.58) | |||
| It is difficult to use mental telehealth care apps. | Agree | 72 (16.48) | 21 (4.81) | 93 (21.28) | 33.77 | p < 0.0001* |
| Neutral | 87 (19.91) | 11 (2.52) | 98 (22.43) | |||
| Disagree | 144 (32.95) | 102 (23.34) | 246 (56.29) | |||
| I find that slow or unstable internet in my area can reduce my willingness to use mental telehealth care apps. | Agree | 144 (32.95) | 57 (13.04) | 201 (46.00) | 4.92 | p = 0.0853 |
| Neutral | 73 (16.70) | 25 (5.72) | 98 (22.43) | |||
| Disagree | 86 (19.68) | 52 (11.90) | 138 (31.58) | |||
| I feel that a lack of technical skills may hinder my ability to access mental telehealth care services. | Agree | 111 (25.40) | 37 (8.47) | 148 (33.87) | 18.44 | p < 0.0001* |
| Neutral | 76 (17.39) | 17 (3.89) | 93 (21.28) | |||
| Disagree | 116 (26.54) | 80 (18.31) | 196 (44.85) | |||
| I believe that mental telehealth care apps are easy to use. | Agree | 192 (43.94) | 123 (28.15) | 315 (72.08) | 37.64 | p < 0.0001* |
| Neutral | 76 (17.39) | 6 (1.37) | 82 (18.76) | |||
| Disagree | 35 (8.01) | 5 (1.14) | 40 (9.15) | |||
| *p < 0.05: statistically significant findings. | ||||||
Mental Telehealth Services App Use
As shown in Figure 1, pattern analysis of app usage revealed a strong preference for the Labayh platform, with 69% of total usage among the studied population. Qareboon followed at 16%, while Estenah and Sanar trailed at 10% and 5%, respectively.
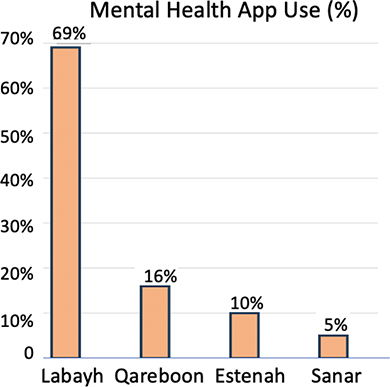
Fig. 1. Distribution of mental telehealth application usage among users (n = 136).
Patient Satisfaction with Mental Telehealth Services
As seen in Figure 2, the findings had a high overall level of patient satisfaction with mental telehealth care among consumers. Specifically, 92% of the survey respondents reported high satisfaction, which suggests that the majority found them useful, accessible, and convenient for their mental health needs. A total of 6% reported moderate satisfaction, consistent with having minor issues or unmet expectations, and just 2% reported low satisfaction levels.
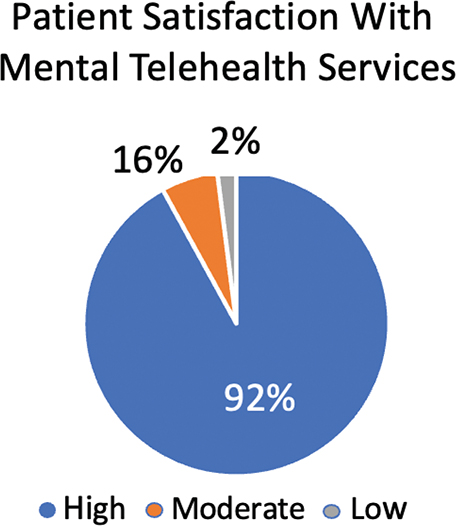
Fig. 2. Proportion of patients satisfied with mental telehealth services among users in study participants (n = 136).
