EDITORIALS AND DISCUSSIONS
AI Enabled Nursing: Moving From Virtual Support to Intelligent Care Redesign
Linda Lockwood, RN, MBA1, Erika Rolland, MSN, RN, RN-BC CAVRN2  , Dominick Pahl, MS, RN, CAVRN3
, Dominick Pahl, MS, RN, CAVRN3  and Sarah Bell, RN, MSN, MHA4
and Sarah Bell, RN, MSN, MHA4
1Senior Advisor, Avia Health, Chicago, Illinois, USA; 2Senior Director Clinical Operations, OutcomesAI, Boston, Massachusetts, USA; 3Senior Director Operations, OutcomesAI, Boston, Massachusetts, USA; 4Chief Clinical Officer, OutcomesAI, Boston, Massachusetts, USA
Keywords: off-load bedside nursing, patient throughput, RN satisfaction, virtual nursing, workflow
Abstract
Virtual nursing has become a critical strategy for health systems in 2025, extending clinical capacity, mitigating burnout, and improving patient throughput. These programs typically focus on “off-loading” bedside nurses by deploying experienced virtual nurses to manage admissions, discharges, monitoring, patient education, and staff mentoring. These programs aim to create gains in efficiency and among registered nurses (RN) satisfaction, yet they lack the ability to prove hard return on investment and focus on offloading rather than redesigning workflow.
The emergence of artificial intelligence (AI) creates the opportunity to move beyond these limitations. This article outlines the transition from task-based virtual nursing to AI-driven models that optimize outcomes and workforce sustainability. All of this while still keeping the nurse at the center of patient care and reimagining a sustainable workforce of the future. To truly evolve nursing, we must integrate intelligence into every workflow, not just relocate the workload.
Citation: Telehealth and Medicine Today © 2026, 11: 669
DOI: https://doi.org/10.30953/thmt.v11.669
Copyright: © 2026 The Authors. This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0.
Submitted: December 2, 2025; Accepted: January 6, 2026; Published: March 31, 2026
Corresponding Author: Sarah Bel, Email: bell.sarahj33@gmail.com
Competing interests and funding: Erika Rolland is a peer reviewer; Dominick Pahl is an editor, and Sarah Bell is Senior Editor on Telehealth and Medicine Today.
None.
The American Nurses Association (ANA) defines virtual nursing as “leveraging remote technology and tools to provide safe and quality patient care through the application of the nursing process, emphasizing communication, compassion, and collaboration throughout the continuum of care.”1 This practice rose to prominence in the early 2000s and had a resurgence during the COVID-19 pandemic as a means to maximize nursing capacity. In 2024, 46% of hospitals were piloting or scaling virtual nursing, with a 34% rise in the adoption of virtual nursing and 74% of hospital leaders saying virtual nursing will become integral to care.2
Despite this rapid growth and belief that virtual nursing can extend the bedside nurses’ capacity, there are flaws in the current design. Firstly, the focus on task-based work rather than true, holistic workflow redesign hinders today’s models. Most programs are built to offload admissions, discharges, patient education, and other tasks from bedside nurses to the virtual nurse. This model does not address the systemic inefficiencies surrounding documentation, communication, and data that exist today. Instead, it simply shifts those responsibilities to a virtual nurse. As a result, the virtual nurse can provide momentary support but lacks the ability to fundamentally change these deeper inefficiencies.
The second limitation includes the technology used for these programs and corresponding system integrations. Virtual nurses rely on video systems and data from electronic health records to complete their workflow. Many health systems lack the integration or quality of devices needed to provide efficient and high-quality virtual care. This reduces efficiency and increases cognitive burden, which impacts the effectiveness of virtual nurses and limits the ability to scale efficiently across health systems.
One final limitation is that virtual nursing relies solely on human clinicians; reassigning experienced nurses to remote roles with unfavorable staffing ratios only deepens shortages at the bedside. This severely limits scalability as virtual nursing programs remain constrained by the same workforce they are intending to help. This staffing challenge puts many nursing leaders in difficult positions, deciding whether to staff the virtual nursing roles or the bedside nursing roles.
Barriers and Foundational Lessons
While enthusiasm for virtual nursing is growing, early implementations reveal significant challenges. In the rush to start, many organizations failed to fully understand the true problem they were trying to solve or to define clear success metrics that could demonstrate progress and value.