Technical Barriers Strongly Discriminate Users and Non-Users
Findings of the technical barrier analysis revealed a significant difference between users and non-users of mental telehealth care on almost all items (Table 2). Non-users always reported higher technical barriers compared to users. Higher percentages of non-users strongly agreed that technical issues, such as unexpected malfunctioning, were a barrier to use (40.5%) as compared to the users (18.1%) (p < 0.001). Similarly, non-users were substantially more likely to agree that it is difficult to use the apps (20.82% vs. 5.95%), that they require technical support (31.81% vs. 9.61%), that they lack technical knowledge (25.40% vs. 8.47%), and that the apps are time-consuming to use (16.48% vs. 4.81%) (all p < 0.001). Cost was also a considerably greater concern among non-users (16.70% agreeing it is more expensive) than among users (9.15%) (p = 0.0177).
| Social barriers | Response | Non-users n (%) | Users n (%) | Total n (%) | Chi-square | P-value |
| My family supports me if I use mental telehealth services. | Agree | 151 (34.55) | 91 (20.82) | 242 (55.38) | 17.26 | p < 0.0002* |
| Neutral | 99 (22.65) | 19 (4.35) | 118 (27.00) | |||
| Disagree | 53 (12.13) | 24 (5.49) | 77 (17.62) | |||
| My friends are supportive of my use of mental telehealth services. | Agree | 172 (39.36) | 106 (24.26) | 278 (63.62) | 20.692 | p < 0.0001* |
| Neutral | 92 (21.05) | 17 (3.89) | 109 (24.94) | |||
| Disagree | 39 (8.92) | 11 (2.52) | 50 (11.44) | |||
| *p < 0.05: statistically significant findings. | ||||||
The only obstacle that did not attain the significance level was fear of slow or unstable internet (p < 0.0853). However, for a question of whether the apps are easy to use, the respondents were totally in agreement, demonstrating an extremely strong inverse correlation with the perceived ease of the apps by the non-users (p < 0.001), as shown in Table 1.
Social Barriers Between Users and Non-Users
Support from family and friends showed a significant difference between non-users and users of mental telehealth services, as shown in Table 2. A much larger percentage of non-users reported that their family will support them if they use mental telehealth services (151, 34.55%) compared to users (91, 20.82%) (p = 0.0002). Similarly, in friend support, non-users reported that their friends are more supportive (172, 39.36%) than users (106, 24.26%) (p < 0.0001).
Individual Barriers between Users and Non-Users
Individual barrier analysis revealed a significant (p < 0.001) difference between users and non-users on most of the items, while non-users in all cases reported higher agreement to barrier statements (Table 2). Specifically, non-users were considerably more concerned about the professionalism of mental health professionals on websites (40.50% vs. 13.50% for users), security for personal information (36.38% vs. 11.67% for users), and discomfort in discussing personal issues at a distance (36.61% vs. 10.76% for users).
Further, a greater percentage of non-users reported that mental telehealth services were not effective (33.41% vs. 8.01% of users), would not find them useful (22.88% vs. 7.09% of users), and would find the service uncomfortable (32.95% vs. 10.53% of users). The inability to meet basic technological requirements was also a much greater barrier for non-users (30.21% vs. 7.78% of users). All except for the statement between knowledge and usage (“If I have knowledge about mental telehealth services, I will use them”) did not show statistical significance of difference (p = 0.184), even with a large majority agreeing, as can be seen from Table 3.
| Individual barriers | Response | Non-users n (%) | Users n (%) | Total n (%) | Chi-square | P-value |
| Mental telehealth services are not effective for psychological needs. | Agree | 146 (33.41) | 35 (8.01) | 181 (41.42) | 56.94 | p < 0.0001* |
| Neutral | 97 (22.20) | 24 (5.49) | 121 (27.69) | |||
| Disagree | 60 (13.73) | 75 (17.16) | 135 (30.89) | |||
| There is difficulty in meeting the basic technological requirements to use mental telehealth services. | Agree | 132 (30.21) | 34 (7.78) | 166 (37.99) | 45.56 | p < 0.0001* |
| Neutral | 90 (20.59) | 19 (4.35) | 109 (24.94) | |||
| Disagree | 81 (18.54) | 81 (18.54) | 162 (37.07) | |||
| It can be uncomfortable (stressful/anxiety/embarrassing) to use mental telehealth care apps. | Agree | 144 (32.95) | 46 (10.53) | 190 (43.48) | 32.93 | p < 0.0001* |
| Neutral | 71 (16.25) | 12 (2.75) | 83 (18.99) | |||
| Disagree | 88 (20.14) | 76 (17.39) | 164 (37.53) | |||
| There are concerns about the security of personal information when using mental telehealth care apps. | Agree | 159 (36.38) | 51 (11.67) | 210 (48.05) | 26.96 | p < 0.0001* |
| Neutral | 70 (16.02) | 17 (3.89) | 87 (19.91) | |||
| Disagree | 74 (16.93) | 66 (15.10) | 140 (32.04) | |||
| There are concerns about the qualifications of mental health professionals on digital remote platforms. | Agree | 177 (40.50) | 59 (13.50) | 236 (54.00) | 40.42 | p < 0.0001* |
| Neutral | 75 (17.16) | 15 (3.43) | 90 (20.59) | |||
| Disagree | 51 (11.67) | 60 (13.73) | 111 (25.40) | |||
| I have the ability to identify sources of mental telehealth care. | Agree | 161 (36.84) | 92 (21.05) | 253 (57.89) | 9.19 | p < 0.0101* |
| Neutral | 86 (19.68) | 25 (5.72) | 111 (25.40) | |||
| Disagree | 56 (12.81) | 17 (3.89) | 73 (16.70) | |||
| Using mental telehealth services will not be helpful. | Agree | 100 (22.88) | 31 (7.09) | 131 (29.98) | 33.32 | p < 0.0001* |
| Neutral | 86 (19.68) | 13 (2.97) | 99 (22.65) | |||
| Disagree | 117 (26.77) | 90 (20.59) | 207 (47.37) | |||
| There is discomfort in discussing personal issues with a mental health provider through a digital platform (remotely). | Agree | 160 (36.61) | 47 (10.76) | 207 (47.37) | 41.71 | p < 0.0001* |
| Neutral | 72 (16.48) | 14 (3.20) | 86 (19.68) | |||
| Disagree | 71 (16.25) | 73 (16.70) | 144 (32.95) | |||
| If I have knowledge about mental telehealth services, I will use them. | Agree | 218 (49.89) | 107 (24.49) | 325 (74.37) | 3.38 | p = 0.184 |
| Neutral | 62 (14.19) | 18 (4.12) | 80 (18.31) | |||
| Disagree | 23 (5.26) | 9 (2.06) | 32 (7.32) | |||
| *p < 0.05: statistically significant findings. | ||||||
Discussion
This study provides valuable insights into barriers to the use of mental telehealth services in Riyadh and identifies the individual, social, and technical obstacles. Results indicated that the individual predictors showed the highest predictability in service use. Non-users reported greater concerns about professional qualifications, privacy, being embarrassed to discuss personal issues online, and the effectiveness of mental telehealth. These results reflect that personal attitudes and beliefs concerning online mental health services are critical factors in determining utilization. Individuals may believe that virtual consultations are less confidential or less effective than conventional face-to-face appointments and thus might not be ready to use these services. Prior research studies also highlighted the fact that professional competence and privacy issues can significantly hinder utility of telehealth services, particularly in settings of generalized stigma for mental health disorders.11–13
Social support from family and friends had a complex association with the utilization of mental telehealth. Contrary to expectations, significantly more non-users reported that their family would be supportive to them in the event they engaged in mental telehealth services. Similarly, more non-users also indicated that friends would support them. These findings show that there is social support in place, but non-users might not use mental telehealth services due to other salient issues such as privacy, effectiveness, or lack of comfort with digital technology. This highlights the fact that positive social networks alone may not be sufficient to guarantee use and calls for the necessity of breaking through personal and attitudinal barriers as well as establishing social support.