Common Foundational Gaps Include
- Failing to define the specific problem virtual nursing is meant to address
- Limited engagement with bedside nurses, skipping critical “listening tours” and unit walk-throughs
- Lack of senior leadership buy-in and sustained sponsorship
- Starting a pilot without a shared vision, guiding principles, or defined workflows
- Underestimating the importance of change management and cultural readiness
- Infrastructure and technology limitations that hinder adoption
- Competing hospital priorities pulling focus away from transformation initiatives
- Fear of embracing new, blended care models enabled by technology
One adoption story was particularly instructive. An Innovation Department introduced continuous monitoring devices across several units. However, without involving nurses in the selection or workflow design, the devices began generating an overwhelming amount of data. Rather than feeling empowered, nurses experienced alert fatigue and frustration, which stalled adoption entirely. The lesson was clear: understanding the “voice of the customer”—in this case the nurses—is essential. When nurses help to define the process, choose the tools, and shape how technology fits into care delivery, adoption accelerates and the technology becomes an ally, not another burden.
These lessons have shaped the next wave of virtual nursing innovation, one that is grounded in clarity of purpose, frontline engagement, and intentional design. With these foundations in place, organizations are now positioned to leverage the emerging enablers that make hybrid, AI-augmented care scalable and sustainable.
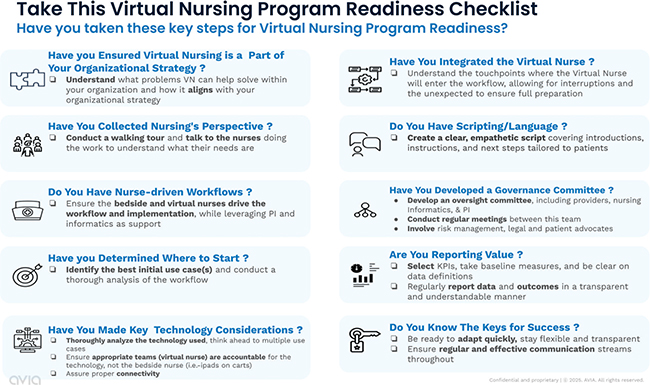
Fig. 1. This virtual nursing Program Readiness Checklist shares a detailed guide of the key elements that are often missed.
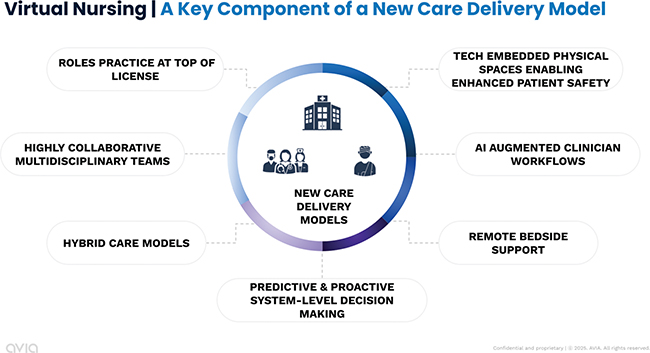
Fig. 2. Virtual nursing is a key component in driving new care delivery models.
The Call for ROI in Virtual Nursing
An emerging priority in virtual nursing is the need to demonstrate clear value and quantifiable return on investment (ROI) to justify technology and staffing expenditures. The ROI should be assessed across multiple domains, including workforce retention, patient satisfaction, and clinical outcomes. Short-term pilots seldom reveal financial benefit; measurable impact typically becomes evident over 12–18 months as programs mature and scale. Virtual nursing generates soft ROI through enhanced nurse satisfaction and patient throughput, and hard ROI through outcomes such as decreased length of stay and reduced readmission rates.
Emerging evidence is promising; a study conducted at the University of North Carolina Kenan-Flagler Business School linked virtual nursing to a 7.18% reduction in length of stay and a 2% drop in 30- and 60-day readmissions.3 According to a 2024 nursing report from New Orleans-based Ochsner Health, over 90% of discharges to home were facilitated by virtual nursing, saving bedside staff time, improving nurse satisfaction, and reducing readmissions by ~2%.4 Similarly, the Houston Methodist’s virtual nursing program tracks metrics including discharge times, length of stay, and nurse/patient satisfaction, with early signals of improved operational and experiential outcomes.5 Additionally, virtual nursing has been associated with improved documentation completeness and task execution, further demonstrating its operational effectiveness.6
Sustained ROI begins with culture and leadership. When executives and nurse leaders position virtual nursing as a core element of hybrid care, and not a project, it creates ownership, accelerates adoption, and builds a foundation for AI- and smart-room–enabled models of the future.
Why a True Care-Model Redesign is Needed
Virtual nursing has created value, but it is constrained by the same workforce issues the model aims to address. Moving forward we must begin to think of virtual nursing as one piece in the puzzle of a hybrid care model that empowers patients and reduces the cognitive load on our nursing and care team members. A true redesign must incorporate people, process, technology, and AI.