Technical barriers, including app complexity and demands for technical support, were associated with lowered use among non-users. Several participants described limited digital capacity, which can restrict them from being able to use mental health apps effectively. Contrary to expectations, concerns about slow or unreliable internet did not significantly affect use in this study. This may reflect the relatively high internet penetration and infrastructure maturity of Riyadh, and it is possible to conclude that technology is less likely to be a hindrance among city residents than among rural residents.7,14–16 The positive relationship between ease of use and service adoption underlines the importance of an easy-to-use design. Easy-to-use, intuitive interfaces can reduce anxiety and encourage frequent use, supporting previous research showing that perceived ease of use has a significant influence on willingness to adopt telehealth services.14,17,18
Overall, the findings emphasize the need for targeted interventions for improved digital literacy, building supportive social contexts, reducing stigma, and building confidence in mental healthcare. Streamlining easy-to-use applications and accessible technical support may enhance take-up and satisfaction. In addition, attitudes and beliefs at an individual level need to be tackled while building ways to encourage mental telehealth service use.11
Strengths and Limitations
This study has several significant strengths that contribute to a greater comprehension of individual attitudes, barriers, and patient satisfaction with mental telehealth in Riyadh. To begin with, it addresses an important research gap, particularly in the field of mental telehealth, which is a comparatively new area in Saudi Arabia, and offers valuable information that can be applied to inform service improvement and policy development.
Mental telehealth service users and non-users are included so that the full picture of barriers to adoption is understood. By surveying user-perceived barriers and actual barriers faced by users, this study provides a broader understanding of the determinants of utilization. Second, satisfaction data were obtained only from respondents who had accessed mental telehealth services. This focus on actual users ensures that findings are representative of real service experiences and minimizes bias that could arise from hypothetical satisfaction ratings among non-users.
Third, the study utilized established data collection instruments with high reliability, maximizing the consistency and credibility of the findings and supporting the rigor of the conclusions drawn.
Despite these strengths, several limitations should be considered when interpreting the findings. The use of convenience and snowball sampling might reduce generalizability, as the sample might not fully represent the entire population of mental telehealth users in Riyadh, and the statistical power to detect more subtle relationships might be limited. Additionally, the cross-sectional design does not allow for causal inference or for assessment of changes in barriers and satisfaction over time. Because this was a cross-sectional descriptive study rather than a randomized trial, the user and non-user groups cannot be assumed to be comparable, and no causal or matched comparisons between groups can be made. Furthermore, individuals aged 65 years and older were not represented in the study, limiting the ability to assess barriers particularly relevant to older adults, such as cognitive impairment, age-related digital literacy challenges, and usability concerns associated with telehealth platforms. This population may experience distinct obstacles to mental telehealth adoption that were not captured in the current analysis.
The survey was distributed exclusively through electronic channels, which may have limited participation among individuals with low digital literacy or infrequent use of digital platforms, introducing potential selection bias. In addition, most participants were female, which is higher than typically reported in other studies. This imbalance might influence the findings and limit the generalizability of the results to male populations. Although efforts were made to achieve a balance between both sexes, approximately one-third of participants were male, which may influence findings related to gender-based perceptions of telehealth services. While family support appeared more relevant among non-users, most participants were single individuals, which may have influenced this finding; differences in family support should therefore be interpreted cautiously.
In addition, not all participants had utilized mental telehealth services; therefore, responses from non-users reflect perceived rather than experienced barriers, which may differ after actual use. Moreover, the results for satisfaction and barrier analyses are limited to the participants who reported prior use of mental telehealth services and therefore may not be generalizable to the broader population of non-users. The low proportion of non-Saudi participants further limits the generalizability of the findings to expatriate populations in Riyadh. Additionally, the study was conducted exclusively in Riyadh city, which, while large and diverse, may limit the generalizability of the findings to other regions of Saudi Arabia. Other cities or rural areas may differ in terms of digital health infrastructure, cultural attitudes, and mental health service availability, potentially influencing both utilization and satisfaction with mental telehealth services.