AI fills the missing capability to drive care into the future by facilitating early risk detection, predicting readmissions, generating documentation, and surfacing decision support in real time, which has been shown to optimize nurse workload and improve satisfaction and patient outcomes.7 These capabilities enable nurses to transition from a reactive responder to a proactive conductor of care. Evidence from hybrid care models reveals that combining virtual and in-person nursing has measurable improvements in clinical outcomes, including reduced readmissions and higher patient satisfaction.8
Emerging Enablers
If the first wave of virtual nursing focused on extending reach, the next wave is about amplifying capability. AI and machine learning are practical tools shaping the future of care. They can mimic human cognitive functions such as learning, reasoning, and problem-solving at a scale and speed beyond human capacity. In healthcare, AI systems analyze structured data (labs, vitals, medications) and unstructured data (clinician notes, conversations) to detect risks, make predictions, and surface actionable insights. Several converging enablers are driving this shift.
AI-Driven Decision Support
Machine learning and natural language processing can transform data into real-time insights that reduce cognitive load and enhance patient safety. AI-driven virtual assistants provide contextual guidance to nurses by surfacing care protocols, patient information, and actionable alerts directly into workflows.7
Unified Technology Platforms
Modern platforms enable seamless communication between bedside teams, virtual teams, and patients. These platforms increasingly integrate AI voice agents, which understand, interpret, and respond to spoken language while assisting nurses in documentation, task management, and patient interactions.9 When combined, these tools reduce administrative burden and allow nurses to focus on direct patient care.
Smart Rooms
Context-aware patient rooms equipped with sensors, adaptive displays, and voice interfaces capture documentation passively while surfacing alerts, letting nurses focus on human care rather than data entry.
Hybrid Care Model
Integrating virtual and direct care enhances nursing competencies, technological literacy, and workflow optimization, preparing nurses for AI-enabled healthcare delivery.8,10 Studies show that hybrid models improve clinical outcomes, reduce readmissions, and enhance patient satisfaction.6
Together, these enablers set the foundation for a truly AI-augmented, hybrid care model, empowering nurses, improving patient outcomes, and creating scalable, sustainable nursing workflows.
Blueprint for Next-Generation Nursing
Next-generation nursing care requires an integrated architecture that unites human judgment, intelligent automation, and seamless interoperability. Rather than layering technology onto old workflows, this model embeds intelligence into the core of care delivery, which will enhance rather than replace the nurse’s role.
Core elements include multichannel patient interfaces (voice, text, video) that enable frictionless communication, clinical AI engines that analyze structured and unstructured data to surface real-time insights, and interoperability layers that unify information into a single longitudinal record. Collaboration hubs connect bedside and virtual nurses within shared digital workspaces, where automation assists with documentation, task routing, and protocol suggestions.
Data flow through this architecture in a closed loop: signals from patients, devices, and clinicians are continuously collected, analyzed, and transformed into actionable insights. Each intervention feeds back into the system, refining models and improving performance over time.
In practice, this blueprint transforms nursing from a fragmented, reactive model to an intelligent, proactive ecosystem that empowers nurses, improves patient safety, and elevates care outcomes.
Proactive Risk Detection
Models of AI continuously monitor patient data for early signs of deterioration, flagging subtle changes such as shifts in respiratory rate or medication adherence hours before traditional thresholds. Nurses can intervene sooner, preventing complications and costly escalations.
Seamless Multichannel Triage
Patients communicate via their preferred channel—voice, text, or video—while an AI agent structures the encounter, verifies context from the EHR, and routes it to the appropriate clinician or automated pathway. Repetitive data collection is reduced and allows the patient to get to a quicker solution, which enhances experience.
Automated Documentation and Care Coordination
Interactions generate structured documentation automatically via natural language processing and smart templates. Task assignments such as labs, education, or discharge planning are routed directly to the appropriate team member. Care coordination then shifts from reactive to proactive, ensuring nothing falls through the cracks.
Market Signals and Early Pioneers
Case Study: Platform-Based Nurse Staffing and AI Services
Emerging startups are moving beyond telehealth into “nurse concierge” platforms offering services and products that blend human clinicians with AI orchestration. These platforms allow patients to access 24/7 nurse support, backed by decision support engines and automated care coordination. Instead of piecemeal apps, the concierge model creates a unified entry point into the health system, positioning nurses as trusted guides through increasingly complex care landscapes. Early adopters have demonstrated both consumer demand and payer interest, signaling a shift toward models that prize convenience, continuity, and intelligence.
Together, these early signals indicate that the market is already moving from “virtual support” toward intelligent care redesign. Organizations that align with this shift stand to capture not only operational efficiencies but also strategic differentiation in a crowded healthcare landscape.