Future studies should include multiple regions to capture a more representative national perspective. Future research should consider longitudinal or case–control designs to compare users and non-users more directly and to examine how satisfaction and barriers evolve over time. Moreover, including older adults and more diverse demographic groups in terms of gender and nationality would enhance representativeness and provide a more comprehensive understanding of mental telehealth utilization determinants. Despite these limitations, the study offers a strong foundation for understanding key factors influencing engagement and satisfaction with mental telehealth services and provides actionable evidence to support improvements in accessibility, usability, and patient-centered digital mental healthcare in Riyadh City.
Conclusion
This study provides significant data on adults’ use of mental telehealth services in Riyadh, alongside patient satisfaction at high levels and continuing obstacles to service utilization. Most participants who used mental telehealth were very satisfied, indicating that the services are perceived overall as being effective, accessible, and convenient. Yet a number of challenges—individual, social, and technical difficulties—still limit broader utilization. Individual beliefs and preferences, such as privacy, efficacy, and discomfort with computer technology, were the strongest predictors of non-use. Social support from families and friends was also a strong predictor of service use. Technical barriers were associated with use, but issues like internet unreliability were not statistically significant, suggesting that infrastructural barriers might be context dependent. In general, the findings underscore the fact that enhancing digital literacy, establishing trust, reducing stigma, and simplifying applications and technical assistance are areas of priority for facilitating improved accessibility and utilization of mental telehealth services in Riyadh.
Implications and Future Directions
The findings have several implications for the Saudi Arabian context, particularly in light of Vision 2030, which emphasizes the advancement of digital health services, including mental health services. Overcoming individual and societal stigma can facilitate the mainstreaming of service use for mental health and promote equal access to diverse populations. Interventions such as community awareness, training on digital literacy enhancement, and culturally tailored messaging have the potential to enhance acceptance and use. Policymakers and service providers must make it a priority to develop user-friendly platforms and offer technical support to minimize usability challenges. Future studies would examine longitudinal patterns of use of mental telehealth, evaluate interventions to reduce psychological and social barriers, and involve more diverse populations to learn from underrepresented groups like males and non-Saudi residents. Comparative investigations among users and non-users could also illuminate causal mechanisms and inform directed strategies to maximally provide mental telehealth services across Saudi Arabia.
Contributions
Conceptualization: Amani F. Alharthy: methodology, Noura Alabdullah, Raghad Alfulaij, Ghaida Alotaibi, Nadin Alghamdi: formal analysis, data curation, and investigation, Noura Alabdullah, Raghad Alfulaij, Ghaida Alotaibi, Nadin Alghamdi: writing—original draft preparation, Noura Alabdullah, Raghad Alfulaij, Ghaida Alotaibi, Nadin Alghamdi: writing—review and editing: Amani Alharthy supervision. All authors read and agreed to the published version of the manuscript.
Data Availability Statement (DAS), Data Sharing, Reproducibility, and Data Repositories
The data supporting the findings of this study are available within the article.
Application of AI-Generated Text or Related Technology
None.
Acknowledgments
None.
References
- GBD 2019 Mental Disorders Collaborators. Global, regional, and national burden of 12 mental disorders in 204 countries and territories, 1990–2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet Psychiatry. 2022;9(2):137–50. https://doi.org/10.1016/S2215-0366(21)00395-3
- Mao Q-S, Guo Y-X, Tian X-L, Zhao H-L, Kong Y-Z. Global burden of mental disorders in 204 countries and territories results from the Global Burden of Disease Study 2021. World J Psychiatry. 2025;15(8):106887. https://doi.org/10.5498/wjp.v15.i8.106887
- Altwaijri YA, Al-Habeeb A, Al-Subaie AS, Bilal L, Al-Desouki M, Shahab MK, et al. Twelve-month prevalence and severity of mental disorders in the Saudi National Mental Health Survey. Int J Methods Psychiatr Res. 2020;29(3):e1831. https://doi.org/10.1002/mpr.1831
- Noorwali R, Almotairy S, Akhder R, Mahmoud G, Sharif L, Alasmee N, et al. Barriers and facilitators to mental health help-seeking among young adults in Saudi Arabia: a qualitative study. Int J Environ Res Public Health. 2022;19(5):2848. https://doi.org/10.3390/ijerph19052848
- Alasiri AA, Mohammed V. Healthcare transformation in Saudi Arabia: an overview since the launch of vision 2030. Health Serv Insights. 2022;15:11786329221121214. https://doi.org/10.1177/11786329221121214
- AlShareef SM, AlWabel AA. Patient opinions about virtual consultations in Saudi Arabia: a nationwide cross-sectional study. Healthcare. 2024;12(10):1001. https://doi.org/10.3390/healthcare12101001
- Alshahrani A, Alrajhi A, Al Muaythir E, Zeyad L, Mortada EM. Assessment of telemedicine usage among Saudis during the COVID-19 pandemic. Cureus. 2024;16(1):e53084. https://doi.org/10.7759/cureus.53084
- Almalky AM, Alhaidar FA. Patients’ satisfaction with telepsychiatry services at a University Hospital in Riyadh during the COVID-19 pandemic. Cureus. 2021;13(8):e17307. https://doi.org/10.7759/cureus.17307
- Kaliyadan F, Amin TT, Kuruvilla J, Ali WHAB. Mobile teledermatology–patient satisfaction, diagnostic and management concordance, and factors affecting patient refusal to participate in Saudi Arabia. J Telemed Telecare. 2013;19(6):315–19. https://doi.org/10.1177/1357633X13501778
- Alodhayani AA, Hassounah MM, Qadri FR, Abouammoh NA, Ahmed Z, Aldahmash AM. Culture-specific observations in a Saudi Arabian digital home health care program: focus group discussions with patients and their caregivers. J Med Internet Res. 2021;23(12):e26002. https://doi.org/10.2196/26002
- Albaghdadi AT, Al Daajani MM. Perceptions, satisfaction, and barriers to telemedicine use: a community-based study from Jeddah, Saudi Arabia. Cureus. 2023;15(6):e40738. https://doi.org/10.7759/cureus.40738
- Houser SH, Flite CA, Foster SL. Privacy and security risk factors related to telehealth services—a systematic review. Perspect Health Inf Manag. 2023;20(1):1f.
- Jonasdottir SK, Thordardottir I, Jonsdottir T. Health professionals’ perspective towards challenges and opportunities of telehealth service provision: a scoping review. Int J Med Inform. 2022;167:104862. https://doi.org/10.1016/j.ijmedinf.2022.104862
- Alhraiwil NJ, Al-Aqeel S, AlFaleh AF, AlAgeel AA, AlAbed MA, Al-Shroby WA. Impact of COVID-19 on the 937 Telephone Medical Consultation Service in Saudi Arabia. Int J Telemed Appl. 2022;2022(1):4181322. https://doi.org/10.1155/2022/4181322
- Mao A, Tam L, Xu A, Osborn K, Sheffrin M, Gould C, et al. Barriers to telemedicine video visits for older adults in independent living facilities: mixed methods cross-sectional needs assessment. JMIR Aging. 2022;5:e34326. https://doi.org/10.2196/34326
- Elfaki NK. Perception and challenges of telehealth among healthcare providers in Najran, Saudi Arabia. Bahrain Med Bull. 2024;46(2):2085–8.
- Fleddermann K, Chwastiak L, Fortier A, Gotham H, Murphy A, Navarro R, et al. Levels of telehealth use, perceived usefulness, and ease of use in behavioral healthcare organizations after the COVID-19 pandemic. J Behav Health Serv Res. 2025;52(1):48–63. https://doi.org/10.1007/s11414-024-09902-6
- Burmeister OK, Ritchie D, Devitt A, Chia E, Dresser G, Roberts R. The impact of telehealth technology on user perception of wellbeing and social functioning, and the implications for service providers. Aust J Inform Syst. 2019;23:1501. https://doi.org/10.3127/ajis.v23i0.1501
Copyright Ownership: This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See http://creativecommons.org/licenses/by-nc/4.0. The authors of this article own the copyright.