Challenges Ahead
Despite its promise, the path to AI-enabled nursing will not be without challenges. Data governance and privacy remain paramount, as predictive models depend on sensitive patient information. Health systems must develop governance frameworks that define data ownership, establish access rights, and embed ethical safeguards to ensure compliance with the Health Insurance Portability and Accountability Act (HIPAA) in the U.S. and evolving privacy regulations. While progress has been made with standards such as the Fast Healthcare Interoperability Resources (HL7 FHIR), many EHRs and legacy systems remain siloed, making integration difficult. Without vendor-neutral platforms and universal interoperability, the risk is that AI solutions will proliferate as isolated pilots rather than integrated enterprise systems.
Perhaps the greatest challenge lies in culture and change management. Nurses and clinicians must tealize that these technologies are implemented in partnership with them, rather than imposed on them or even passed onto them. Robust training, transparent communication of value, and leadership engagement at every level are required. Health systems that neglect the cultural dimension risk creating resistance or burnout, even with the best technical tools. Ultimately, successful adoption will hinge as much on workforce development and change leadership as on the algorithms themselves.
Conclusion
AI-enabled virtual nursing represents the next evolution of care delivery, moving beyond task-based offloading toward an integrated, proactive, and scalable hybrid model. Embedding intelligence into workflows and harnessing AI for risk detection, triage, documentation, and decision support, while integrating multichannel communication and smart environments, empowers health systems to advance patient safety, boost nurse satisfaction, and drive operational in cultural transformation and technological capability will define the future of AI-enabled nursing. Realizing this vision requires deliberate design, frontline engagement, cultural readiness, and phased implementation. With these foundations in place, organizations can create sustainable nursing models that empower staff, improve outcomes, and position themselves at the forefront of the rapidly evolving healthcare landscape.
Contributions
The authors collaborated on each aspect of the project and manuscript preparation.
Data Availability Statement (DAS), Data Sharing, Reproducibility, and Data Repositories
None.
Application of AI-Generated Text or Related Technology
AI was utilized for proofing the manuscript.
Acknowledgments
The authors wish to thank the following leaders for sharing their insights and experiences, which greatly informed this work: Maura Nazario, MSN, RN, SANE, VP CNO at AdventHealth; Rachelle Longo, RN, AVP Telemedicine at Ochsner Health; Kaitlyn Torrence, Executive Director of Innovation at Wellspan Health; and Peggy Norton-Rosko, RN, CNO at University of Maryland Health System. Their perspectives on virtual nursing, hybrid care models, and AI integration provided invaluable context and practical guidance.
References
- American Nurses Association. Principles of virtual nursing [Internet]. 2025. Available from: https://www.nursingworld.org/globalassets/docs/ana/ethics/principles-of-virtual-nursing.pdf
- Siwicki B. 74% of hospital leaders say virtual nursing will become integral to acute care [Internet]. Healthcare IT News. 2024 [cited 2026 Nov 23]. Available from: https://www.healthcareitnews.com/news/74-hospital-leaders-say-virtual-nursing-will-become-integral-acute-care
- Liu B, Xu Y, Staats BR. Bridging the nursing gap: How virtual nurse adoption impacts patient outcomes [Internet]. SSRN Scholarly Paper No. 5213142. SSRN. 2025 [cited 2026 Nov 23]. Available from: https://ssrn.com/abstract=5213142
- Ochsner Health. Ochsner Health Nursing Annual Report 2024 [Internet]. 2024 [cited 2026 Nov 23]. Available from: https://ochsner-craft.s3.amazonaws.com/doctors/Ochsner-Health-Nursing-Annual-Report-2024.pdf
- Wicklund E. Houston Methodist is playing the long game with virtual nursing. HealthLeaders Media. 2024 [cited 2026 Nov 23]. Available from: https://www.healthleadersmedia.com/innovation/houston-methodist-playing-long-game-virtual-nursing
- Khairat S, Morelli J, Aucoin J, Edson BS, Jones CB, Shea CM. Association of virtual nursing and task completeness: An observational study. SAGE Open Nurs. 2025;11:23779608251363667. https://doi.org/10.1177/23779608251363667
- Rony MKK. Advancing nursing practice with artificial intelligence. Nurs Manage. 2023;50(3):45–52. https://doi.org/10.5678/nm.2023.50345
- Rezilient Health. 2024 Clinical outcomes report [Internet]. 2024. Available from: https://www.rezilienthealth.com/resources/2024-clinical-outcomes-report
- Stark Digital Media Services. AI voice agents in healthcare: Transforming the patient journey [Internet]. 2025 [cited 2026 Nov 23]. Available from: https://www.starkdigital.net/ai-voice-agents-in-healthcare/
- Innovation Advantage. 2024.
Copyright Ownership: This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0.